Breakout 1.2 Assessing competence in practice: Quality assured diagnostic spirometry - Monica Fletcher
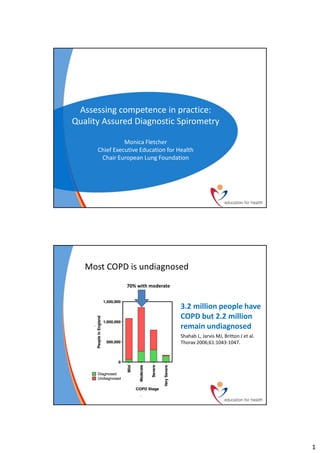
- 1. Assessing competence in practice: Quality Assured Diagnostic Spirometry Monica Fletcher Chief Executive Education for Health Chair European Lung Foundation Most COPD is undiagnosed 70% with moderate 3.2 million people have COPD but 2.2 million remain undiagnosed Shahab L, Jarvis MJ, Britton J et al. Thorax 2006;61:1043-1047. 1
- 2. www.rightcare.nhs.uk/index.php/atlas/respiratorydisease/2012 • 20% GP consultations are for respiratory problems • GPs manage the majority of patients with airways disease • Nationally about 25% on primary care COPD registers not meeting diagnostic criteria • West London study verifying diagnosis of COPD using a centralised diagnostic service for primary care found 36% misdiagnosed & therefore on inappropriate treatment 1 • Several studies have also demonstrated that asthma is also frequently over diagnosed or misdiagnosed2,3,1 Starren et al (2011) PCRJ 2. Linden Smith et al (2004) 1. CanRJ 3.Aaron et al (2008) CMAJ 2
- 3. Does late diagnosis matter in COPD? • Lung function declines progressively, but evidence this is more rapid than we thought in early stages of the disease,1,2 • Exacerbations are common even in moderate disease (22% GOLD stage 2 )3 • Quality of life, physical & social function are significantly reduced in all stages of disease from mild to severe4 • 44% of people with COPD in the UK are of working age: over half are prevented from working at all and a quarter limited in their ability to work – lost personal & societal income Decramer M, et al (2009) Effect of tiotropium on outcomes in patients with moderate chronic obstructive pulmonary disease (UPLIFT): DOI:10.1016/S0140-6736(09)61298-8 Lancet , (2009)2 Jenkins CR, et al. TORCH study. Respir Res 2009;10:59 3. Hu rst J, et al. Susceptibility to Exacerbation in Chronic Obstructive Pulmonary Disease. NEJM 2010;363(12):1128-38. 4;Miravitlles M, et al. Prevalence of COPD in Spain: impact of undiagnosed COPD on quality of life and daily life activities. Thorax 2009;64:863-8. How late is “late” diagnosis? • A recent Canadian study found that 21% of those with undiagnosed COPD had severe or very severe disease1 • NCROP audit 2008 – Nationally 10% of emergency COPD admissions were undiagnosed 2 • London study 2011 - 34% admissions were undiagnosed and one fifth of the undiagnosed patients were in respiratory failure 3 1HillK, et al. Prevalence and underdiagnosis of chronic obstructive pulmonary disease among patients at risk in primary care CMAJ 2010;182:673-8 2. Royal College of Physicians, BTS, BLF. Report on the National Clinical COPD resources outcomes Project RCP 2008 3. Bastin A, et al. High prevalence of undiagnosed and severe chronic obstructive pulmonary disease at first hospital admission with acute exacerbation. Chronic Respiratory Disease 2010;7(2)91-7. http://dx.doi.org/10.1177/1479972310364587 3
- 4. Missed opportunities in primary care 38,000 patients, 2 years prior to diagnosis: • Over half (56%) had two or more consultations for lower respiratory tract complaints • 27% had four or more consultations for lower respiratory tract infections • One third of these received two or more prescriptions for steroids and or antibiotics Price D, Halpin D, Winter D et al. Missed opportunities to diagnose COPD. Oral Presentation European Respiratory Society Conference. 2011 Impact of Inaccurate Spirometry results: Costs to the individual • Diagnosis : be it wrong, inaccurate and correct diagnosis (COPD, asthma, other diagnosis) • Psychological impact on individual and family • Disability and/or work issues • Life insurance • Inappropriate and expensive ongoing treatments (with potential side effects) • Further tests or investigations 4
- 5. Inaccurate spirometry results: Healthcare costs • Under or over treatment or no treatment including inappropriate, expensive therapies • Inappropriate referrals • Further unnecessary investigations • Wrong labeling on practice registers / QOF: Follow up and recall An estimation of cost of misdiagnosis (Based on a rate of 25%) Approx £28.5m Total Stage % number Cost of annual Total cost misdiagnosed total medication per per year (COPD pts) patient 835,000 mild 53% 110,637 £80 £8,850,960 known 25%=208,750 moder 39% 81,412 £137 £11,153,444 ate severe 8% 16,700 £514 £8,583,800 TOTAL £28,588,204 5
- 6. • The diagnosis and assessment of respiratory disease requires accurate measurement of lung function (along with clinical history taking and physical examination) • The most widely used test of lung function is SPIROMETRY • Many options which are: affordable, easy to use, reliable, portable desktop hand held options providing reference values & computer generated interpretation “Yet high quality spirometry continues to prove difficult to implement in primary care” (and other settings!) Jenkins C (2009) Editorial Primary Care Respiratory Journal 18(3)128-129 The UK Quality & Outcomes Framework (QOF) pay for performance scheme & spirometry Strong M et al (2009) BMC Health Services Research • QOF Introduced in 2003 to improve Quality in general practice • In 2006/07 practices in Rotherham achieved 94.5% indicators (national average 96%) • 3217 patients randomly selected from 5,649 patients with COPD from 38 GP practices in Rotherham • Only 31% met BTS standards (3 consistent readings 2 within 100mls) and 12% not consistent with COPD diagnosis Quality Outcomes Framework is rewarding the QUANTITY not QUALITY of spirometry Substantial variation in performance and interpretation 6
- 7. How can we ensure earlier diagnosis? Opportunistic assessment: • Smoker or ex smoker over 35 • Symptoms such as breathlessness, chronic cough, regular sputum production, frequent winter “bronchitis” and wheeze Systematic case finding by audit of GP register • Symptomatic patients with airflow obstruction • E.g. smokers or ex-smokers not known to have COPD or asthma with history of recurrent respiratory symptoms or infections or treatment with inhalers Quality assured diagnostic spirometry • Ensuring the diagnosis is correct What can go wrong with spirometry in the community setting? Equipment • Fully functioning, calibration, regular Patient serviced….. • Ill prepared • Poor technique, effort • Posture …. Operator • Competence, training, motivated, lack of time, conscientious, poor instructions……. Environment • Temperature, privacy, distraction, hygiene….. 7
- 8. Misbelief Simple test Minimum skill required Clinical Experience : A definition Making the same mistakes with increasing confidence over an impressive number of years 8
- 9. A Guide to Performing Quality Assured Diagnostic Spirometry In publication by DH Assessing Quality Assured Spirometry 9
- 10. A Guide to Performing Quality Assured Diagnostic Spirometry 1. Calibration and cleaning 2. Preparation of the patient 3. Performance of the test 4. Interpretation of results 5. Reporting – top ten tips 6. Common technical errors 7. Quality assurance 8. Ensuring competency Performing Quality Assured Diagnostic Spirometry in clinical practice: Assessing competence in those performing and interpreting the test* *currently being formalised 10
- 11. Who should diagnose respiratory conditions Diagnosis should be made by a qualified medical practitioner or an appropriately trained nurse or AHP The diagnosis of most common respiratory disorders is based on – comprehensive clinical history – physical examination – relevant additional tests e.g. FBC, CXR – Diagnostic spirometry Who should perform quality assured diagnostic spirometry • Spirometry may be performed by a range of practitioners who may not be qualified HCPs BUT the interpretation should only be carried out by a qualified HCP or clinical physiologist • Because spirometry is a practical procedure, assessment of competence is critical • Quality Assured Diagnostic Spirometry should only be performed in a clinical setting by individuals who have been assessed to the standards established by the ARTP otherwise the accuracy of the diagnosis cannot be relied upon 11
- 12. Delegation of tasks • Professionals responsible for Quality assured diagnostic spirometry have a duty to ensure that they and the staff they manage have the necessary skills and competence to undertake the procedure in accordance with the nationally agreed standards. • This includes GPs delegating to practice nurses and practice nurses delegating to HCAs So what is the plan? • Inexperienced staff will attend an approved training programme and 1 on successful completion will be entered onto a register • Practitioners undertaking a current ARTP approved training programme 2 will be entered on to a register on successful completion of the course • Practitioners already on a register will remain on the register for 3 3 years and will then be reassessed • Experienced staff may have direct entry to a register by submitting a portfolio of tests to a recognised assessment centre and upon meeting 4 the qualifying criteria will be entered on to the register • Very experienced staff may be able to access the register directly 5 through an equivalence process * To be determined 12
- 13. Evidence for the need for training – ‘good quality spirometry from trained and experienced staff provides more robust and reliable results than office testing’ (Lange et al. Respir Med 2009) – Nurses who have undertaken a COPD diploma module were more confident in interpreting spirometry than those who had not undertaken the training 53% v 12% (p<0.001) (Davison BTS abstract 2012) • Spirometry in Primary Care Practice – 30 primary care clinics, Comparison 3.4% in usual group v 13.5% in trained group (15 of each) met ATS acceptability and reproducibility criteria (Eaton et al, Chest 1999; 116:416-423) – Only 12% of nurses performing spirometry had received accredited training. (Upton et al. PCRJ 2007) Existing training programmes • Need to explore opportunities to broaden certification opportunities for all HCP including doctors, during their training programmes both GPs and Specialist Registrars. • Practice nursing programmes and other nursing courses • Pharmacists 13
- 14. Improving primary care Spirometry Francis Report : • QOF & local enhanced ‘ there needs to be a clear set of services fundamental standards of care • Cost savings to be had which are backed by evidence, • Satisfaction clinically informed and enforced by • Professionalism a clear regulatory regime’ • Excellence in care: PCRS Quality Award Care Quality Commission • Improving Quality In Commissioning processes Physiological diagnostic Certification courses and Services: IQIPs individuals Registration of individuals During the first half of2013 will draw up detailed plans and processes. So we can start to implement and roll out Later in the year LIFE AND BREATH FOR THOUSANDS OF PATIENTS! 14
