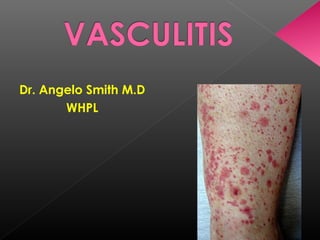
Vasculitis
- 1. Dr. Angelo Smith M.D WHPL
- 2. • Affects all ages, although some types are restricted to certain age groups • Tends to affect Caucasians, although many African-Americans are affected • Has a genetic component, but is not heritable • It is a chronic relapsing disease, although some patients experience prolonged remission
- 3. Inflammatory destruction of blood vessels •Infiltration of vessel wall with inflammatory cells – Leukocytoclasis – Elastic membrane disruption •Fibrinoid necrosis of the vessel wall •Ischemia, occlusion, thrombosis •Aneurysm formation •Rupture, hemorrhage A clinicopathologic process characterized by inflammatory destruction of blood vessels that results in occlusion or destruction of the vessel and ischemia of the tissues supplied by that vessel. “Systemic vasculitides” Definition
- 5. 1. Unexplained signs and symptoms 2. Multisystem involvement 3. Unexplained elevated ESR/CRP 4. Skin lesions (palpable purpura) 5. Ischemic vascular changes (Raynaud’s, gangrene, livedo, claudication) 6. Glomerulonephritis 7. Mononeuritis multiplex 8. Intestinal angina 9. Inflammatory ocular disease 10. Arthralgia's/arthritis, myalgia's 11. Sudden visual loss/headache
- 7. 1. Fatigue 2. Weakness 3. Fever 4. Abdominal pain 5. Proteinuria , hematuria , casts 6. Nerve problems (numbness , weakness) 7. Skin rash
- 9. Based on › Size of Vessels involved › Site of involvement › Characteristic Features
- 12. • Large-vessel vasculitis – Giant cell arteritis, Takayasu’s arteritis – Behcet’s disease, Cogan’s syndrome • Medium-vessel vasculitis – Polyarteritis nodosa – Buerger’s disease, Central nervous system vasculitis, Kawasaki’s disease, Rheumatoid vasculitis • Small-vessel vasculitis – Wegener’s Granulomatosis , microscopic polyangiitis, Churg-Strauss (ANCA associated) – Cryoglobulinemic vasculitis, Henoch- Schönlein purpura (Non ANCA associated)
- 16. Can occur exclusively but often seen with PMR Rare: 15/100,000 Age >50 Cause unknown Involves the medium/large blood vessels of the head and neck including the blood vessels that supply the optic nerve
- 17. Unknown trigger causes inflammatory response with the release of IL-1 and IL-6. This leads to systemic symptoms and the infiltration of inflammatory cells into the adventitia of the temporal and other involved arteries Typical histologic pattern: Giant Cells
- 20. Temporal Artery Biopsy is the gold standard Elevated ESR and CRP, usually levels higher than in PMR Anemia Elevated LFTs not uncommon
- 21. High dose Steroids (60 mg/day) is the only drug that works Slow taper over time usually 1-2 years. Some patients require low dose (<10 mg/day) chronically
- 22. Blindness Scalp Necrosis Lingual Infarction Aortic Dissection/Aneurysm Complications from high dose steroids: osteoporosis, cataracts, elevated blood sugars, wt. gain etc.
- 26. 70 %
- 29. Pathergy- An erythematous papule larger than 2 mm at the prick site 48 hours after the application of a 20- to 22-gauge sterile needle, which obliquely penetrated avascular skin to a depth of 5 mm as read by a physician at 48 hours
- 30. Medium vessel vasculitis Can be caused by Hep B 5/million cases Peak incidence 50’s & 60’s, slightly more common in males
- 31. In Hep B assoc cases immune complexes play significant role In non Hep B cases, the pathophysiology is less understood
- 32. • Systemic: fever, fatigue, wt loss • Abdominal pain due to mesenteric angina/ischemia • Mononeuritis multiplex • Myalgias/arthalgias/mild arthritis • Renal: uremia, Hypertension • Skin: livedo reticularis, palpable purpura, fingertip ulceration, subcutaneous nodules • Testicular pain or tenderness
- 35. Chronic renal failure Bowel perforation Stroke/cerebral hemorrhage due to HTN Foot/wrist drop
- 36. Elevation of acute phase reactants (ESR, CRP etc) Absence of ANCA Elevated transaminases, decreased albumin +/- Hep B Urine: proteinuria and hematuria without casts
- 37. Mesenteric and/or renal angiography is the test of choice Biopsies seldom done STRING OF PEARLS
- 38. High dose steroids and Cyclophosphamide Methotrexate or Azathioprine is used as steroid sparing agents later once the disease is controlled Treatment for Hep B with antivirals. Sometimes plasma exchange is used to remove immune complexes
- 45. Necrotizing Granuloma Hypereosinophilia •Sinusitis •Subglottic stenosis •Pulmonary nodules •Orbital pseudotumor •Asthma •Pulmonary infiltrates •Myocarditis •Pulmonary capillaritis •Glomerulonephritis •Sensory neuropathy •Mononeuritis multiplex
- 46. Potentially fatal vasculitis involving small vessels Rare: 3-14/million, more common in whites, any age but rare in children Pathology shows necrotizing granulomas usually in upper airways, lungs and kidneys
- 47. SADDLE NOSE
- 48. • Variable, multisystem involvement
- 51. Presence of c-ANCA (cytoplasmic staining pattern antineutrophil cytoplasmic antibodies + clinical picture is often enough to make the diagnosis. It is + 80-90% of generalized WG. Tissue biopsy of lung or kidney Elevated CRP and ESR Anemia, leukocytosis, & thrombocytosis Elevated Cr Active urine sediment with red cell casts, hematuria and proteinuria
- 52. Prior to immunosuppression therapies, WG was uniformly fatal. Now survival rates almost 90% with aggressive treatment. High dose steroids and Cyclophosphamide are cornerstone of therapy. Methotrexate or Azathioprine sometimes used as steroid sparing agents.
- 58. No specific diagnostic laboratory markers exist The plasma coagulation factor XIII is reduced in about 50% of patients Urinalysis reveals hematuria. Proteinuria may also be found CBC can show leukocytosis with eosinophilia and a left shift. Thrombocytosis is present in 67% of cases Serum IgA levels are increased in about 50% of patients during the acute phase of illness The antistreptolysin O (ASO) titer is elevated in 30% of cases
- 59. • Remission induction: – Cyclophosphamide 2mg/kg po qd x 3-6 months [or 15 mg/kg IV q 2 wk x3 then q 3 weeks x 6-12 months] – Prednisone 1mg/kg po qd x 1 month, then taper – [Bactrim, Calcium, Vitamin D] • Remission maintenance (minimum 2 years) – Methotrexate 20-25 mg po q week + folate – Azathioprine 2mg/kg po qd – Mycophenolate mofetil 1.5 g po BID – Leflunomide 20-30 mg po BID
- 63. • Large-vessel vasculitis – MRI/MRA chest/abdomen/pelvis every 6-12 months • Medium-vessel vasculitis – Mesenteric angiogram to assess disease activity – EMG/NCV to monitor nerve damage – Wound care for cutaneous ulcers • Small-vessel vasculitis – Chest CT every 6-12 months – Blood and urine tests every 1-4 weeks
- 65. • Large-vessel vasculitis – Blindness, Stroke – Claudication: “Angina” of the arms • Medium-vessel vasculitis – Foot drop: inability to lift a foot – Wrist drop: inability to lift a hand – Cutaneous ulcerations • Small-vessel vasculitis – Oxygen dependence – Renal insufficiency/failure