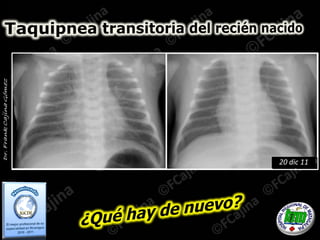
Taquipnea transitoria del recién nacido: Que hay de nuevo?
- 1. 20 dic 11
- 2. Dra. Mary Ellen Avery YEAR OF BIRTH / DEATH 1927 – 2011 MEDICAL SCHOOL The Johns Hopkins University School of Medicine LOCATION Massachusetts CAREER PATH Pediatric medicine Avery ME, Gatewood OB, Brumley G. Transient tachypnea of the newborn: Possible delayed resorption of fluid at birth. Am J Dis Child. ©1966 ;111:380–85.
- 3. Epidemiology Epidemiologic data are scarce, but studies show that TTN occurs in 3.6 to 5.7 per 1,000 term infants. Retention of fetal lung fluid may be more common in preterm infants (up to 10 per 1,000 births), but there usually are coexisting problems such as respiratory distress syndrome (RDS) that may mask its presenta- tion. TTN is one of the most common causes of neonatal respiratory distress, and actually may be underdiagnosed. Risk factors for TTN include birth by cesarean section with or without labor, male sex, family history of asthma (especially in mother), lower gestational age, macrosomia, and maternal diabetes. Guglani L, et al. November 2008;29(11):c59-c65.
- 4. Epidemiology For babies born by elective cesarean section, the pre- sence of labor and the timing of delivery significantly affect the presence of respiratory morbidity. The incidence of respiratory morbidity in babies delivered by cesarean section before the onset of labor is 35.5 per 1,000, compared with cesarean section with labor, in which the rate is 12.2 per 1,000. With vaginal delivery, morbidity occurs in 5.3 per 1,000 births. Even late preterm delivery (between 34 and 37 weeks of gestation) increases the risk for TTN. A significant reduction in respiratory morbidity can be achieved if elective cesarean section is performed after 39 weeks of gestation. Guglani L, et al. November 2008;29(11):c59-c65.
- 14. Patients were randomized in a blinded manner to receive one nebulized dose of either 0.9% normal saline solution 4 mL (placebo), or a solution of salbutamol 4 mL (Ventolin Nebules 2.5 mg) in 0.9% saline solution. The standard dose of salbutamol was 0.15 mg/kg. Solutions were given with a jet type nebulizer with continuous flow of oxygen at 5 to 6 L/min. One dose was administered over the course of 20 minutes, and vital signs were monitored for 4 hours.
- 16. Fluid restriction was defined as 60 mL/kg/day on DOL 1 for preterm neonates and 40 mL/kg/ day on DOL 1 for term neonates. Typically, total fluid was increased by 20 mL/kg/day daily for all patients until 150 mL/kg/day or ad libitum feeding was achieved.
- 18. Objective: Identify perinatal risk factors for transient tachypnea and pneumonia in neonates, and compare the outcome of these clinical conditions during the Neonatal Intensive Care Unit (NICU) stay. Methods: Retrospective review of newborns admitted to a level III NICU, comparing patients with transient tachypnea, pneumonia and a control group of healthy neonates. Results: We included 202 patients with transient tachypnea, 29 with pneumonia and 498 controls. Perinatal infectious risk factors were more frequent in patients with pneumonia than in transient tachypnea (p < 0.001), but the two were identical in terms of the remaining perinatal variables. Patients with pneumonia were admitted for a longer period (p < 0.001) and required supplemental oxygen and ventilatory support more frequently and for a longer period. Comparing with controls, Apgar score at one and five minutes was higher in controls than in patients with pneumonia (p0.032 and p < 0.001) or transient tachypnea (p < 0.001 and p < 0.001). Conclusion: In most cases, newborns with transient tachypnea and pneumonia are indistinguishable at presentation but clinical evolution is significantly different. The presence of perinatal infectious risk supports the diagnosis of pneumonia. Low Apgar score at one and five minutes was associated with both diseases, suggesting that etiologic factors may already be present at birth.
