Varicose Veins
- 1. Varicose veins and treatment • Jeannouel van Leeuwen , surgeon • Chirurgen Maatschap Emma Care • Courtesy of Servier • 25 january 2012
- 2. What we‟ll cover • Some Definitions • Anatomy • What are you looking for? • Examination techniques • Treatment options
- 3. Incidence • annual incidence of varicose veins is about 2% • life-time prevalence of varicose veins approaches 40% • Varicosities are more common in women (about 2-3 times as prevalent in women than in men) • 10-20% actually are symptomatic enough to complain about their lower leg varicose veins and seek treatment.
- 4. What is a varicose vein? • Long, tortuous and dilated vein of the superficial varicose system • Commonly legs but where else? • Abdominal Wall • Anus • Vulva • Oesophagus • Scrotum
- 5. Why do they happen? • increased pressure in the superficial venous system • normally blood flows from superficial system to deep • if the valves protecting the superficial veins become incompetent there is higher pressure in the superficial veins and they become varicose
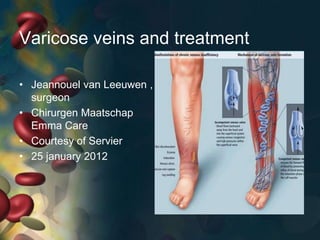
- 6. Normal venous flow in the Leg Normal Flow • Superficial veins drain into the deep veins •From the foot up to the heart Superficial vein disease always starts with abnormal valves and interruption to normal flow called venous reflux
- 8. Abnormal flow = Venous Reflux Damaged Valves 1. Blood flows to the skin 2. Blood is pushed distally and proximally 3. Close loop recirculation 4. Blood is retained in the leg • Increased volume of blood (heaviness Fatigue) • Increased venous pressure • Veins Dilate (varicose veins)
- 9. Taking the history Presenting Complaint: Varicosities, abdominal/groin lump – saphena varix Symptoms Localized discomfort in the leg, Pain, Swelling, Venous claudication, Itching “Risk” factors Female, age, ethnicity, occupation, pregnancy, obesity, sm oking ASK about history of abdominal complaints/cancer, DVT, previous & other venous complaints
- 10. So the examination • Inspection • Auscultation • Palpation • cough test • tap test • Tourniquet Tests • Trendelenberg • Tourniquet test • Perthes • Doppler • Sapheno-femoral junction • Sapheno-popliteal junction
- 11. Diagnosis of venous disease • Physical exam • Appearance • Trendelenburg test • Palpation • Hand Doppler • Duplex Examination • R/O DVT • Size of veins • Map out superficial veins • Locate the site of reflux • Reflux 0.5 sec in GSV and 1 sec in deep system • Find refluxing perforators
- 12. Clinical picture - symptoms • Cosmetic disfigurement • Pain and discomfort • Night cramps • Mild swelling at night • Pigmentation • Itching • Ulceration
- 13. Anatomy • Superficial System arises from foot and ends at Sapheno- femoral junction (spiderhead) • Long saphenous vein- medial leg up to SFJ • Short saphenous vein- lateral malleolus , up calf to meet popliteal vein behind knee • Sapheno- femoral junction- 4 cm lateral and 4cm below the pubic tubercle • Communication veins: connecting deep and superficial system through piercing deep fascia, with valves to direct blood from superficial to deep viens. • Perforator veins: there are 3 perforators on the medial side and 1 on the lateral side of the leg
- 15. Inspection- other features 1. Spider Veins- blueish vessels that distend above the skin surface 2. Thrombophlebitis- superficial red painfull lump 3. Brown pigmentation- haemosiderin deposition 4. Venous Eczema 5. Venous Ulcers- over medial ankle 6. Lipodermatosclerosis-progressive sclerosis of cutaneous fat- ankle becomes thin and hard- area above becomes oedematous 7. Scars from previous surgery
- 17. Atrophy blanche Ulceration: active and healed Inspection Leaves a white patch Venous ulcers/eczema Pitting oedema Spider veins
- 18. Inspection Lipodermatosclerosis Literally "scarring of the skin and fat“ A slow process that occurs over a number of years and has 2 phases: 1. Acute Venous pooling →chronic venous hypertension RBC forced into surrounding tissue Haemoglobin broken down into brown haemosiderin 2. Chronic Chronic haemosiderin formation leads to fibrin deposition Skin becomes thickened and shiny Skin around ankle constricts and the inverted champagne-bottle shape is seen
- 19. Stages of chronic venous insufficiency (Expert meeting in Moscow, 2000.) • 0 - no symptoms; • 1 - heavy feet syndrome; • 2 - intermittent edema; • 3 - persistent edema, hyper- or hypopigmentation, lipodermatosc lerosis, eczema; • 4 - venous ulcer.
- 21. Causes Primary • Theories of Aetiology: • Weak wall theory • Congenital valvular incompetence • Aggravating factors: • Female sex • High parity • Occupation requiring prolonged standing • Marked obesity • Constricting clothes • Estrogen intake • Deep venous thrombosis
- 22. Secondary Anything that raises intra-abdominal pressure or raises pressure in superficial/deep venous system so…: •Pregnancy •Abdominal/pelvic mass •Ascites •obesity •constipation •thrombosis of leg veins (DVT) •AV fistula •Vena cava thrombose •Large liver cysts
- 23. Auscultation • Auscultate over any varicosities for bruits • due to A-V malformation
- 24. Palpation • Palpate the veins to confirm they are infact veins- will refill if if gently pressed and released • Next- find the sapheno-femoral junction (SFJ) • Find Pubic Tubercle just lateral to pubic symphisis • 4 cm lateral then 4cm below • Palpate for a sapheno varix- localised distension of the long saphenous vein in the groin • Cough Test- Fingers over SFJ, ask patient to cough can you feel a thrill, if yes suggest incompetence • Tap Test- tap over the SFJ and feel further down long saphenous vein for any transmitted sounds, if yes suggest incompetence
- 25. Trendelenberg/Tourniquet tests Aim- to localise the valve/s that are incompetent Trendelenberg • Lie patient down and raise leg attempting to drain varicosities of blood. • Using either a tourniquet or fingers put pressure over SFJ to occlude it • Ask patient to stand If varicosities DO NOT refill indicates SFJ incompetence If DO refill the leaky valve is lower down „I will now try and locate the incompetent perforator using the tourniquet test‟
- 26. Tourniquet test continued • Same as before- lie down, raise and drain leg • Place tourniquet approximately over area of each perforator( mid thigh, sapheno popliteal, calf perforators) • If varicosities DO NOT refill that perforator is incompetent • If varicosities DO refill continue down leg
- 27. To complete my examination I would like to… • Perform a full Abdominal Examination • Scrotal examination ( on males!) • Arterial Examination Investigations • Duplex Ultrasonography- maps valve incompetence • Phlebography not done anymore
- 28. Spider Veins The proper term is Telangiectasia •These are non raised dilated veins located in the Dermis (deep layer of the skin) •Single layer endothelium, minimal muscle •Can be Red or Blue in color depending on the origin •Do not cause major medical complications •Appears earlier than varicose veins (4% of teenagers , and 13 % in 18 to 20 year olds •More common in females •Reticular Veins are lager feeding veins
- 29. Spider Veins Etiology: Multifactorial • Venous Hypertension associated with varicose veins • Congenital: vascular nevi, neonatal hemangiomatosis, others.. • Collage Vascular Disease: lupus, • Hormonal factors: pregnancy, estrogen therapy, topical steroids • Trauma: contusion, incisions • Infections
- 30. Venous Stasis Ulcers • Differential Diagnosis 1. Venous ulcerations 50% on non healing ulcers 2. Arterial ulcers in about 10% 3. Malignancy : basal and squamous cell, lymphoma 4. Infections: HIV, fungal 5. Collagen vascular disorders: Lupus ec. 6. Lymphatic obstruction • Affects over 1 million people in the US • 100,000 are disabled from this • More common in elderly population
- 32. Venous Stasis Ulcers • Etiology 1. Venous Hypertension • Venous reflux • DVT • Varicose veins 2. Edema 3. Biological factors • Leakage of proteins impedes diffusion O2 • Aggregation of white cells • Block capillary flow • Release on inflammatory proteins
- 33. Management Surgical Conservative/Medical • Ankle-to-groin saphenous vein Graded compression stripping (with stab avulsion) bandaging, Compression • Segmental saphenous vein stripping hosiery (with stab avulsion) • Saphenous vein ligation: Paste Gauze (Unna) Boots high, low, or both Diuretics? Zinc? • Saphenous vein ligation and Phlebotrophic/Hemorheologi sclerotherapy c agents? Aspirin/NSAIDs etc • Saphenous vein ligation (with stab avulsion) • Stab avulsion of varices without saphenous vein stripping (phlebectomy) • Endoluminal occlusion of the saphenous vein by radiofrequency (RF) or laser energy
- 34. Surgical ligation and Stripping • Standard treatment for a century • General anesthesia • Pain • Long recovery • Some complications • Good cosmetic results
- 35. Surgical treatment • Crossectomy or/and vein stripping till below knee better than compressive therapy alone • Other techniques : Endovas.burning or foam injection
- 36. Vein Ablation • Laser Ablation (EVLA ) • Uses light to heat the vein • Radio Frequency (VNUS Procedure) • Uses radio frequency to heat the vein • Office based procedure • Done under local anesthesia • One needle puncture at the level of the knee • Takes about 1 hour • Patient resumes normal activity same day
- 37. EVLA Results Images from http://venacure-evlt.com/
- 38. Sclerotherapy • Cumulate vein with needle • Inject Sclerosing Solution • Ethoxysclerol • Hyper tonic Saline • Foam (Mix STS with air and make bubbles) • Intravenous injection causes intima inflammation and thrombus formation
- 39. Sclerotherapy Use • Neovascularization • Perforators • Clean up after Phlebectomies • Spider veins • Reticular veins • GSV: can closure the, but has high recurrence rate
- 41. UNNA boot result • Weekly change with UNNA boot bandage gives nice result
- 42. • Compressive bandages first choice with simple small vein ulcer
- 43. • Skin grafting can be put on a non infected granulating skin defect of a venous ulcer
- 44. Treatment complications • Major complications following VV surgery are relatively rare • Up to 20% morbidity • Infection • Hematoma • Pain • Nerve damage • Saphenous nerve (LSV surgery) • Sural, peroneal nerve (SSV surgery) • Lymphatic leak - Venous thrombosis - Vascular injury • Recurrence
- 45. Oral medication • Effect on edema , hematocrit , augmentation capillary permeability , inflammation , less fibrinolysis , leukocyte function en erythrocytes • No evidence for monotherapy only in addition effect on ulcer healing • Daflon , Trental , Aspirine
- 46. Рhlebotropic drugs • Daflon • Venal • Venoruton • Doxium
- 47. Rheologic hemocorrectors • acetylcalicylic acid, • dipiridamol • pentoxyphylline • low-molecular dextranes
- 48. Thank you for your attention www.surgerycuracao.com www.curacaoveininstitute.com Chirurgen Maatschap Curacao www.cmc.an
