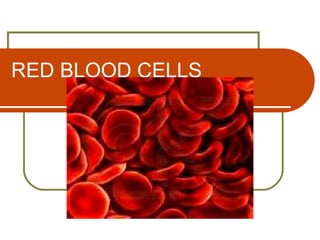
Erythocyte
- 2. Three Phases of an Erythrocyte Life A) Erythropoiesis or Erythrocyte Production B) Release from Bone Marrow to Circulation C) Destruction and Death
- 3. RBC Materials needed for Red Blood Production a) Metals e.g. Copper, Iron, Cobalt, Zinc b) Vitamins e.g. Thiamine, Folate Cyanocobalamin c) Amino Acids e.g. Glutamic, Lysine, Leucine d) Hormones e.g. Erythropoietin, Androgen
- 4. RBC Erythrokinetic Evaluation states that Red Cell Production is equal to Red Cell Destruction Erythrocyte Kinetics ( M = P x S) M - Total Erythrocyte Mass P– Production ( Number of New RBC produced per day) S – RBC Life Span
- 5. Erythrocyte Kinetics Ex: A 70 kg man with 2 liters of Erythrocyte must produced 20 ml of new erythrocytes each day to replace the 20 ml. normally lost RBC due to cell senecent 2000 (M) = 20 ml /day (P) 100 days (S) If Survival time is decreased by half, the BM must double its production to maintain the man of 2000 ml of RBC 2000 ml(M)= 40 ml/day (P) 50 days(S)
- 6. Tests to Measure Erythropoiesis A) M/E Ratio ( 3:1) or E:G Ratio (1:3) B) Fecal Urobilinogen C) PITR ( Plasma Iron Turnover Rate)
- 7. Two Types of Erythropoiesis A) Effective Erythropoiesis 1) Reticulocyte count 2) Red Cell Utilization of Iron 3) Red Cell Survival Time B) Ineffective Erythropoiesis Two groups demonstrating I.E. 1) Hypoproliferative anemias 2) Anemias secondary to maturation
- 8. Factors Involved in the Release of RBC 1) Hypoxia 2) Presence of Erythropoietin 3) Thyroid Hormone 4) Androgenic Hormone 5) Growth Hormone 6) Prostaglandins
- 9. Normal red cells Normal red cells or erythrocytes show only slight variation in size and shape. The blood film should be examined in the area where the red cells are touching but not often overlapping. In this area many red cells have an area of central pallor which may be up to a third of the diameter of the cell. This is consequent on the shape of a normal red cell, which resembles a disc that is thinner in the centre.
- 10. Variation of RBC ( Anisocytosis) Anisocytosis Anisocytosis refers to increased variation in the size of red cells. This image also shows anisochromasia, i.e. an increased variation in the staining of red cells. Anisochromasia indicates variation in the haemoglobin concentration between different cells.
- 11. Macrocytosis Macrocytosis. Macrocytosis refers to an increase in the average size of red cells. A large red cell is referred to a macrocyte. This blood film is from a patient with macrocytosis caused by liver disease. The MCV was 105 fl (normal range 82-98).
- 12. Macro-ovalocyte An ovalocyte which is appreciably larger than a normal erythrocyte is referred to as a macro- ovalocyte [arrow]. Macro-ovalocytes are a feature of megaloblastic anaemia, congenital dyserythropoietic anaemias and South- East Asian ovalocytosis
- 13. Microcytosis The term microcytosis means that red cells are smaller than normal. Small red cells are referred to as microcytes. This blood film is from a blood sample with a mean cell volume (MCV) of 72 fl (normal range 82-98). There is also hypochromia, i.e. the cells have an increased area of central pallor.
- 14. Microspherocytes Microspherocytes resemble spherocytes in that they lack central pallor but differ in that they are smaller than normal discocytes. They result from red cell fragmentation. This photograph also shows large red cells, which are likely to be young cells, and a nucleated red cell or erythroblast
- 15. Variation of RBC (Poikilocytosis) Poikilocytosis in a baby with hereditary elliptocytosis and transient neonatal poikilocytosis. Poikilocytosis means an increased variability in red cell shape. A poikilocyte is a red cell of abnormal shape. An individual may have a predominance of a particular type of poikilocyte or there may be cells of a variety of shapes.
- 16. Classification of poikilocytes Poikilocytes can be classified as shown.
- 17. Acanthocyte An acanthocyte is an erythrocyte that is irregular in shape and is covered with a small number of spicules (2-20) which vary in length and thickness. The spicules are irregularly distributed over the surface of the red cell. The presence of acanthocytes is referred to as acanthocytosis.
- 18. Severe Liver Disease (Acanthocytosis – Spur Cell Anemia) Acanthocyte are Scanning electron irregularly shape and micrograph of is covered with a acanthocyte small spicules (2 to 20)
- 19. Echinocyte An echinocyte is an erythrocyte with a large number of short blunt spicules (10-30), regularly distributed over the surface of the cell. The presence of echinocytes is referred to as echinocytosis. In this case the abnormality was caused by chronic renal failure but much more often echinocytes represent a storage artefact indicating that EDTA- anticoagulated blood has been stored for too long before the blood film was made.
- 20. Elliptocytes in iron deficiency Elliptocytes are quite common in iron deficiency. They are usually particularly long and thin and for this reason are sometimes referred to as 'pencil cells'. This film also shows anaemia, mild anisocytosis, hypochromia and microcytosis.
- 21. Spherocyte Spherocytes in hereditary spherocytosis. The spherocytes are the cells that lack central pallor. Cells which have rounded up to become spherocytes have a reduced diameter in comparison with normal discocytes but the cell size is normal.
- 22. Sickle cell and boat-shaped cell Sickle cell and boat-shaped erythrocytes in sickle cell anaemia. Sickle cells [dark red arrow] are sickle- or crescent-shaped red cells with both ends being pointed. Boat-shaped cells [dark blue arrows] are pointed at one or both ends but are not curved. Sickle cells are pathognomonic for sickle cell disease whereas boat- shaped cells are suggestive but not pathognomonic.
- 23. Stomatocytes Stomatocytes are red cells that, on a stained blood film, appear to have a slit-like mouth or stoma. In three dimensions they are cup- shaped. Common causes of stomatocytosis are liver disease and alcohol excess. Less common causes include myelodysplastic syndromes and hydroxyurea therapy. Congenital stomatocytosis is a rare cause of stomatocytosis.
- 24. Target cell Target cells are erythrocytes that, in stained blood films, resemble a target. They have an area of increased staining in the centre of the normal area of central pallor. In three dimensions, target cells are found to be bell-shaped. Target cells are a feature of hyposplenism, obstructive jaundice, liver disease and various haemoglobinopathies.
- 25. Teardrop poikilocyte Teardrop poikilocytes or dacrocytes are pear- shaped or teardrop- shaped red cells. They are a feature of idiopathic myelofibrosis (this case), secondary myelofibrosis, megaloblastic anaemia and congenital or acquired dyserythropoiesis
- 26. Keratocyte Keratocytes or horned cells are erythrocytes with a pair of spicules or 'horns' surrounding a gap in the cell outline. There may be a single pair of spicules [red arrow] or two pairs of spicules [blue arrow]. Keratocytes can result from removal of a Heinz body from a cell (this case) or from red cell fragmentation.
- 27. Elliptocytes in hereditary elliptocytosis Elliptocytes are cells of elliptical shape. This film also shows ovalocytes which have an oval outline and are intermediate in shape between elliptocytes and discocytes.
- 28. RBC INCLUSIONS (alpha Chain precipitates) When synthesis of b globin chain is reduced excess alpha chains may precipitate in erythroblasts or mature erythrocytes. a chain precipitates [blue arrow] have the same staining characteristics as haemoglobin and appear as an irregular mass within a hypochromic red cell. They are seen in patients with b thalassaemia major.
- 29. Basophilic stippling Basophilic stippling [arrows] or punctate basophilia refers to the presence of numerous small basophilic inclusions scattered through red cells. They differ from Pappenheimer bodies in being present in larger numbers within an individual red cell and being scattered through the cytoplasm rather than being peripherally sited
- 30. Haemoglobin C crystal Haemoglobin C is prone to crystallize, forming crystals with straight parallel edges [arrows]. They are usually rhomboidal or hexagonal. Usually all the haemoglobin in the cell crystallizes so that the cell appears otherwise empty of haemoglobin.
- 31. Heinz body Heinz bodies are red cell inclusions that are seen only after a specific vital stain, a Heinz body stain, has been performed. They stain pale pink or purple, are attached to the red cell membrane and sometimes protrude through the membrane. Heinz bodies cannot be seen on a routinely stained blood film. However when they are present the routine blood film usually shows irregularly contracted cells and keratocytes. Sometimes there is a protrusion of the red cell membrane
- 32. Glucose-6-phosphate dehydrogenase (G6PD) deficiency The commonest cause of congenital haemolytic anaemia is glucose-6-phosphate dehydrogenase (G6PD) deficiency which affects millions of people world-wide. Most individuals with G6PD deficiency suffer only intermittent haemolysis. The blood film then shows irregularly contracted cells [deep red arrows] and sometimes hemighosts [deep blue arrow] in which all the haemoglobin appears to have retracted to one side of the erythrocyte.
- 33. Howell-Jolly body Howell-Jolly bodies [arrow] are small nuclear fragments within erythrocytes. Their staining characteristics resemble those of the nucleus of a mature erythrocyte. They are round in shape and are sited closer to the edge of the cell than the centre.
- 34. Irregularly contracted cells Irregularly contracted cells are rounded cells lacking central pallor but with irregular outlines. This image also shows large cells that are likely to be young red cells.
- 35. Acquired haemoglobin H disease Acquired haemoglobin H disease occurs in myelodysplastic syndromes and erythroleukaemia. This patient also has sideroblastic erythropoiesis. The film is dimorphic and shows target cells, other poikilocytes, hypochromia and Pappenheimer bodies.
- 36. Pappenheimer bodies Pappenheimer bodies [arrows] are small basophilic inclusions sited near the periphery of red cells. They are smaller than Howell- Jolly bodies, stain deep blue rather than purple and are more likely to be multiple..
- 37. Siderotic granules (Perls' stain) Siderotic granules [arrow] are cytoplasmic granules composed of haemosiderin. The term 'siderotic granule' is used when an iron stain is employed. The same red cell inclusions on a routinely stained film are referred to as 'Pappenheimer bodies'.
- 38. Variation of RBC (Anisochromasia) Anisochromasia This film from an iron deficient patient shows anisochromasia, i.e. there is increased variation in staining from cell to cell. Some cells are normally haemoglobinized while others show only a thin rim of haemoglobinized cytoplasm.
- 39. Dimorphic blood film The term dimorphic indicates that there are two distinct populations of red cells. Most often the term is used, as in this case, to refer to a mixture of normal cells and hypochromic microcytes. This film is from a heterozygous carrier of sideroblastic anaemia. The photograph also shows three cells of abnormal shape.
- 40. Variation of RBC (Hypochromic) Hypochromia Hypochromia refers to reduced staining of red cells, indicative of a reduced haemoglobin concentration. Cells that are hypochromic are often also microcytic. In this film, from a patient with haemoglobin H disease, the great majority of cells are hypochromic.
- 41. Hyperchromia caused by spherocytosis Hyperchromia. The term hyperchromia can be used to indicate the presence of increased numbers of cells lacking central pallor. However it is more useful to state specifically why cells lack central pallor. This film shows hyperchromia consequent on spherocytosis, i.e. the presence of cells which are more spherical than normal cells. In this case they are consequent on autoimmune haemolytic anaemia.
- 42. Rouleaux and increased background staining Rouleaux and increased background staining often occur together since both are consequent on increased concentration of plasma proteins. Rouleaux are stacks of red cells, arranged like a pile of pennies. Increased background staining means that there is a basophilic background between the red cells.
- 43. Red cell agglutination Red cell agglutination is the clumping of red cells into irregular masses. It is caused by the presence of an antibody, usually a cold antibody, which bridges red cells. Agglutination can be distinguished from rouleaux formation by the irregularity of the clumps of cells, in contrast with the stacks of red cells in rouleaux.
- 44. Red cell rosetting Red cell rosetting is an uncommon phenomenon of uncertain significance in which erythrocytes are rosetted around leucocytes.
