Disorders of pituitary gland (( THE MASTER )) BY M.SASI
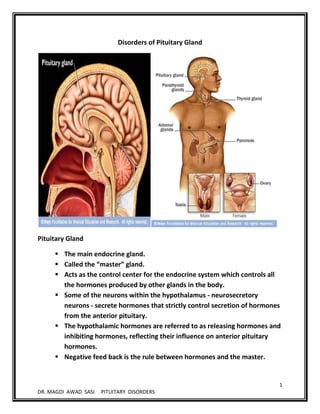
- 1. 1 DR. MAGDI AWAD SASI PITUITARY DISORDERS Disorders of Pituitary Gland Pituitary Gland The main endocrine gland. Called the “master” gland. Acts as the control center for the endocrine system which controls all the hormones produced by other glands in the body. Some of the neurons within the hypothalamus - neurosecretory neurons - secrete hormones that strictly control secretion of hormones from the anterior pituitary. The hypothalamic hormones are referred to as releasing hormones and inhibiting hormones, reflecting their influence on anterior pituitary hormones. Negative feed back is the rule between hormones and the master.
- 2. 2 DR. MAGDI AWAD SASI PITUITARY DISORDERS PITUITARY HYPERFUNCTION (HYPERPITUITARISM) Hyperpituitarism - excessive production of adenohypophyseal hormones . Causes Pituitary adenoma Carcinoma (rare) Hypothalamic disorder-excess stimulation of the pituitary (rare) Order of frequency with which hormone secretion occurs in pituitary tumour is prolactin (relatively common) GH ACTH gonadotrophin TSH PITUITARY HYPERFUNCTION (HYPERPITUITARISM) Prolactin excess Hyperprolactinaemia GH excess Acromegaly/ gigantism ACTH excess Cushing’s disease TSH excess (rare) Secondary hyperthyroidism Gonadotrophin excess menstrual disorders and infertillity
- 3. 3 DR. MAGDI AWAD SASI PITUITARY DISORDERS Hypothalamic releasing and inhibiting hormones are carried directly to the anterior pituitary gland via hypothalamic-hypophyseal portal veins. Specific hypothalamic hormones bind to receptors on specific anterior pituitary cells, modulating the release of the hormones they produce.
- 4. 4 DR. MAGDI AWAD SASI PITUITARY DISORDERS The pituitary gland has two distinct parts, the anterior and the posterior lobes, each of which releases different hormones. Location and size Suspended from hypothalamus by stalk (infundibulum) Housed in sella turcica of sphenoid bone 1.3 cm diameter Contiguous to vascular and neurologic structures 1. Cavernous sinuses 2. Cranial nerves 3. Optic chiasma
- 5. 5 DR. MAGDI AWAD SASI PITUITARY DISORDERS Adenohypophysis(anterior pituitary) Neurohypophysis (posterior pituitary) The portion of the adenohypophysis known as the pars tuberalis contains cords of epithelial cells and is filled with hypophyseal portal vessels. • It reportedly contains gonadotropes and thyrotropes, plus other secretory cells of unknown function. • The pars intermedia is closely associated with pars nervosa and separated from the pars distalis by the hypophyseal cleft. Melanocyte-stimulating hormone is the predominant hormone secreted by the pars intermedia. • Acidophils: contain the polypeptide hormones: 1. Somatotropes which produce growth hormone 2. Lactotropes which produce prolactin • Basophils: contain the glycoprotein hormones: 1. Thyrotropes which produce thyroid stimulating hormone 2. Gonadotropes which produce luteinizing hormone or follicle- stimulating hormone 3. Corticotropes which produce adrenocorticotrophic hormone • Chromophobes These are cells that have minimal or no hormonal content. May be acidophils or basophils that have degranulated and thereby are depleted of hormone May also represents stem cells that have not yet differentiated into hormone-producing cells.
- 6. 6 DR. MAGDI AWAD SASI PITUITARY DISORDERS NOTES: • Although classification of cells as acidophils or basophils is useful in some situations, specific identification of anterior pituitary cells requires immunostaining for the hormone in question. • In addition to differential staining characteristics, the size of secretory granules varies among different types of cells in the anterior pituitary. Somatotropes and lactotropes tend to have the largest size granules. Control of Pituitary: Feedback from Target Organs Negative feedback target organ hormone levels inhibits release of tropic hormones Positive feedback stretching of uterus Oxytocin release, causes more stretching of uterus, until delivery
- 7. 7 DR. MAGDI AWAD SASI PITUITARY DISORDERS Anterior Pituitary “Master gland” Major blood source: hypothalamic-pituitary portal plexus Allows transmission of hypothalamic peptide pulses without significant systemic dilution. Consequently, pituitary cells are exposed to sharp spikes of releasing factors and in turn release their hormones as discrete pulses. Anterior Pituitary “Master gland” Secreted in a pulsatile manner Elicits specific responses in peripheral target tissues Feedback control at the level of the hypothalamus and pituitary to modulate pituitary function exerted by the hormonal products of the peripheral target glands Tumors cause characteristic hormone excess syndromes Hormone deficiency may be inherited or acquired
- 8. 8 DR. MAGDI AWAD SASI PITUITARY DISORDERS Pituitary Tumors 1. Is the tumor causing local mass effect? 2. Is hypopituitarism present? 3. Is there evidence of hormone excess? • Clinical presentation: Mass effect A.Superior extension May compromise optic pathways – leading to impaired visual acuity and visual field defects May produce hypothalamic syndrome – disturbed thirst, satiety, sleep, and temperature regulation B.Lateral extension May compress cranial nerves III, IV, V, and VI – diplopia C. Inferior extension May lead to cerebrospinal fluid rhinorrhea Diagnosis Check levels of all hormones produced Check levels of target organ products Treatment Surgical excision, radiation, or medical therapy Generally, first-line treatment surgical excision Drug therapy available for some functional tumors Simple observation Option if the tumor is small, does not have local mass effect, and is nonfunctional Not associated with clinical features that affect quality of life
- 9. 9 DR. MAGDI AWAD SASI PITUITARY DISORDERS Hyperpituitarism and Pituitary Adenomas Pituitary tumor causes symptoms by any of three mechanisms: 1. By producing too much of one or more hormones. 2. By compressing the pituitary gland, and thus making it produce too little of one or more hormones. 3. By compressing the optic nerves or (less commonly) the nerves controlling eye movements, and thus causing either loss of part or all of the visual field, or diplopia as may extend to cavernous sinus.
- 10. 10 DR. MAGDI AWAD SASI PITUITARY DISORDERS Epidemiology Etiology is unknown Not associated with environmental factors 10-15% of all primary brain tumors 20-25% of pituitary glands at autopsy found to have adenomas 70% of adenomas are endocrinogically secreting 25% of those with MEN-I develop pituitary adenomas Natural History Pituitary adenomas have long natural history Vary in size and direction of spread Microadenomas < 10 mm – may cause focal bulging Macroadenomas > 10 mm – cause problems due to mass effect
- 11. 11 DR. MAGDI AWAD SASI PITUITARY DISORDERS Endocrine-Active Pituitary Adenomas Prolactin – Amenorrhea, galactorrhea, impotence Growth hormone – Gigantism and acromegaly Corticotropin – Cushing’s disease, Nelson’s syndrome post adrenalectomy TSH - Hyperthyroidism Non-functioning Adenomas 25-30 % of patients do not have classical hypersecretory syndromes May grow to a large size before they are detected Present due to mass effect Visual deficits HA Hormone deficiency Prolactinoma: • Prolactin (PRL) is a polypeptide protein hormone secreted by the lactotroph cells in the anterior pituitary gland . • Suppressed by hypothalamic dopamine to act on Lactotroph D2 receptors . • Prolactin (PRL) is the hormone for stimulation & maintenance of milk production in the breast .
- 12. 12 DR. MAGDI AWAD SASI PITUITARY DISORDERS Epidemiology • Most common functional pituitary adenomas . • Prolactinoma account for 40 % of pituitary tumor . • Ninety percent are intrasellar adenomas that rarely increase in size. • The rest are macroadenomas (10 mm) that usually come to clinical attention because of local mass effects. • Microprolactinomas are more frequent in women . • Macroprolactinomas are more frequent in men . • Gender : female more than male 10 :1 • Age : 20-50 years . • Some growth hormone producing tumors also cosecrete PROLACTIN.
- 13. 13 DR. MAGDI AWAD SASI PITUITARY DISORDERS CLINICAL MAINFESTATION: 1. Affect of increased hormone secretion 2. Mass effect 3. Affect on surrounding hormones A. HORMONAL EFFECT : • GnRH release is decreased in direct response to elevated prolactin, leading to decreased production of LH and FSH Women : • Amenorrhea – this symptom causes women to present earlier. • Infertility • Oligomenorrhea, rarely galactorrhea • Dryness in vagina may also occur and this makes intercourse a painful experience • Loss of libido Although many women with hyperprolactinemia will have galactorrhea and/ or amenorrhea .The absence these the two signs do not excluded the diagnosis
- 14. 14 DR. MAGDI AWAD SASI PITUITARY DISORDERS Men • Men with prolactinomas frequently present with headache, visual loss, or neurological deficit but also have hypogonadism and infertility. • Male patient presents with macroadenoma as an elder patient who gradually becomes impotent may refer this to his age. • This will lead to late presentation which is also applies to post menopause female . • Impotence – often ignored • decreased libido, sexual desire • Infertility • Gynecomastia , hair growth decreased, shaving decreased • Rarely galactorrhea • Larger tumors • Signs of mass effect • Hyperprolactinemia may lead to bone loss in both men and women due to the inhibitory effect of prolactin on sex steroids. B. MASS EFFECT : headache ,CSF rhinorrhea , compression of optic chiasma & cranial nerve.
- 15. 15 DR. MAGDI AWAD SASI PITUITARY DISORDERS DIAGNOSIS: • Clinically : by excluded 2o cause of High prolactin . • HYPOTHYRODISM and PREGNANCY are 1st to be excluded. 1) Physiological ( pregnancy ,stress ,nipple suckle ) 2) Hypothalamic - pituitary disease ( tumor, trauma, infiltrative ) 3) Others : hypothyroidism, chest injury, CRF . 4) Drugs . a) Drugs which decrease dopamine stores i) Phenothiazines ii) Amitriptyline iii) Metoclopramide b) Factors inhibiting dopamine outflow i) Estrogen ii) Pregnancy iii) Exogenous sources 5) Biochemical : by serum PRL concentration * Normal range for serum prolactin is 5 - 20 ng/mL . * Serum prolactin values above 200 ng/mL usually indicate the presence of a lactotroph adenoma Prolactin levels correlate with tumor size in the macroadenomas. Suspect another tumor if prolactin low with a large tumor. • Hook effect : can be observed in macroprolactinomas.
- 16. 16 DR. MAGDI AWAD SASI PITUITARY DISORDERS The extremely high PRL levels cause antibody saturation , the resulting in an artifactually low reported value . This can be eliminated by dilution of serum samples. * Other s: FSH ,LH ,GH ,TSH, FT4 , RFT, LFT (2RY DEFICIENCY). Antihypertensive agents Methyldopa (Aldomet) Reserpine (Hydromox, Serpasil, others) Verapamil (Calan, Isoptin) Opiates Codeine Morphine Antipsychotics agent Phenothiazine drugs Haloperidol (Haldol) Risperidone (Risperdal) Antidepressant agents Clomipramine (Anafranil) Desipramine (Norpramin) Gastrointestinal drugs Cimetidine (Antiacid) Metoclopramide (Antaemetic) Drugs Diagnosis A. Assess hypersecretion • Basal, fasting morning PRL levels (normally <20 ug/L) – Multiple measurements may be necessary • Pulsatile hormone secretion • levels vary widely in some individuals with hyperprolactinemia .
- 17. 17 DR. MAGDI AWAD SASI PITUITARY DISORDERS B.Imaging : MRI Of Head • Is the most sensitive test for detecting and measuring prolactinomas. MRI scans may be repeated periodically to assess tumor progression and the effects of therapy. Computer tomography (CT scan) also provides an image of the pituitary, but it is less sensitive than the MRI for detection of a prolactinoma. • Should be performed in a patient with any degree of hyperprolactinemia to look for a mass lesion in the hypothalamic-pituitary region and look for damage to surrounding tissues. TREATMENT: The goals of therapy are to normalize prolactin, fertility, reduce tumor size, and ameliorate the symptoms of hypogonadism & correct any vision abnormalities.
- 18. 18 DR. MAGDI AWAD SASI PITUITARY DISORDERS The indications for treatment : 1) Neurologic symptoms . 2) Hypogonadism or other symptoms . 1.The corner stone treatment of prolactinomas are medical treatment . DOPAMINE AGONISTS Dopamine agonists decrease prolactin secretion and reduce the size of the lactotroph adenoma in more than 90 % of patients. Decrease symptoms within days . Decrease in serum prolactin within 2-3 weeks . Decrease in size within 6 weeks ... ( 6 month ) .
- 19. 19 DR. MAGDI AWAD SASI PITUITARY DISORDERS 1. Bromocriptine : dopamine agonist, It is given at least twice a day . 1.25 -2.5 mg PO at bedtime or with dinner ( max. 15 mg / d ) – Safe in pregnancy// Will restore menses Bromocriptine normalizes prolactin and decreases tumor size in 80–90% of patients with microadenomas and in 70% with large tumors. 2.Cabergoline : administered once or twice a week . 0.25 mg twice /wk or 0.5 mg once/wk . 2. Cabergoline is more effective and better tolerated than bromocriptine and is also effective in treatment of tumors resistant to other dopamine agonists. Cessation of therapy leads to recurrence of hyperprolactinemia and tumor reexpansion . Adverse effects Common Less common Nausea Postural hypotension Mental fogginess valvular heart disease Nasal stuffiness, Depression, Raynaud phenomenon, Constipation 2.Surgical TRANSSPHENOIDAL SURGERY The indications for surgery : 1) Patients who do not respond to medical treatment or those who show progression after an initial response to medical treatment . 2) Women who have a microadenoma, desire pregnancy, and cannot tolerate medical treatment.
- 20. 20 DR. MAGDI AWAD SASI PITUITARY DISORDERS 3) RADIATION THERAPY The indications for radiation : Radiation is primarily used to prevent regrowth of residual tumor in a patient with a very large macroadenoma after transsphenoidal debulking 4) ORAL CONTRACEPTIVE The indications for Estrogen- progestin : can be considered as therapy in women with symptomatic microprolactinomas IF : women cannot tolerate or Do not respond to dopamine agonists or Do not want to become pregnant. Follow Up After one month of therapy, the patient should be evaluated for side effects and serum prolactin should be measured , So : If the serum PRL is normal and no S/E So (continued). If the serum PRL not decreased to normal but no S/E , the dose should be increased gradually to as much as 1.5 mg of Cabergoline 2 or 3 times / week or 5 mg of Bromocriptine 2 times / day. Whatever dose results in a normal serum prolactin value should be continued . If the prolactin has been normal for two or more years and no adenoma is seen on MRI , discontinuation of the drug is the rule. NOTE: • How frequently to image the pituitary after therapy ? 【measure prolactin yearly and do not repeat an MRI unless there is a marked increase in prolactin (more than 250 μg/liter) or clinical signs of tumor expansion such as headaches or visual loss】. • Because macroadenomas possess a higher growth potential, more frequent radiographic monitoring is necessary. 【 repeat an MRI 2–3 yr after achievement of normal prolactin and reduction in tumor size to confirm tumor suppression and to ensure that prolactin levels are a reliable indicator of tumor size】.
- 21. 21 DR. MAGDI AWAD SASI PITUITARY DISORDERS
- 22. 22 DR. MAGDI AWAD SASI PITUITARY DISORDERS ACROMEGALLY
- 23. 23 DR. MAGDI AWAD SASI PITUITARY DISORDERS ESSENTIALS OF DIAGNOSIS Excessive growth of hands, feet, jaw, and internal organs; or gigantism before closure of epiphyses. Amenorrhea, headaches, visual field loss, weakness. Soft, doughy, sweaty handshake. Elevated IGF-I. Serum GH not suppressed following oral glucose. Acromegally is an anterior pituitary disorder characterized by: • Enlargement, thickening, and broadening of bones • Particularly extremities of the body Epidemiology: Estimated incidence is 3-4 cases/ million /year. No clear relationship exists between incidence and race. Acromegaly occurs with equal frequency in males and females. Median age at diagnosis is 40 years in males and 45 years in females . Problems in childhood or adolescence Gigantism = oversecretion; dwarfism = hyposecretion Sweating is a usual compliant. SYMPTOMS AND SIGNS includes: 1. Excessive growth of soft tissues and bones
- 24. 24 DR. MAGDI AWAD SASI PITUITARY DISORDERS A. Thick, coarse, oily skin; enlarged lips, nose and tongue, Supraorbital ridges, Broadening of nose. B. Thickening wrinkles on forehead (bossing) C. Protrusion of Lower jaw (prognathism) D. Deepening of the voice due to enlarged sinuses and vocal cords; snoring due to upper airway obstruction E. Abnormal growth of the hands-spade like/feet F. Excessive sweating and skin odor; fatigue and weakness; headaches; impaired vision; G. Enlargement of body organs, including the liver, spleen, kidneys and heart. H. Face with these features called as acromegalic or guerilla face I. Multiple skin tags J. Colon polyps----3-6 more likely than general population K. Increased skin and GIT tumors. L. Bone changes alter facial features including the spacing of teeth M.arthritis Thyroid , parathyroid and adrenal glands shows hyperactivity
- 25. 25 DR. MAGDI AWAD SASI PITUITARY DISORDERS 2.Metabolic disturbance High blood pressure//high blood sugar Heart disease Sleep apnea Carpal tunnel syndrome Pain symptoms (including headache). Kyphosis ,arthritis Visual disturbance – Bitemporal hemianopia
- 26. 26 DR. MAGDI AWAD SASI PITUITARY DISORDERS 3. Pressure symptoms: Decreased visual field and a acuity May involve the cavernous sinus with ophthamoplegia May extend to the hypothalamus with disturbance of temperature blood pressure Control, appetite disturbance ,sleep and behavioral changes. 4. 2ry hormonal deficiency ((hypopituitrism)): As the adenoma is increasing in size, it will compress over the hypothalamic pituitary stalk leading to decreased supply of the secretor hormones with reduction of sex hormones , thyroid hormones and cortisol. TSH: causes fatigue, low energy, and weight gain. Prolactin: causes inability to breastfeed after delivery. ACTH: fatigue , low blood pressure, low sugar, and upset stomach. Gonadotropins (FSH and LH): cause infertility, decrease in sex drive, impotence, and irregular menstrual cycles. Acromegaly Co-morbidities Hypertension and heart disease Cerebrovascular events and headache Sleep apnea 50% Arthritis irreversible Insulin-resistant diabetes 40% DM or Glucose in tolerance
- 27. 27 DR. MAGDI AWAD SASI PITUITARY DISORDERS Causes of Acromegaly • Hypersecretion of GH after fusion of epiphysis with shaft of bone • Adenomatous tumor- Slow growing pituitary tumour (99%) Diagnosis: • The diagnosis of acromegaly is optimally based on both clinical and biochemical evidence . Lab Studies include: 1. glucose non suppressibility test. Two baseline GH levels are obtained prior to ingestion of 75 or 100 g of oral glucose, and additional GH measurements are made at 30, 60, 90, and 120 minutes following the oral glucose load. Patients with active acromegaly are unable to suppress GH concentration below 1µg/L (immunradiometric assay) or below2µg/L (older radioimmunoassay) after a 75-g oral glucose load 2. IGF-I measurement: It is useful to gauge integrated GH secretion, to screen for acromegaly , and to monitor the efficacy of therapy. How do you screen for acromegaly? Check for high IGF-I levels (>3 U/ml) 3. Measurement of IGF-binding protein-3 (IGFBP-3): The main binding protein for circulating IGF-1, is increased in acromegaly. It might be useful in the diagnosis of acromegaly and may also be helpful in following the activity of the disease during treatment . • GHRH concentration can be obtained if clinically indicated. • Random GH measurements which are often not diagnostic because of the episodic secretion of GH, its short half-life, and the overlap between GH concentration in acromegalic patients and healthy subject
- 28. 28 DR. MAGDI AWAD SASI PITUITARY DISORDERS Imaging Studies: • Imaging studies are only carried out after a firm biochemical diagnosis of acromegaly. • Imaging of the sella turcica should be performed first. • Skull x-ray may show ballooning of pituitary fossa in cases of pituitary macroadenoma • MRI is more sensitive than CT scan. • MRI shows a pituitary tumor in 90% of acromegalic patients.
- 29. 29 DR. MAGDI AWAD SASI PITUITARY DISORDERS Treatment: Objectives of Treatment for Acromegaly • Control and reverse symptoms and signs • Suppress GH and IGF-1 to control morbidity and mortality • Decrease pituitary tumor size • Control tumor mass effects • Preserve normal pituitary hormone secretion A multimodality approach usually requires surgery as the first treatment line followed by medical therapy for residual disease Radiation treatment is reserved for refractory cases Treatment Surgery Radiotherapy (not widely used) Stereotactic Gamma Knife Dopamine Agonists ( Cabergoline) Somatastatin Analogue (Octreotide LAR, Lanreotide Autogel) GH receptor Antagonist (Pegvisomant)
- 30. 30 DR. MAGDI AWAD SASI PITUITARY DISORDERS Surgical treatment: • Even though surgery ( Transsphenoidal hypophysectomy ) might not cure a significant number of patients , it is employed as the first line therapy. • A remission rate of 80-85% can be expected for microadenomas and 50- 65% for macroadenomas. • Sweating and carpal tunnel syndrome are improved within 24hours.
- 31. 31 DR. MAGDI AWAD SASI PITUITARY DISORDERS CUSHING’S DISEASE Cause • Hypersecretion of glucocorticoids mainly cortisol • Either pituitary origin or adrenal origin OR ectopic ACTH Cushing’s Cushing’s disease syndrome Pituitary origin • Increased secretion of ACTH leads to hyperplasia of adrenal cortex therefore, hypersecretion of glucocorticoids takes place. • ACTH is increased by • Tumor in pituitary cells ( basophilic cells)
- 32. 32 DR. MAGDI AWAD SASI PITUITARY DISORDERS • Malignant tumor of nonendocrine origin like cancer of lungs or abdominal viscera • Hypothalamic disorder causing hypersecretion of corticotropin releasing hormone • Cushings syndrome is a disease due to chronic exposure of tissues to excess (supra-physiological doses) glucocorticoid (GC) hormones from endogenous or exogenous source. Causes / types: • ACTH-dependant • Non-ACTH-depentant • Pseudo-Cushings syndrome Signs and symptoms 1. Disproportionate distribution of body fat results: • Moon face: Fat accumulation and retention of water and salt. • Torso: Fat accumulation in chest and abdomen but slim legs and arms(muscle wasting muscle atrophy and weakness-proximal ). • Buffalo hump: Fat deposit on the back of neck and shoulder. • Pot belly: Fat accumulation in upper abdomen.
- 33. 33 DR. MAGDI AWAD SASI PITUITARY DISORDERS 2. Purple striae : Reddish purple stripes on abdomen due to: Loss of collagen fibers due to protein depletion thin, weakened integumentary tissues purple striae; rupture of small vessels. Stretching of abdominal wall by excess subcutaneous fat Rupture of sub dermal tissues due to stretching. - Skin- thin, atrophic skin , easily damaged, with skin breaks And ulceration 4. Thinning of subcutaneous tissues, bruises, echymoses. 5. Darkening of skin on neck (aconthosis) 6. Pigmentation of skin - due to very high levels of ACTH - manifestation in: mucous membranes, hair, and skin . 7. Facial redness (facial plethora) 8. Weakening of muscle-proximal myopathy. 9. Facial hair growth ( Hirsutism )- acne, oligomenorrhea ,changes of ovulation due to adrenal androgens level in women 10. Bone resorption leads to osteoporosis 11. Hyperglycemia due to gluconeogeneis leads adrenal diabetes and glycosuria
- 34. 34 DR. MAGDI AWAD SASI PITUITARY DISORDERS 12. Hypertension vascular sensitivity to catecholamines. 13 Suppression of the immune system susceptibility to infections 14. Poor healing 15. hyperglycemia, glycosuria, hypokalemia, metabolic alkalosis Epidemiology Majority of cases are Exogenous due to therapeutic use of glucocorticoids / ACTH Endogenous CS : Annual incidence has been estimated to be 13 cases / million (USA) : 70 % Cushing`s disease (CD) 15 % Ectopic ACTH secretion 15 % Primary adrenal tumor Sex : F : M ratio for pituitary or adrenal CS 5 : 1 Ectopic CS : more common in males-lung cancer Age : Peak incidence of pituitary or adrenal CS : 25-40 years Ectopic ACTH CS usually occurs later in life Mortality / Morbidity 1. Primarily related to glucorticoid (GC) excess ie : HTN, DM, perforated viscera , immune suppression, psychiatric problems, … 2. . Pituitary tumors may increase morbidity and mortality 3. . Adrenocortical carcinoma 5-y survival < 30%. 4. . Exogenous GC suppress HPA axis which carries risk of adrenal crisis
- 35. 35 DR. MAGDI AWAD SASI PITUITARY DISORDERS Differential Diagnosis Pseudo-Cushing`s Syndrome . Major depression . Alcoholism Hypercortisolism without Cushing`s syndrome . Obesity . Psychiatric illness / anorexia nervosa . Stress : acute illness, trauma, …etc . States of elevated (cortisol binding globulin) CBG : . Pregnancy . Estrogen therapy . Hyperthyroidism . Familial generalized glucocorticoid resistance Diagnosis of Cushing`s Syndrome Principals 1. Biochemical Confirmation 2. Localization by Imaging Steps of Diagnostic Workup 1. Screening tests 2. Confirmation of diagnosis of CS 3. Knowing the Cause of CS 4. Imaging Steps to do: DEXAMETHAZONE single night dose DEXAMTHEAZONE 2 days Urinary free cortisol
- 36. 36 DR. MAGDI AWAD SASI PITUITARY DISORDERS Screening Tests in the evaluation of Cushing’s syndrome Specificity (%) Sensitivity (%) InterpretationMeasurementsProtocolTest 70 - 8098Normal, < 5 mcg/dl 8 A.M. plasma cortisol. Dex, 1 mg PO at 11 P.M. 1 mg overnight DST 9895-100Values 2 – 3 fold higher than the upper limit of normal suggest Cushing syndrom Cortisol, creatinine.24-hr urine collection 24-hr urine free cortisol ( UFC) 74 - 10056 - 69Urine free cortisol >36 mcg/day or urine 17-OHCS >4 mg/day suggests Cushing syndrom 24-hr urine collection for cortisol, 17-OHCS, creatinine during last 24 hrs of dex administration Dex, 0.5 mg PO q6h 48 hrs (last dose 6 A.M.) 2-day low-dose urine DST (UFC) 10090Normal < 1.4 mcg/dL Plasma cortisol 2 hrs after last dose of dexa Dex, 0.5 mg PO q6h 48 hrs (last dose 6 A.M.) 2-day low-dose serum DST Specifici ty (%) Sensitivit y (%) InterpretationMeasurementsProtocolTest 100100Cortisol > 1.4 mcg/dl suggests Cushing’s Plasma cortisol 15 mins after CRH injection Same as LDDST with first dose dex given at noon and CRH, 1 mcg/kg IV at 8 A.M. after last dose of dex. CRH / dex 10092Value < 1.3 ng/mL exc. Cushing’s Salivary cortisol11 P.M sampleLate-night salivary cortisol 10096Cortisol > 7.5 mcg/dL suggests Cushing’s Midnight plasma cortisol Indwelling catheter. Hospitalization recommended Midnight plasma cortisol Screening tests – cont.
- 37. 37 DR. MAGDI AWAD SASI PITUITARY DISORDERS Specificity (%) Sensitivity (%) InterpretationProtocolTest 10083PituitaryCushing’s will havesuppression ofurine 17-OH by >64% or a >90% reductionin urine free cortisol Collest24-hr urine for 17-OH or urinefree cortisol andcreatinine; give dex, 2 mg POq6h 48 hrs; re- collecturine during last 24 hrs of dexadministration. 2– day HDDST 10092PituitaryCushing’s will havesuppression of cortisolby 50% compared tobaseline. Measureplasma cortisol at 8A.M.; givedex 8 mg PO at11 P.M.; redraw plasma cortisol next morningat 8A.M. 8mg dex 10093Increase ofACTH (mean of +15and +30 mins values) by35% over baseline (meanof -5 and -1 min) suggestspituitary Cushing,s CHR,1 mcg/kg IV bolus at 8 A.M. (giventhroughindwellingcatheter placed2 hrs beforebolus );draw plasmaACTH at -5, -1 min before CRHand +15, +30 mins after CRH CRH 10095- 100PituitaryCushing’s if basalpetrosal : peripheral >2 or post-CRH petrosal: peripheral > 3 Simultaneousbilateral inferior petrosalsampling andperipheral samplingforACTH beforeand afterCRH, 100 mcg IV IPSS Differentiating Cushing`s disease from Ectopic ACTH
- 38. 38 DR. MAGDI AWAD SASI PITUITARY DISORDERS PlasmaACTH 2 ACTH<10pg/mL ACTH-IndependentCauses ACTH10-20pg/mL Indeterminate ACTH>20pg/mL ACTH-DependentCauses BiochemicalTests IPSS withCRH Central: PeripheralACTHGradient < 2 2-3 > 3 CushingsDisease Indeterminate EctopicACTH CRHStimulation Test ACTHResponse > 34% < 34% CushingsDisease Indeterminate DexamethasoneSuppression Test UFCor 17-OHCSResponse Present Absent Cushing’sdisease Indeterminate MetyraponeStimulationTest 17-OHCSor Compound S Response Present Absent Cushing’sdisease Indeterminate Bilaterally Small Glands PPNAD Exogenous steroids Unilateral Mass Contralateral Gland Small Adrenal adenoma Adrenal carcinoma Bilateral Masses Idiopathic massive macronodularadrenal disease Massive macronodularadrenal disease/ abnormal receptors McCune-Albright syndrome Bilateral adenomas (Consideriodocholesterolscan to determine functional state of masses) (ReconsiderACTH-dependentforms) AdrenalCTScan ACTH<20 pg/mL ACTH>20 pg/mL Remeasure ACTH, or measure ACTH after CRH
- 39. 39 DR. MAGDI AWAD SASI PITUITARY DISORDERS Imaging Tests
- 40. 40 DR. MAGDI AWAD SASI PITUITARY DISORDERS Imaging studies for Cushing`s syndrome should be performed after the biochemical evaluation has been done 1. Pituitary: 1.5-T hr MRI with 3mm contiguous slices before and after gadolinum contrast 2. Adrenal: CT/MRI Iodo cholestrol scan 3. Chest , Abdomen, Neck, Pelvis CT / MRI 4. Octeriotide scintigraphy 5. Selective venous sampling of site suspected of ectopic ACTH production 6. PET imaging with isotopes eg CII 5HTP TREATMENT: SURGERY MEDICATION RADIOTHERAPY Treatment of Cushing`s syndrome is directed by the primary cause. In general, therapy should reduce the cortisol secretion to normal. The optimal approach to treatment of CS is resection of abnormal tissue. When surgery cannot be done or is not successful , control of hypercortisolism may be attempted with medication. Pituitary radiation may be useful if surgery fails for Cushing`s disease. The treatment for exogenous CS is gradual reduction of dose or withdrawal of glucocorticoid . The treatment of choice for CD is transsphenoidal surgery by an experienced surgeon.
- 41. 41 DR. MAGDI AWAD SASI PITUITARY DISORDERS The goal of surgery is to remove the adenoma , preserving as much pituitary function as possible. A. MRI-guided pituitary surgery, a new procedure, may be indicated B. With experienced surgeon, initial cure ranges from 66% to 89%, but may be much lower in les experienced hands or after repeat surgery C . The more extensive the mass and the resulting resection, the greater the risk for loss of pituitary function D. Transcranial resection for macroadenoma or tumors invading the cavernous sinus. Success rate : 50 %-70 % E. Permenant post-op complications (5%) : DI, partial / complete hypopituitarism, injury to local tissues F. After surgery most patients who achieve long-term remission are hypocortisolemic and require replacement therapy until the HPA axis is normalized , usually within the first postoperative yr G. The recurrence rate after initial surgery is 10% or less . Pituitary irradiation is used when TS surgery is not successful or not possible , late effects include hypopituitarism . Bilateral adrenalectomy is an option if TS surgery , pituitary irradiation, and medical treatment fail to normalize cortisol . Nelson`s syndrome may develop in some patients treated with bilateral adrenalectomy without pituitary irradiation. Assessing Response to Surgery . Most patients who had surgery develop adrenal insufficiency postoperatively and are typically on high dose of hydrocortisone which should be tapered gradually , over 3-4 days . Morning daily cortisol and UFC are obtained daily for 3 days without HC.
- 42. 42 DR. MAGDI AWAD SASI PITUITARY DISORDERS . Post operative hypercortisolemic ===indicate surgical failure. . Eucortisolemic patients with morning values 6-9 ug/dl are at risk of recurrence compared with hypocortisolemic patients . . There should be return to dexamethasone suppressebility Medical treatment of CS((all forms)) . Compounds that modulate ACTH release from pituitary : . Retanserin . Cyproheptadine . Bromocriptine . Octeriotide . Compounds that inhibit stroidogenesis : . Mitotane, ketoconazol, metyrapone, trilostane,etomidate . Compounds that act on cortisol receptor : . Mifeprestone . Combination therapy may be used
- 43. 43 DR. MAGDI AWAD SASI PITUITARY DISORDERS Hyperthyroidism Synthesis and release of thyroid hormones is influenced by TSH from the pituitary. Two kinds of hormones are produce in the thyroid gland triiodothyronine (T3) and thyroxine (T4). Concern the regulation of the metabolic and oxidation rates in all the tissues of the body except the brain. Hypothalamus - the highest control of thyroid function. Hyperfunction Hyperthyroidism - over-activity of the thyroid gland results in excessive secretion of T3 and T4. Hyperthyroidism is a disorder that occurs when the thyroid gland makes more thyroid hormone than the body needs.
- 44. 44 DR. MAGDI AWAD SASI PITUITARY DISORDERS Thyroid hormones circulate throughout the body in the bloodstream and act on virtually every tissue and cell in the body. Hyperthyroidism causes many of the body’s functions to speed up. Thyrotoxicosis is due to diffused toxic goiter (Grave’s disease) or nodular toxic goiter, with single or multiple nodules (adenomas) of the thyroid responsible for the excessive T3 and T4 secretion. Symptoms The patient will have symptoms of toxic thyroid gland. Hyperthyroidism has many symptoms that can vary from person to person CNS--heat intolerance, nervousness or irritability, heat intolerance, fatigue or muscle weakness bilateral progressive proximal myopathy, sweating, trouble sleeping , hand tremors, mood swings (common in young) CVS-- rapid and irregular heartbeat, palpitation , dyspnea , chest pain.(elder) GIT--weight loss, increased apetite, diarrhea, epigastric pain TSOMA is a rare adenoma . DIAGNOSIS: Many symptoms of hyperthyroidism are the same as those of other diseases, so hyperthyroidism usually cannot be diagnosed based on symptoms alone. With suspected hyperthyroidism, a medical history and physical exam mandatory . 1.TSH test 2.T3 3.T4 Increased levels of TSH in toxic patient gives a clue to the diagnosis.
- 45. 45 DR. MAGDI AWAD SASI PITUITARY DISORDERS PART 2= DEACREASED HORMONE PRODUCTION HYPOPITUITRISM (Anterior Pituitary Insufficiency) Partial/ complete hypopituitrism The pituitary gland is effected by something and may be deficient in one single hormone, several hormones, or have complete pituitary failure(PAN). Hypopituitarism is a rare disorder where there is a loss of function in the pituitary and the failure to secrete hormones that affect many of the body's functions. There are may symptoms which are not specific leading to delay of diagnosis and you should look for patients who at risk of pituitary dysfunction like radiotherapy , trauma ,postdelivery shock due to bleeding -sheehans syndrome , TB etc. Who and when? Can affect both males and females. Can occur at any time in life. Can be congenital . Hypopituitarism can also be acquired (a condition that develops later in life) and may be caused by: Radiation to the head Tumors in the brain Other disorders, such as tuberculosis or sarcoidosis which infiltrate the gland, can result in a reduction in function.
- 46. 46 DR. MAGDI AWAD SASI PITUITARY DISORDERS Causes of hypopituitarism Tumours (tu’) Pituitarytumor Adenoma,craniopharyngioma Cerebraltumor Hypothalamicdisorders Tumor Functionaldisturbance- Eg -Anorexia nervosa IsolatedGH and GnH secretion due to impairedsecretionof hypothalamicreleasing hormones Miscellaneous Sarcoidosis(inflammation of L.N) Histocytosis X(abnormal increasein the numberof immunecells ) Haemochromatosis Vascular ds Necrosis(Sheehan’s synd) Infarction Severehypotension Cranial arteritis Trauma Infection Meningitis esp TB, syphilis Iatrogenic Surgery Irradiation Prolongedrx with glucocorticoidor thyroid hormones-isolatedACTH or TSH suppression 3 most common causes: secretory adenoma of ant pituitary Sheehan’s syndrome (postpartum pituitary necrosis) Empty sella syndrome (pituitary gland become shrinks or becomes flattened)
- 47. 47 DR. MAGDI AWAD SASI PITUITARY DISORDERS GENERAL RULES IN HYPOPITUITIRSM: Partial hypopituitarism is more frequent than PANHYPOPITUITRISM. Symptoms/signs do not manifest until > 75% of ant lobe is destroyed. GH secretion is an early feature of pituitary failure which effects is dramatic in children but less significant in adults. LH/ FSH are affected before ACTH. The hormones which are mandatory for survival are the last to be lost. Hypothyroidism is an uncommon presenting feature of pituitary failure. The presentation differs depending on: -age -sex -severity of the deficiency -number of hormones involved -underlying cause of the hypopituitarism Hormone Features of deficiency GH Children: growth retardation, weakening of bone strength Adults: ↓muscle bulk, feeling unwell Tendency to hypoglycaemia. Prolactin Gonadotrophins Failure of lactation Children: delayed puberty Female: oligomenorrhoea, infertility,atrophy of breast &testis Male: Impotence,azoospermia,testicular atrophy Both sexes: loss of libido, loss of body hair ACTH Weight loss ,Hypotension, fatigue and low energy
- 48. 48 DR. MAGDI AWAD SASI PITUITARY DISORDERS TSH Vasopressin Hypoglycaemia ,Hypotension, decrease skin pigmentation Weight gain, cold intolerence,fatique Thirst, polyuria
- 49. 49 DR. MAGDI AWAD SASI PITUITARY DISORDERS Measurement of anterior pituitary hormones: Measured in serum by immunoassay Pulsatility of secretion of some of these hormones makes inappropriate to rely on single measurements for diagnostic purposes Dynamic tests/ functional tests are important tools in investigating pituitary functions and other endocrine organs. INSULIN INDUCING HYPOGLYCEMIA(ITT) Isolated deficiencies of anterior pituitary hormones due to pathologies other than genetic – do exist! If present – may point to underlying pathology 1. Isolated gonadotrophin deficiency-Haemochromatosis 2. Isolated ACTH deficiency -Lymphocytic hypophysitis Timing of onset of hypopituitarism • Childhood GHD - growth FSH/LH – puberty • Adult Normal height/secondary sex characteristics Investigation for Hypopituitarism: • Gonadotrophin status – FSH,LH,T/E2 – GnRH test x – TSH, FT4
- 50. 50 DR. MAGDI AWAD SASI PITUITARY DISORDERS – TRH test x – Prolactin – INSULIN TOLERANCE TEST GH stimulation tests • ITT/Arginine/Glucagon • Arginine + GHRH • GHRH + GHRP Diabetes Insipidus • 24 hour urine output > 3 litres • 8 hour fluid deprivation test Radiology – MRI Scan Microadenoma vs Macrodenoma o Risk of hypopituitarism Stalk interruption Type and site of lesion Evolution Basic principle of dynamic tests: Hypofunction - stimulation tests Hyperfunction-suppression tests Treatment Hormone replacement therapy, including glucocorticoids, thyroid hormone, sex steroids, growth hormone and vasopressin, is usually free of complications.
- 51. 51 DR. MAGDI AWAD SASI PITUITARY DISORDERS • Hormone replacement therapy – usually free of complications • Treatment regimens that mimic physiologic hormone production – allow for maintenance of satisfactory clinical homeostasis Trophic Hormone Deficit Hormone Replacement ACTH Hydrocortisone (10-20 mg A.M.; 10 mg P.M.) Cortisone acetate (25 mg A.M.; 12.5 mg P.M.) Prednisone (5 mg A.M.; 2.5 mg P.M.) TSH L-Thyroxine (0.075-0.15 mg daily) FSH/LH Males Testosterone enanthate (200 mg IM every 2 wks) Testosterone skin patch (5 mg/d) Females Conjugated estrogen (0.65-1.25 mg qd for 25days) Progesterone (5-10 mg qd) on days 16-25 Estradiol skin patch (0.5 mg, every other day) For fertility: Menopausal gonadotropins, human chorionic gonadotropins GH Adults: Somatotropin (0.3-1.0 mg SC qd) Children: Somatotropin [0.02-0.05 (mg/kg per day)] Vasopressin Intranasal desmopressin (5-20 ug twice daily) Oral 300-600 ug qd
- 52. 52 DR. MAGDI AWAD SASI PITUITARY DISORDERS Prognosis/Prevention • Patients can lead a normal life • Hypopituitarism is permanent so it requires a lifelong treatment • Patients will have to alter their lives depending on the primary cause of the disorder. • There is no known prevention except for the prevention of damage to the pituitary/hypothalamic area from injury. DON’T FORGET: • Remember that the cause may be functional – Treatment should be aimed at the underlying cause • Hypopituitarism may present 1) Acutely with cortisol deficiency 2) After withdrawal of prolonged glucocorticoid therapy that has caused suppression of the HPA axis. 3) Post surgical procedure//Post trauma -Hemorrhage • Exacerbation of cortisol deficiency in a pt w unrecognized ACTH deficiency 1. Medical/surgical illness 2. Thyroid hormone replacement therapy Glucocorticoid replacement require careful dose adjustments during stressful events. Consider cortisol deficiency In a patient who has received a large dose of radiation particularly if 1) sodium 2) TSH deficient 3) symptoms worsen with thyroxine therapy
- 53. 53 DR. MAGDI AWAD SASI PITUITARY DISORDERS 4) SPECIFIC CONDITIONS OF HORMONAL DEFICIENCY: A.Pituitary Apoplexy Hemorrhagic infarction of a pituitary adenoma/tumor. Considered a neurosurgical emergency. Presentation: Variable onset of severe headache Nausea and vomiting Meningismus Vertigo +/ - Visual defects +/ - Altered consciousness Symptoms may occur immediately or may develop over 1-2 days . Risk factors: 1) Diabetes 2) Radiation treatment 3) Warfarin use Usually resolve completely Transient or permanent hypopituitarism is possible • undiagnosed acute adrenal insufficiency Diagnose with CT/MRI Differentiate from leaking aneurysm Treatment: • Surgical - Transsphenoid decompression – Visual defects and altered consciousness
- 54. 54 DR. MAGDI AWAD SASI PITUITARY DISORDERS Medical therapy – if symptoms are mild • Corticosteroids B. Empty Sella Syndrome Often an incidental MRI finding Usually have normal pituitary function • Implying that the surrounding rim of pituitary tissue is fully functional Hypopituitarism may develop insidiously Pituitary masses may undergo clinically silent infarction with development of a partial or totally empty sella by cerebrospinal fluid (CSF) filling the dural herniation. Rarely, functional pituitary adenomas may arise within the rim of pituitary tissue, and these are not always visible on MRI C. Lymphocytic Hypophysitis a. Etiology i. Presumed to be autoimmune b. Clinical Presentation i. Women, during postpartum period ii. Mass effect (sellar mass) iii. Deficiency of one or more anterior pituitary hormones 1. ACTH deficiency is the most common c. Diagnosis i. MRI - may be indistinguishable from pituitary adenoma
- 55. 55 DR. MAGDI AWAD SASI PITUITARY DISORDERS d. Treatment i. Corticosteroids – often not effective ii. Hormone replacement D. Craniopharyngioma Derived from Rathke's pouch. Arise near the pituitary stalk i. extension into the suprasellar cistern common These tumors are often large, cystic, and locally invasive Many are partially calcified ii. characteristic appearance on skull x-ray and CT images Majority of patients present before 20yr Usually with signs of increased intracranial pressure, including headache, vomiting, papilledema, and hydrocephalus Associated symptoms include: – Visual field abnormalities, personality changes and cognitive deterioration, cranial nerve damage, sleep difficulties, and weight gain. • Children – growth failure associated with either hypothyroidism or growth hormone deficiency is the most common presentation • Adults i. sexual dysfunction is the most common problem ii. erectile dysfunction iii. amenorrhea
- 56. 56 DR. MAGDI AWAD SASI PITUITARY DISORDERS • Anterior pituitary dysfunction and diabetes insipidus are common. • Treatment : – Transcranial or transsphenoidal surgical resection followed by postoperative radiation of residual tumor This approach can result in long-term survival and ultimate cure most patients require lifelong pituitary hormone replacement. • If the pituitary stalk is uninvolved and preserved at the time of surgery – Incidence of subsequent anterior pituitary dysfunction is significantly diminished.
- 57. 57 DR. MAGDI AWAD SASI PITUITARY DISORDERS RARE DISEASES(POSTGRADUATE) 1.Dwarfism • Pituitary disorder in children characterized by stunted growth Cause of Dwarfism • Reduction in the GH in infancy or early childhood • Occurs because of following reasons: Deficiency of GH releasing hormone from hypothalamus Deficiency of Somatomedin – C Atrophy of acidophilic cells in the adenohypophysis Tumor of chromophobes : nonfunctioning tumor , compresses and destroys the normal cells Panhypopituitarism
- 58. 58 DR. MAGDI AWAD SASI PITUITARY DISORDERS Signs and Symptoms Stunted skeletal growth Maximum height approximately 3 feet Head becomes slightly larger in relation of body Mental activity is normal without any deformity Reproductive system is not affected due to lack of GH but in Panhypopituitarism puberty is not obtained due to lack of gonadotropic hormone Laron Dwarfism Genetical disorder Called as GH insensitivity Occurs due to presence of abnormal GH secretagogue receptors in liver GHS becomes abnormal due to mutation in genes responsible for receptor Doesn’t depend on amount of GH secretion , hormone can’t stimulate the growth due to abnormal GHS Psychogenic Dwarfism((psychosocial dwarfism or Stress dwarfism)): Due to extreme emotional deprivation or stress Deficiency of GH Dwarfism in Dystrophia adiposogenitalis((Frohlich syndrome)) • Rare childhood disorder • Characterized by : • Obesity • Growth retardation • Retarded development of genital organs • Associated with tumors of hypothalamus – increased appetite and decrease in gonadotropin hormone
- 59. 59 DR. MAGDI AWAD SASI PITUITARY DISORDERS 2.Acromicria • Rare disease in adults characterized by the atrophy of the extremities of the body Causes of Acromicria • Deficiency of GH in adults • Secretion of GH decreases in the following conditions: Deficiency of GH releasing hormone Atrophy of acidophilic cells in the anterior pituitary Tumor of chromophobes Panhypopituitarism Signs and Symptoms • Atrophy and thinning of extremities ( major symptoms ) • Associated with hypothyroidism • Hyposecretion of adrenocortical hormone • Person becomes lethargic and obese • Loss of sexual function
- 60. 60 DR. MAGDI AWAD SASI PITUITARY DISORDERS 3.Simmond’s Disease((cachexia)) Rare pituitary disease Occurs mostly in panhypopituitarism Signs and Symptoms Developing senile decay Senile decay is due to deficiency of hormone from target glands of anterior pituitary e.g. thyroid gland, adrenal cortex and the gonads Loss of hair and loss of teeth The skin on face becomes dry and wrinkled. ( most common ) 4.Dystrophia Adiposogenitalis Obesity and hypogonadism affecting mainly adolescent boys Also known as Frohlich syndrome or hypothalamic eunuchism Causes Hypoactivity of both anterior and posterior pituitary Tumor in pituitary gland and hypothalamic regions concerned with food intake and gonadal development Injury or atrophy of pituitary gland Genetic inablility of hypothalamus to secrete luteinizing hormone Symptoms Obesity (common feature) Sexual infantilism (failure to develop secondary sexual characters) Dwarfism occurs if disease starts in growing age Called as infantile or prepubertal type of Frohlich syndrome (in children) and adult type of Frohlich’s syndrome (in adults) Other features are loss of vision and diabetes.
- 61. 61 DR. MAGDI AWAD SASI PITUITARY DISORDERS 5. Hypothalamic Dysfunction Craniopharyngioma: most frequent cause in children and young adults. Primary central nervous system tumors, pinealomas, dermoid and epidermoid tumors seen in adulthood. Posterior Pituitary hypofunction Vasopressin Main actions: 1.Promote tubular reabsorption of water. 2.Stimulate smooth muscle contraction. By giving vasopressin in pharmacological dose i. Coronary vasoconstriction. ii. Contraction of smooth muscles in the gut. iii. Pallor. Mechanism of action: The disulphide linkage of the peptide may be the means of the attachement to the target organ. So, blockade-------loss of action of hormone. Each day , 70-50ml/H2O isomotic with plasma are filtered by the glomeruli. 85% of the filtered water is reabsorbed passively by the proximal tubule along with the active reabsorption of solutes (Na&CL) without aid of vasopressin. So , the urine remains remains isosomatic with plasma.
- 62. 62 DR. MAGDI AWAD SASI PITUITARY DISORDERS The long U shaped loop of henle form counter –current concentrating system. The ascending limb –actively transports sodium to the interstitial fluid of the renal medulla , reendering this region hypertonic and the urine reaching the distal tubule hypotonic and large volume. ANTIDIURETICHORMONE production(ADH) cranial diabetes insipidus (DI) Posterior Pituitary disorder characterized by excess loss of water through urine. Implication • Site of lesion is hypothalamic/ high stalk. • occurs with posterior pituitary dysfunction. • Pathology of lesion much more likely to be cranopharyngioma vs pituitary adenoma. • Presence of DI provides no information about anterior pituitary function except that ACTH status must be normal for DI to be manifested. • ADH deficiency results in a large volume of urine which is very dilute. Types of DI: Central (neurogenic) origin: failure of posterior pituitary to secrete adequate amounts of ADH. Nephrogenic origin: failure of kidney to respond to circulating ADH Regardless of cause, patients secret Large volumes of dilute urine causing cellular and extra-cellular dehydration resulting in excess thirst(polydypsia and polyuria) DI needs to be differentiated from:
- 63. 63 DR. MAGDI AWAD SASI PITUITARY DISORDERS Primary polydypsia a compulsive psychoneurotic disorder appearing as a thirst disorder. Pt drinks > 5L of water a day Results in decreased ADH secretion and water causes subsequent diuresis plasma and urine are dilute as opposed to DI where urine osmolarity is less than plasma osmolarity due to inappropriate water diuresis Causes of cranial DI INFECTION- Meningitis, Abscess and Encephalitis. ISCHEMIA- Vascular disorders INFLAMMATION- Granulomatous disease Tumors- craniopharyngioma, secondary tumors (metastatic CA), pituitary tumors with suprasellar extension Trauma. Lesion (injury) or degradation of supraoptic and paraventricular nuclei of hypothalamus Lesion in hypothalamo-hypophyseal tract Atrophy of posterior pituitary Surgery. Inability of renal tubules to give response to ADH hormone. Called as Nephrogenic diabetic insipidus IDEOPATHIC. Signs and Symptoms: 1.Polyuria • Excretion of large quantity of dilute urine with increased frequency of voiding is called polyuria. • Daily output is 4 to 12 liters. • Due to absence of ADH ,the epithelial cells of distal convoluted tubule in the nephron and the collecting duct of the kidney becomes impermeable to water.
- 64. 64 DR. MAGDI AWAD SASI PITUITARY DISORDERS 2.Polydipsia • Intake of excess water. • Because of polyuria ,thirst center in hypothalamus results in intake of large quantity of water . 3.Dehydration In some cases ,the thirst center in the hypothalamus is also affected by the lesion. Fatigue , dryness of mouth, dizziness ,palpitation. Therefore water intake decreases in these patients and, the loss of water through urine is not compensated. DIAGNOSIS: Primary test for cause of polyuria - Water deprivation for 12- 18hrs Body weight, BP ,urine volume, urine specific gravity, plasma and osmolarity measured q 2hrs 24-h urine output collection 50 mL/kg per day (>3500 mL in a 70-kg man). Normal response is decreased urine output, increased urine concentration greater than plasma Patient with DI maintain high dilute urine output. pts with primary polydypsia have urine omsolarity greater than plasma . water deprivation continue until plasma lvl plateaus, then AVP is given and urine osmolarity is checked in 1hr Check osmolarity >300 mosmol/L
- 65. 65 DR. MAGDI AWAD SASI PITUITARY DISORDERS Due to a solute diuresis and the patient should be evaluated for uncontrolled diabetes mellitus or other less common causes of excessive solute excretion <300 mosmol/L Due to water diuresis and should be evaluated further to determine which type of DI is present . If does not result in urine concentration before body weight decreases by 5% or plasma osmolarity/sodium exceed the upper limit of normal (osmolarity >300 mosmol/L, specific gravity >1.010) Primary polydipsia or a partial defect in AVP secretion or action are largely excluded Severe pituitary or nephrogenic DI are the only remaining possibilities o pts w/ complete central DI; urine osmolarity increases to about plasma osmolarity . o pts w/ nephrogenic DI; osmolarity of urine increases less than 50%. o pts w/primary poldypsia; osmolarity increases <10%. Diagnosis: Neurogenic vs Nephrogenic • Administer Desmopressin (DDAVP) • 1 g ,0.03 ug/kg ,subcutaneously or intravenously • Measure urine osmolality – (30,60,120 min) ,1 to 2 h later • An increase of >50% indicates severe pituitary DI • Smaller or absent response is strongly suggestive of nephrogenic DI TREATMENT: Central DI Desmopressin acetate (DDAVP) intranasal or orally
- 66. 66 DR. MAGDI AWAD SASI PITUITARY DISORDERS serum osmolarity and sodium is monitored Chlorpropamide (Diabinese) Antidiuretic effect can be enhanced by cotreatment with a thiazide diuretic SE: hypoglycemia, disulfiram like reaction to ethanol Contraindicated in Gestional DI Nephrogenic DI tx seek underlying cause Not affected by treatment with DDAVP or chlorpropamide May be reduced by treatment with a thiazide diuretic and/or amiloride in conjunction with a low-sodium diet Inhibitors of prostaglandin synthesis (e.g., indomethacin) are also effective in some patients maintain a state of mild sodium depletion w/reduction in solute load on kidney by giving diuretics and salt restriction Psychogenic or dipsogenic DI There is no effective treatment Syndrome of Inappropriate secretion of Antidiuretic Hormone (SIADH) • Disease characterized by loss of sodium through urine due to hypersecretion of ADH
- 67. 67 DR. MAGDI AWAD SASI PITUITARY DISORDERS plasma ADH concentrations inappropriately high for plasma osmolarity leads to water retention and hyponatremia w/ decrease plasma osmolarity DX can only be made in absence of hyper-volumemia (nephrotic syndrome, cardiac failure, cirrhosis) and w/ normal thyroid, adrenal and renal function Signs and Symptoms Depends on degree of hyponatremia and rate of fall of plasma osmolarity i. Loss of appetite ii. Weight loss iii. Nausea and vomiting iv. Headache v. Muscle weakness , spasm and cramps vi. Fatigue vii. Restlessness and irritability • Anorexia, vomiting and confusion w/ sodium between 115 and 120mEq/l • Na level <110mEq/l; disorientation, stupor, coma, seizures, paralysis, and focal neurologic findings several malignant and benign conditions are associated w/SIADH
- 68. 68 DR. MAGDI AWAD SASI PITUITARY DISORDERS Disorders associated w/SIADH Pulmonary: malignant- Oat cell carcinoma benign- TB, pneumonia, abscess CNS: meningitis, brain abscess, hd trauma Adverse drug effects: Clofibrate, Chlorpropamide, Cyclophosmamide, Phenothiazine, Carbamazapine Tumors (ectopic production of ADH): lymphoma, Sarcoma, Carcinoma of pancreas or duodenum 31 Syndrome of Inappropriate ADH secretion • Treatment – Acute • Fluid restriction • Hypertonic saline – Central myelinolysis – Chronic • Demeclocyline 150-300mg PO TID- QID –Reversible Nephrogenic DI
