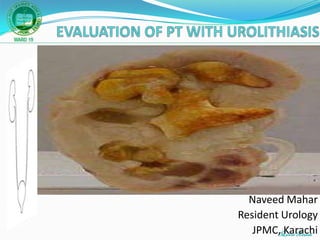
Evaluation of pt with urolithiasis
- 1. Naveed Mahar Resident Urology JPMC, Karachi
- 2. Detailed history Examination Metabolic evaluation Radiological investigations
- 3. HISTORY Demographic biodata Life style Occupation Diet/fluid intake Drug history Systemic disease Family history History of bowel surgery
- 5. OCCUPATION Sedentary occupations predispose to stones more than manual work Low activity levels predispose to bone demineralization and hypercalciuria. Physical activity agitate urine and dislodge crystal aggregates
- 6. DIET Water intake Low fluid intake (<1200 ml/day) predisposes to stone formation A less energy-dense diet may decrease the incidence of stones. Vegetarians have decreased incidence of urinary stones High sodium intake is associated with increased urinary Sodium Calcium PH Decreased urinary citrate
- 7. CLIMATE Summer is the season of urinary stones and dehydration is the key factor Concentrated urine has a lower ph, encouraging cystine and uric acid stone formation Exposure to sunlight may also increase endogenous vitamin D production, leading to hypercalciuria.
- 8. FAMILY HISTORY Incidence increases with positive family history Familial diseases like Cystinuria An auto-somal recessive disorder of transmembrane cystine absorption RTA Type 1 or distal RTA: the distal tubule is unable to secret H+ Urinary ph(>5.5) Low urinary citrate Hypercalciuria Type 2 or proximal RTA: failure of bicarbonate resorption in the proximal tubule. Type 3: a variant of type 1 RTA Type 4 : is seen in diabetic nephropathy and interstitial renal disease.
- 9. PAST HISTORY Bowel resection Inflammatory bowel disease Systemic diseases i-e - Gout - Hyperparathyroidism - Sarcoidosis
- 10. DRUG HISTORY The antihypertensive(triamterene) is associated with urinary calculi Long-term use of antacids containing silica leads to silicate stones. Protease inhibitors in immunocompromised patients are associated with radiolucent calculi. Corticosteroids (increase enteric absorption of calcium, leading to hypercalciuria) Chemotherapeutic agents (breakdown products of malignant cells leads to hyperuricemia)
- 11. PHYSICAL EXAMINATION Pt frequently changes posture to find pain relief Renal colic is associted with tachycardia, sweating,and nausea Costovertebral angle tenderness may be apparent. An abdominal mass may be palpable in patients with hydronephrosis A thorough abdominal examination to exclude other causes of abdominal pain. Abdominal tumors, Abdominal aortic aneurysms Herniated lumbar disks Pregnancy Bladder palpation as urinary retention may present with pain similar to renal colic. Incarcerated inguinal hernias Epididymorchitis A rectal examination helps exclude other pathologic conditions.
- 12. METABOLIC EVALUATION Depends on the stone type(composition) Stone type is analyzed by Polarizing microscopy X-ray diffraction Infrared spectroscopy If stone is not retrieved Radiological appearance radiolucecy/opacity Metabolic evaluation
- 13. METABOLIC EVALUATION… Urine pH pH <6 in a patient with radiolucent stones suggests the presence of uric acid stones. pH consistently >5.5 suggests distal RTA (~70% calcium phosphate stones) Evaluation for cystinuria Cyanide-nitroprusside colorimetric test (cystine spot test) Measurement of 24-hour urinary cystine (>250 mg is diagnostic) Evaluation for RTA If fasting morning urine ph >5.5, the patient is labeled to have distal RTA.
- 14. COMPOSITION & PREVELENCE OF RENAL STONES
- 15. PH VALUES AND PREDISPOSITION TO STONE TYPE
- 16. RADIOLOGIC INVESTIGATIONS 1. X-ray KUB 2. Ultrasonography 3. Intravenous pyelography 4. Computed tomography 5. Magnetic resonance imaging
- 17. PLAIN X-RAY KUB Not useful if stones are Radiolucent Smaller than 4mm Lies over the sacrum or other bony structure. Bowel gases can obscure its efficacy. Can not differentiate between Stones Calcified lymph nodes Phleboliths Sensitivity for diagnosis of stones is 50–70%
- 18. X-RAY KUB
- 19. US KUB Usually done to compliment x-ray KUB Its sensitivity for detecting renal calculi is ~95% Very sensitive for the diagnosis of obstruction and can detect radiolucent stones missed on KUB Its non invasive May miss small stones and ureteral stones Particularly important in pregnant pt
- 20. U/S KUB
- 21. INTRAVENOUS PYELOGRAPHY Useful for patients with suspected indinavir stones Requires trained technician Its an invasive procedure predisposing pts to highly allergic IV contrasts Its very prolonged procedure takes hours Require proper pt preparation Not good investigative modality in acute renal colic
- 22. IVP Films and “phases” of IVP Plain film: This is used to look for calcification overlying the region of the kidneys, ureters, and bladder. Nephrogram phase: Film taken immediately following iv contrast The nephrogram is produced by filtered contrast within the lumen of the proximal convoluted tubule Pyelogram phase: Much denser than the nephrogram phase. As concentrated contrast accumulates in plvicalycel system
- 23. IVP
- 24. X-RAY IVP 3D
- 25. COMPUTED TOMOGRAPHY Has greater specificity (95%) and sensitivity (97%) for diagnosing ureteric - stones Noncontrast spiral CT scans are now the imaging modality of choice Advantages: It is rapid No need for experienced radiologic technician No need for intravenous contrast. Uric acid stones are also visualized Disadvantage: Distal ureteral calculi can be confused with phleboliths. These images do not give anatomic details as seen on an IVP (for example, a bifid collecting system)
- 26. MAGNETIC RESONANCE IMAGING MRI is a poor study to document urinary stone disease. Clue towards obstruction by diagnosing hydronephrosis
