Sacramento Heart Center | B Pro APulse CASP
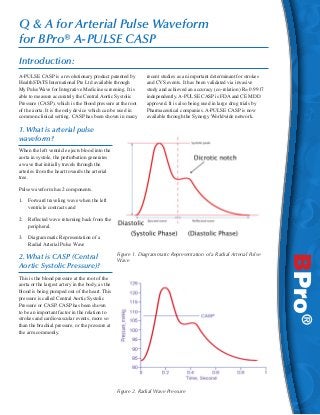
- 1. Q & A for Arterial Pulse Waveform for BPro® A-PULSE CASP Introduction: A-PULSE CASP is a revolutionary product patented by HealthSTATS International Pte Ltd available through My PulseWave for Integrative Medicine screening. It is able to measure accurately the Central Aortic Systolic Pressure (CASP), which is the blood pressure at the root of the aorta. It is the only device which can be used in common clinical setting. CASP has been shown in many recent studies as an important determinant for strokes and CVS events. It has been validated via invasive study and achieved an accuracy (co-relation) R= 0.9917 independently. A-PULSE CASP is FDA and CE MDD approved. It is also being used in large drug trials by Pharmaceutical companies. A-PULSE CASP is now available through the Synergy Worldwide network. 1. What is arterial pulse waveform? When the left ventricle ejects blood into the aorta in systole, the perturbation generates a wave that initially travels through the arteries from the heart towards the arterial tree. Pulse waveform has 2 components. 1. Forward traveling wave when the left ventricle contracts and 2. Reflected wave returning back from the peripheral. 3. Diagrammatic Representation of a Radial Arterial Pulse Wave Figure 1. Diagrammatic Representation of a Radial Arterial Pulse Wave This is the blood pressure at the root of the aorta or the largest artery in the body, as the blood is being pumped out of the heart. This pressure is called Central Aortic Systolic Pressure or CASP. CASP has been shown to be an important factor in the relation to strokes and cardiovascular events, more so than the brachial pressure, or the pressure at the arm commonly. Figure 2. Radial Wave Pressure BPro® 2. What is CASP (Central Aortic Systolic Pressure)?
- 2. Q & A For Arterial Pulse Waveform 3. How to measure CASP? 3.1 Invasive method This is direct measurement and has been considered as the most accurate method. To perform the measurement, a catheter must be inserted into the aortic root from brachial or femoral artery, which is obviously an invasive method and could result in complications (Fig. 3). This invasive method of measuring CASP is not available in clinical setting. However, A-PULSE CASP can be used in clinic and the accuracy has been validated against this invasive method, the result is R= 0.9917 (co-relation). 3.2 Non-invasive method HealthSTATS (HS) invented a device named BPro® which is able to capture radial pressure waveforms. Furthermore, HS developed a proprietary formula to derive central aortic systolic pressure (CASP) from the calibrated radial Figure 3. Direct measurepressure waveform (Fig. 4). ment of CAP using catheter 4. What is augmentation index? Figure 4. Non-invasive measurement of CASP using HealthSTATS BPro® device and APULSE software. The difference between the second and first systolic peaks expressed as a percentage of the pulse pressure. 5. What is the arterial compliance? The ability of an artery to increase the volume in response to a given increase in blood pressure is called compliance. 6. What is pulse wave velocity? PWV is the speed at which the pressure waveform travels (wave propagation) along the aorta and large arteries, during each cardiac cycle. 7. What is applanation tonometry? The principle of applanation tonometry is that the force acting on the plunger is proportional to the pressure in the artery when where the artery surface is flattened. 8. How does CASP help hypertension diagnosis and treatment in primary care? PAGE 2 To evaluate CASP in primary care, we must establish the normal range of CASP. Besides, guidelines of hypertension management should be redesigned based on the stratification of CASP. More and more epidemic clinical studies need to be done to consolidate the normal range of CASP for different races. BPro® and A-PULSE CASP can be used to fulfill this task.
- 3. Sample Waveform of different age groups 19 years old For a normal young person, where the arteries are generally compliant, the slow traveling reflected wave from the peripheral occurs during diastole, thus enhancing perfusion of the coronary arteries. Figure 5. Sample waveform of a 19 year old 47 years old With age, the arteries stiffen. Pulse wave velocity increases and the reflected wave now travels faster and at a higher amplitude, and occurs during systole. This has the effect of prolonging the systolic phase (increasing left ventricular workload and oxygen requirements) but a compromise in coronary artery perfusion Figure 6. Sample waveform of a 47 year old. 82 years old In the elderly, further arterial stiffening causes the reflected wave to return much faster and at much higher amplitude; and coincide very close to the systolic peak, resulting in an augmented wave. The heart now needs to contract even harder (to overcome the oncoming reflected wave) and for a longer period. At the same time, coronary artery perfusion is further compromised. Figure 7. Sample waveform of an 82 year old.
- 4. Q & A For Arterial Pulse Waveform Various indices captured by A-PULSE CASP Systolic & Diastolic Pressure The systolic pressure (SBP) is the peak pressure in the arteries when the heart contracts while the diastolic pressure (DBP) is the lowest pressure when the heart relaxes. Pulse Pressure (PP) PP is the difference between the systolic and diastolic pressure. Normal PP in the brachial artery is approximately 40mmHg. Increase PP may be due to several reasons, e.g. exercise (temporary increase), anemia, Hyperthyroidism, arterial stiffening (usually about 50-60 years)6. Figure 8. SBP is the peak pressure while DBP is the lowest pressure. Central Aortic Systolic Pressure (CASP) Studies have shown that central pressure better represents the load imposed on the coronary and cerebral arteries and hence is more strongly related to vascular hypertrophy, extent of atherosclerosis and cardiovascular events than brachial pressure10-12. Radial Augmentation Pressure (rAP) & Radial Augmentation Index (rAI) Figure 9. PP is the difference between the maximum and minimum pressures. rAI is defined as augmented pressure as a percentage of pulse pressure. It is also influenced by factors such as age and gender. rAP is defined as the difference between 1st [SBP1] and 2nd [SBP2] systolic peaks. Peak Relative Time It is the relative time between the 2 peaks. [T1-T2] In older individuals (> 60), pulse pressure amplification (from central SBP to peripheral SBP) is diminished as a consequence of increased arterial stiffness and the early return of reflected waves in the central arteries. Therefore, the relative timing of the pressure waves merging (forward-backward traveling) may be regarded as the third principal parameter that defines central BP28. A higher peak relative time indicated that the degree of arterial stiffness has increased. Figure 10. CASP derived from proprietary formula in A-Pulse™ CASP Mean Arterial Pressure (MAP) PAGE 4 Mean arterial pressure is the mean perfusion pressure throughout the cardiac cycle. It is also the strongest predictor for stroke and cerebrovascular mortality as it also indicates the perfusion pressure of cerebral circulation16. Normal MAP should be 95±15mmHg. However, it is also dependent on: • Age- older people tends to have higher MAP; • Sex- men have a wider deviation; • Ethnic group- so far, all data are available from the western population. No data is available yet for the Asian population.
- 5. BPro® Arterial Pulse Waveform When the heart contracts a volume of blood is squeezed into the Aorta causing it to stretch to accommodate this new blood volume. Then as the vessel walls return to normal, blood is pushed from the Aorta through the arteries. This process of expansion and returning to normal repeats with each beat of the heart as blood travels through your arteries. If you imagine for a moment that your blood was a strand of pearls being pulled through a much smaller rubber tube, then you will be able to think of circulation not as a series of single beats but as a wave pattern of blood flow. This simplified version of the complex process of circulation does not take into account many aspects of fluid dynamics; however, it does illustrate the two points that I wish to discuss further which are wave patterns and the importance of arterial elasticity. Have you ever stood at the edge of a lake in the morning when the water is calm and then toss a stone into the lake just to watch the waves that are formed? If you have, then you have seen the concentric circles that are formed which travel away from the point where the stone entered the water. If we exclude the effects of fluid dynamics as we did earlier, then these waves would travel unchanged to the other side of the lake. If these waves encountered a rock or log along the way then they would bend around the obstruction, thus altering the wave pattern, but still would continue to the far shore. Now in our arteries these rocks and logs represent build-ups inside the lining of the artery or a stiffening of the artery wall which are precursors to Atherosclerosis and Arteriosclerosis. By analyzing the alterations of a Pulse Wave one can glean a tremendous amount of information about the health and elasticity of an individual’s arterial system. The analysis of the pulse wave consists of measuring the relationship between the forward traveling waves created by the contraction of the heart and reflected waves that travel back towards the heart created by resistance of the arteries. These two wave forms overlap each other to form the pulse wave. As an individual looses elasticity in their arteries the reflected resistance waves increase in intensity, further altering the pulse wave and these changes can be measured. There are primarily two different ways that you can noninvasively measure pulse waves. The first is to measure the movement of the artery walls and the second is to measure the flow of blood through the artery and then from those measurements, estimate the movement of the artery wall. Research facilities and hospitals generally utilize technologies that specifically measure the artery walls because it is through this type of measurement that the greatest level of precision and accuracy is obtained. I have always incorporated the highest level of testing equipment available in our institute, because I closely monitor the arterial elasticity of our patients. I need the assurance that changes in the test results of a patient are due to treatments and not fluctuations in the testing equipment. Other technologies that measure blood flow and then extrapolate arterial wall movement are still valuable tools because they provide information of the health and elasticity of arteries; they are just prone to fluctuations in test results. These fluctuations result from the rapidly changing environment that exists inside our capillaries. The most exciting thing I have seen with these type of devices recently is the advances in the computer industry which have shrunken the size of this technology to that of a wristwatch and inexpensive enough for commercial use. I believe that once more people become aware of the importance of arterial elasticity and have access to testing that only then will we have a chance at impacting the staggering statistics of cardiovascular disease in positive and meaningful way. Daniel Austin, RN High Desert Heart Institute Victorville, CA A Pulse CASP SBP- Systolic Blood Pressure The blood pressure when the heart is contracting. It is specifically the maximum arterial pressure during contraction of the left ventricle of the heart. The time at which ventricular contraction occurs is called systole. In a blood pressure reading, the systolic pressure is typically the first number recorded. For example, with a blood pressure of 120/80 (“120 over 80”), the systolic pressure is 120. By “120” is meant 120 mm Hg (millimeters of mercury).
- 6. Q & A For Arterial Pulse Waveform DBP- Diastolic Blood Pressure The diastolic pressure is specifically the minimum arterial pressure during relaxation and dilatation of the ventricles of the heart when the ventricles fill with blood. In a blood pressure reading, the diastolic pressure is typically the second number recorded. For example, with a blood pressure of 120/80 (“120 over 80”), the diastolic pressure is 80. By “80” is meant 80 mm Hg (millimeters of mercury). PP- Pulse Pressure Blood pressure measurements include both a systolic and a diastolic reading. These two readings are taken at opposite ends of the cardiac cycle and are a person’s highest and lowest blood pressure levels. The difference between these two extremes is called the pulse pressure, and represents the force that your heart generates each time it contracts. a person with a pulse pressure of 40 has normal blood pressure. Consider these examples: Equal Pulse Pressure Doesn’t Mean Equal Risk: Clearly, a blood pressure of 140/100 is much different than 120/80. These examples demonstrate that pulse pressure, by itself, can’t be used to make treatment decisions when other information is unavailable. A person with normal blood pressure (120/80) will have a pulse pressure of 40 (120-80). But that doesn’t mean that • Systolic Pressure = 120; Diastolic Pressure = 80; Pulse Pressure = 120-80 = 40 • Systolic Pressure = 140; Diastolic Pressure = 100; Pulse Pressure = 140-100 = 40 MAP2- Mean Arterial Pressure Based on the time weighted average of blood flow. MAP is considered to be the perfusion pressure seen by organs in the body. It is believed that a MAP that is greater than 60 mmHg is enough to sustain the organs of the average person. If the MAP falls significantly below this number for an appreciable time, the end organ will not get enough blood flow, and will become ischemic. PR- Pulse Rate CASP: Derived Central Aortic Systolic Blood Pressured This value provides a non-invasive assessment of central aortic blood pressure. Higher than normal values of central aortic systolic blood pressure impact the organs of the body and over time can cause organ damage. Normal Ranges are from 106.0 to 119.5 over the age range of Children age 10+ and adults: Well-conditioned athletes: 60–100 40–60 20 years old to 90 years old. See attachment #1 for age range details. PAGE 6 rAI: Radial Augmentation Index This is the index that compares the amplitude of the reflected wave from arteries to the amplitude of the forward traveling wave of blood flow created by the contraction of the heart. This value is a percentage of the reflected wave to the height of the forward wave pattern. Lower numbers here indicate more elastic and pliable arteries. rAP: This is the blood pressure at the height of the reflected wave pattern. Lower values here are better. This is a measure of cardiac after-load and the efficiency of the cardiovascular system. PRT: This is the relative time interval between the Systolic Blood Pressure peak and the reflected augmentation peak. Note: When the reflected wave comes back lower in amplitude and later in time then the arteries have a greater amount of arterial elasticity. Higher reflective waves that rebound in shorter time intervals indicate stiff and less elastic arteries.
