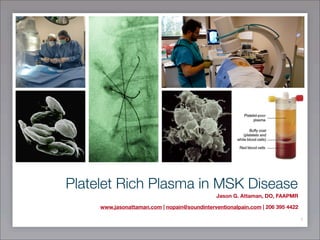
Platelet Rich Plasma in MSK Disease
- 1. Platelet Rich Plasma in MSK Disease Jason G. Attaman, DO, FAAPMR www.jasonattaman.com | nopain@soundinterventionalpain.com | 206 395 4422 1
- 2. Overview About me Basic Science Applications Image Guided PRP Case Presentations 2
- 3. Pain Medicine is an official ABMS Subspecialty Residency in PM&R at the University of Michigan Department of Physical Medicine & Rehabilitation Fellowship in Pain Medicine at Wayne State University Department of Anesthesiology 3
- 5. 5 Patient Injection Psychology Medication RIT (PRP) Surgery Systemic Disease Excercise Sleep Manipulation Alternative Medicine SocialworkPT PRP is but one tool of many! (a cool one!)
- 6. PRP Definition • Platelet-Rich Plasma Therapy (PRP) is defined as a sample of autologous blood with concentrations of platelets in a given volume of plasma that is above the concentration found in whole blood (Arnoczky et al, JAAOS 2010)
- 7. What is PRP therapy useful for? Ligaments Tendons Joints Discs? Nerves? 7
- 8. PRP overview Platelets release various chemical signals when needed These signals cause stem cells to activate, tenocytes to lay down new tendon, chondrocytes to lay down new cartilage, etc PRP therapy accelerates this process by delivering platelets in a concentration 4-10 X normal levels. 8 Works well for tendonopathy, ligament injury, hypermobility, joint degeneration, wound healing, and possibly disc healing Ideally applied in the context of optimizing biomechanics and kinetic chain. Used to “tighten” loose ligaments and tendons
- 9. My experience... 10-20% non responders 25% rapid responders Majority have steady improvement in symptoms over a 6-12 week post-op period followed by a slower improvement phase Tendon architecture improves Overall 80% of those treated with one session have >70% long term pain relief. 9
- 10. History • First introduced in the 1980s for the treatment of cutaneous ulcers (Margolis et al, Diabetes Care 2001) • Use expanded in the 1990s in the maxillofacial and plastic surgery fields (Marx, J Oral Maxillofac Surg 2004)
- 11. History Cont’d • Its use in orthopedic surgery began a decade ago – Initially used with bone grafts to augment spinal fusion and fracture healing – Indications have expanded widely
- 12. Public Awareness • Its appeal has soared ever since Tiger Woods and Cliff Lee swore that PRP cured them • Public awareness was raised after The New York Times detailed the use of PRP to treat the injured Pittsburgh Stealer players Hines Ward and Troy Polamalu before the 2009 Super Bowl – The New York Times, February 17, 2009
- 13. • Blood components: – 93% RBCs – 6% platelets – 1% WBCs – Plasma (liquid component) • PRP: – 94% platelets and plasma – 5% RBCs
- 14. 14 Whole Blood Vs. PRP
- 15. PRP Components • PRP contains not only a high concentration of platelets, but also the full component of clotting factors and secretory proteins
- 16. Platelets • Important in hemostasis / clotting • Platelets are normally activated during the inflammatory phase to begin healing • Role in the normal healing response via the secretion of local growth factors • Growth factors released by platelets recruit reparative cells (stem cells) and augment soft-tissue repair (Eppley et al, Plast Reconstr Surg 2004)
- 17. Creany & Hamilton, Br J Sports Med 2008
- 18. Platelet Activation • Platelets are stimulated to release these growth factors and cytokines by exposure either to collagen or to thrombin and calcium
- 19. PRP Preparation • “Not all PRP preparations are created equal” • PRP can be affected by: – Variations in blood volume taken (5-120 ccs!) – Platelet recovery efficacy – Final volume of plasma in which the platelets are suspended – Presence and/or absence of RBCs and WBCs – The presence of absence of anticoagulant in the sample – The addition or absence of thrombin or calcium chloride – The addition of pH-altering compounds (Arnoczky et al, JAAOS 2010) •
- 20. Lopez-Vidriero et al, Arthroscopy 2010
- 22. Pre Centrifuge
- 23. Post Centrifuge
- 24. Withdraw PRP into procedure procedure syringe
- 25. Technique
- 26. Technique
- 27. Risks and Side Effects Bleeding; <<1% Infection; <<1% No effect; <<1% Worsening pain; <<1% Weakness; <1% Paralysis, death, or stroke; <<<<<<1%. 27 IF image guidance employed for injection!
- 28. Safety • No studies have documented any cases of hyperplasia, carcinogenesis, or tumor growth • Some systems use purified bovine thrombin to activate the platelets, which may produce coagulopathies – Most now have converted to human recombinat thrombin (Mei-Dan et al, Phys Sports Med 2011)
- 29. 99% of MY procedures are done under image guidance to confirm needle location and increase efficacy
- 31. When image guidance is not used
- 32. Needle Tenotomy • Several case series concluding it is effective. • McShane, J Ultra Med, 2006,2008 – ~ 60% effective • Zhu, Adv Ther, 2008 – 54% excellent outcomes • Housner, J Ultra Med, 2009 – Decrease in VAS scores at 4 and 12 weeks • Most physicians peforming PRP do not perform an aggresive tenotomy, which in my opinion limits outcomes. – mild to no pain when local anesthetic administered
- 34. PRP & Doping • In January of 2011, the World Anti-Doping Agency removed intramuscular PRP injections from its prohibitions • There is a “lack of any current evidence concerning the use of these methods for purposes of performance enhancement.” – Irish Medical Times 2011
- 35. Applications • Tendinosis and tendon injuries -- Lateral epicondylitis, Achilles tendinosis • Ligamentous injuries and reconstructive surgery -- ACL • Cartilage injuries • Osteoarthritis • Muscle injuries • Bone augmentation – fusions, nonunions • Wounds – Chronic non-healing • ETC…
- 36. PRP & Tendinopathy What Does The Literature Say???
- 37. Laboratory Evidence: Human Tenocytes • de Mos et al, Am J Sports Med 2008 – In-vitro study of human tenocytes treated with PRP – Results: • PRP stimulates tenocyte proliferation • PRP-treated tenocytes produced increased collagen
- 41. Laboratory Evidence: Achilles Tendon • Virchenko & Aspenberg, Acta Orthop Scand, 2006 – Rat Achilles tendon defect model – Results: • Greater initial regeneration in a rat Achilles tendon defect treated with PRP than without • Greater increases in tendon strength vs. controls at 14 days • Authors concluded: PRP may accelerate the initial inflammatory phase of tendon repair, thus making cells more receptive to earlier mechanical loading
- 42. Laboratory Evidence: Achilles Tendon • Lyras et al, Foot Ankle Int 2009 – Rat Achilles tendon model investigating the effect of PRP injection vs. saline on angiogenesis during tendon healing – Results: • Significant increase in angiogenesis in PRP group at 2 weeks compared to control group • Shorter healing process in the PRP group • Better organization of collagen fibers in the PRP group
- 43. Achilles Tendon Repair • Sanchez et al, Am J Sports Med 2007 – 12 athletes s/p Achilles tendon repair – 6 patients treated with PRP at repair site – Results: PRP group demonstrated: • Earlier functional return of ROM • Earlier return to jogging • Earlier return to training • No wound problems • Less scar tissue based upon Achilles tendon cross- sectional area at 18 months
- 44. Achilles Tendonitis • Gaweda et al, Int J Sports Med 2010 – Prospective study on 14 patients with Achilles tendonitis (15 tendons) treated with PRP – Results: Significant improvement in pain scores and increased tendon vascularization on ultrasound imaging
- 45. Achilles Tendinosis • De Vos et al, Br J Sports Med 2010 – Randomized, double-blind, placebo-controlled trial of 54 patients with Achilles tendinopathy who were treated with PRP vs. control (saline injection), in addition to eccentric exercises – Results: At 6 weeks, there was no significant improvement in tendon structure and no effect on neovascularization in the PRP group, compared to the control group
- 46. Achilles Tendinosis • O’Malley, Presented at: American Orthopaedic Foot & Ankle Society 2010 – Retrospective study of 34 patients with Achilles tendinosis • Symptoms greater than 6 months • Failed conservative treatment – Results: • 19 / 34 had improvement and no longer required treatment • 5 went on to surgery
- 47. Plantar Fasciitis • Barrett & Erredge, Podiatry Today 2004 – Pilot study of 9 patients with plantar fasciitis – Used ultrasound-guided PRP injections – Results: • 6/9 patients had complete symptom resolution after 2 months • 77.9% of patients had complete pain resolution at 1 year
- 50. Lateral / Medial Epicondylitis • Mishra & Pavelko, Am J Sports Med 2006 – Prospective, nonblinded study of 20 patients who failed non-operative treatment for medial or lateral epicondylitis – 15 patients: single PRP injection – 5 patients: single bupivicaine injection – Results in PRP group: • 8 weeks: PRP group statistically significant improvement in VAS and Mayo Elbow Performance scores
- 51. Lateral Epicondylitis • Mishra et al, Clin Sports Med 2009 – Double-blind RCT of PRP vs. cortisone injections of 100 patients – Results: The PRP group demonstrated greater improvement on VAS and DASH scores at a minimum follow-up of 6 months
- 52. Lateral Epicondylitis • Peerbooms et al, AJSM 2010 – Double-blinded randomized control trial of 100 patients treated with either PRP or cortisone injection – Results at 1 year follow-up: • VAS scores – 73% PRP group successful vs. 49% in cortisone group • DASH scores – 73% of PRP group successful vs. 51% in cortisone group • Cortisone group declined with time, while the PRP group progressively improved
- 53. PRP vs Corticosteroid in Lateral Epicondylitis: Netherlands Study. AJSM Feb 2010 l Results: l VAS scores: 49% improved in steroid group l VAS scores: 73% in the PRP group improved l DASH: 51% in steroid group improved l DASH: 73% in the PRP group l PRP group kept getting better over the next year!!! l PRP patients: 64% improvement in pain, 84% disability l Steroid group: 24% improvement in pain, 17% disability
- 55. Evidence: Patellar Tendinopathy • 2 animal studies showed increased strength following PRP • Kon et al. (2009): Prospective pilot study of 20 patients with chronic patellar tendinosis (20+ months) – 70% patients improved • Fiardo et al. (2010): Non-randomized trial, PRP/PT vs PT alone – PRP group did better
- 56. Knee Osteoarthritis • Sanchez et al. (2008) – retrospective cohort design – PRP vs. Hyaluronan – 53% improvement in PRP vs. 10% hyaluronan • Kon et al. (2010) – prospective cohort design – intra-articular PRP injections – significant improvement at 6 months, less at 1 year
- 58. PRP and Muscle
- 59. PRP and Muscle l Sanchez M, et al; “Application of Autologous Growth Factors on Skeletal Muscle Healing”, World Congress on Regenerative Medicine Podium Presentation, May 18, 2005 l Study: 20 patient prospective acute muscle injury pilot study with 6 month follow-up - Ultrasound guided injection of PRP. l Multiple, serial prp injections at one week intervals to defect sites after hematoma evacuation l Ultrasound demonstrated injured muscle healed fully without fibrosis. Functional capacities 50% faster than the control group. l The athletes had full recovery in half the expected times
- 60. PRP and Muscle l Wright-Carpenter et al 2004. IntJ of Sports Med l Pilot study l Professional athletes with muscle strain l Administered autologous conditioned serum l Control group received actovegin/traumeel l Found a reduction in recovery time in return to 100% activity in competitive sports. (16 days vs 22 days in the control group) l MRI recovery time was accelerated as well.
- 61. PRP and Muscle l Hammond et al. Am J Sports Med. 2009 l Tib anterior of rats injected with PRP or PPP for treatment of acute muscle strain (high repetition multiple small strains vs single large strain) l Conclusion: “local delivery of PRP can shorten recovery time after a muscle strain injury in a small animal model.” l Recovery of muscle from a high repetition model has been shown to require myogenesis. This may explain why PRP was more effective in the high-repetition protocol.
- 62. PRP and muscle l Cugat: unpublished case series 2005 International society of arthroscopy l 14 professional athletes l 16 muscular injuries (soccer and basketball) l PRP injected under ultrasound after hematoma aspiration l 50% reduction in time to return to play in less severe injuries. l RTP diminished in each group according to severity
- 69. 69 Pubic Symphisis block for osteitis pubis
- 71. Subtalar Joint
- 72. Ankle Joint
- 74. Patient Selection: who will benefit? Who do you want to “tighten up?” aka your hypermobile patients Any tendonopathy Labral injuries Facet capsule injuries Meniscal injuries 74
- 75. Rehabilitation Protocol Ideal protocol is not yet established 75
- 77. 77 Advanced PRP
- 81. What is the pain generator?
- 86. Treatment
- 89. 89
- 90. 90
- 91. 91
- 92. 92
- 93. 93
- 94. 94
- 95. 95
- 96. 96
- 97. 97
- 98. 98
- 99. 99
- 100. 100
- 101. 101
- 102. 102
- 103. 103
- 104. 104
- 105. 105
- 106. 106
- 107. 107
- 108. 108
- 109. 109
- 110. 110
- 111. 111
- 112. 112
- 113. 113
- 114. Jason G. Attaman, DO, FAAPMR 114 www.jasonattaman.com | nopain@soundinterventionalpain.com | 206 395 4422 Offices in Seattle, Bellevue and Auburn
- 115. 115 Jason G. Attaman, DO, FAAPMR 801 Pine St, Suite 100, Seattle, WA 1600 116th Ave NE #202, Bellevue, WA 202 N. Division, Auburn, WA 206 395 4422 phone 888 688 4167 fax nopain@soundinterventionalpain.com WWW.JASONATTAMAN.COM
- 116. 116
