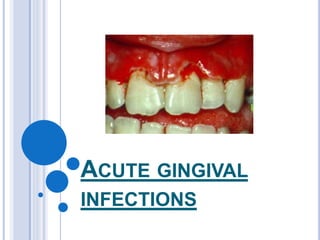
acute gingival infections
- 2. CONTENTS Introduction Primary herpetic gingivostomatitis Necrotizing ulcerative gingivitis (NUG) Pericoronitis Abscesses of periodontium
- 3. INTRODUCTION An acute lesion is of sudden onset and short duration and is painful. They are manifested with severe pain along with systemic manifestations Thus these lesions must be treated at the earliest with a proper treatment protocol.
- 5. HSV- type 1 Infants/ children younger than 6 yrs Males=females Primary infection asymptomatic The virus ascends through the sensory or autonomic nerves and persists in the neuronal ganglia that innervate the site as a latent HSV Sunlight, fever, trauma, stress , after oral surgical procedures
- 6. Secondary manifestations Herpes labialis Herpetic stomatitis Herpes genitalis Ocular herpes Herpetic encephalitis
- 7. Early stage Late stage showing brownish crusted lesions
- 8. CLINICAL FEATURES Intra-oral Diffuse, erythematous, shiny involvement of the gingiva and adjacent oral mucosa Varying degree of edema and gingival bleeding Discrete spherical grey vesicles Primary herpetic gingivostomatitis
- 9. Rupture of vesicles and formation of ulcers after 24 hrs Ulcers– small , painful, red, elevated, halo-like margin with depressed yellowish/greyish white central portion Widely spread/clusters 7-10 days No scarring
- 10. Soreness, difficulty in eating and drinking Ruptured vesicles sensitive to touch, thermal changes, foods such as condiments and fruit juices Infants show irritability and refusal to take food
- 11. Extra-oral Cervical adenitis Fever (101ͦ -105ͦ F) Generalized malaise
- 12. HISTOPATHOLOGY Virus targets epithelial cells Ballooning degeneration (acantholysis, nuclear clearing, nuclear enlargement) Tzanck cells
- 13. Fusing of infected cells Formation of multinucleated cells and intercellular edema Formation of intraepithelial vesicles Rupture Secondary inflammatory response with fibropurulent exudate Ulcers with central portion of acute inflammation and exudation surrounded by zone rich in engorged blood vessels
- 14. DIAGNOSIS Early diagnosis important (reducing symptoms and recurrences) History/clinical findings Virus culture Immunologic tests using monoclonal antibodies or DNA hybridization techniques
- 16. Erythema multiforme: o More extensive vesicles with pseudomembrane formation on rupture o Tongue more involved o Skin lesions present o Prolonged involvement may occur for weeks
- 17. Stevens-Johnson syndrome: rare form of EM characterized by hemorrhagic lesions in the oral cavity, hemorrhagic occular lesions and bullous skin lesions
- 18. Bullous lichen plannus: Rare & painful condition Large blisters on tongue & skin- rupture undergo ulceration Skin lesions + oral involvement Prolonged indefinite course Linear, grey, lacelike lesions of lichen plannus inter-spread among bullous eruptions
- 19. Desquamative gingivitis Chronic condition Diffuse involvement of gingiva Varying degree of peeling of epithelium
- 20. Recurrent aphthous stomatitis Small well defined round shallow ulcers, yellowish grey central areas & red halo H/o previous mucosal ulcers is dignostic, unknown etiology No diffuse erythematous involvement of the gingiva, no acute toxic symptoms
- 21. COMMUNICABILITY Contagious Most adults develop immunity due to infection during childhood – subclinical infection Hence seen in infants & children Recent studies have demonstrated HSV in periodontal pockets (Slots J 2000)
- 22. TREATMENT Consists of early diagnosis & immediate initiation of antiviral therapy. Antivirals : o Acyclovir suspension 15mg/kg is given 5 times daily for 7 days (Amir et al,1997) o It reduces days of fever, pain, lesion and virus shedding
- 23. o Acyclovir does not affect normal cells but inhibits DNA replication in HSV infected cells o Newer antivirals like Valacyclovir and Famicyclovir can also be used o <3 days– antiviral o >3 days- (immunocompetent pt) limited value
- 24. Palliative measures: o Removal of food debris, plaque and supra gingival calculus o NSAID (FEVER AND PAIN) o Extensive periodontal therapy to be postponed o Local /systemic antibiotics to prevent opportunistic infection especially in immuno-compromised patients
- 25. o The patient must be informed that the disease is contagious, thus precautions must be taken (vesicles –highest viral titer) Supportive measures: o Copious fluid intake o Nutritional supplements o Topical anesthetics while eating
- 26. Infection of fingers of health professional treating infected patients may occur and is known as Herpetic Whitlows
- 28. Necrotizing Gingivitis, Necrotizing Periodontitis and Necrotizing Stomatitis are the most severe inflammatory disorders caused by plaque bacteria They are rapidly destructive and debilitating A distinction between these diseases has not always been made in the literature
- 29. Microbial diseases affecting gingiva/ periodontium in the context of an impaired host response Characterized by death and sloughing of tissues
- 30. HISTORY Fourth century BC, Xenophon mentioned that Greek soldiers were affected with “sore mouth” and foul-smelling breath In 1778, John Hunter described the clinical findings and differentiated ANUG from scurvy and chronic destructive periodontal disease ANUG occurred in epidemic form in the French army in the 19th century
- 31. In 1886, Hersch, a German pathologist, discussed some of the features associated with the disease such as enlarged lymph nodes, fever, malaise and increased salivation In 1890s, Plaut and Vincent described the disease and attributed its origin to fusiform bacilli and spirochetes
- 32. NOMENCLATURE Ulceromembranous gingivitis Acute necrotizing ulcerative gingivitis Trench mouth Vincent’s gingivostomatitis Phagedenic gingivitis Fusospirallary periodontitis Plaut-Vincent stomatitis
- 33. CLINICAL FEATURES Classification Acute Subacute (Repeated remissions and exacerbations) Recurrent Single tooth, group of teeth Entire mouth
- 34. NUP (long standing, severe immunosuppression) NUS Noma
- 35. ORAL SIGNS AND SYMPTOMS Punched out, craterlike depressions at the crest of the interdental papilla Can extend into the marginal gingiva, attached gingiva and oral mucosa Grey pseudomembranous slough Linear erythema Removing slough exposes red, hemorrhagic, shiny surface which bleeds easily
- 36. Fetid odor Metallic taste Increased salivation/pasty saliva Can be superimposed on chronic gingivitis/periodontitis Recession rather than pocket formation
- 37. Constant radiating, gnawing pain that is intensified on eating spicy and hot foods and on chewing Lesions extremely sensitive to touch Low socioeconomic groups Seasonal variations (Skach et al, 1970)
- 38. EXTRAORAL AND SYSTEMIC SIGNS AND SYMPTOMS Local lymphadenopathy Fever Increased pulse rate, leukocytosis, loss of apetite and general lassitude additionally seen in severe cases Insomnia, constipation, GI disorders, headache and mental depression in children
- 39. OTHER SEVERE SEQUELAE 1) Fusospirochetal meningitis 2) Peritonitis 3) Pulmonary infection 4) Toxemia 5) Fatal brain abscess 6) Noma
- 40. CLINICAL COURSE ACCORDING TO HORNING AND COHEN: Stage 1 : Necrosis of tip of the interdental papilla (93%). Stage 2 : Necrosis of entire papilla (19%) Stage 3 : Necrosis extending to gingival margin (21%) Stage 4 : Necrosis extending to attached gingiva (1%) Stage 5 : Necrosis extending to buccal / labial mucosa (6%) Stage 6 : Necrosis exposing alveolar bone (1%) Stage 7 : Necrosis perforating skin and check (0%)
- 41. ACCORDING TO PINDBORG: Stage 1: Erosion of only tip of interdental papilla Stage 2: Lesion extending to marginal gingiva and causing potentially a complete loss of papilla Stage 3: Involving attached gingiva Stage 4: Exposure of bone
- 42. HISTOPATHOLOGY Microscopically the lesion is acute necrotizing inflammation of the gingiva, involving both the stratified squamous epithelium and the underlying connective tissue Epithelium destroyed and replaced by meshwork of fibrin, necrotic epithelial cells and PMN’s and various types of microorganisms (surface pseudomembrane) Border: Epithelium edematous and individual cells exhibit varying degree of hydropic degeneration along with infilteration of PMN’s in the intercellular spaces
- 43. Underlying connective tissue: hyperemic with numerous engorged capillaries and dense infiltration by PMN’s (linear erythema) Plasma cells at the periphery(underlying chronic condition) Epithelium and CT alterations decrease with increase in distance from the necrotic area and gradually blends with the uninvolved area
- 44. Listgarten – described four zones that blend with each other ZONE I - BACTERIAL ZONE- The Most superficial zone Consists of varied bacteria, including a few spirochetes of small, medium and large type. ZONE II – NEUTROPHIL RICH ZONE - Contains numerous leukocytes, predominantly neutrophils, with bacteria, including many spirochetes of various types, between the leukocytes
- 45. ZONE III – NECROTIC ZONE- Consists of disintegrated tissue cells, fibrillar material, remnants of collagen fibers and numerous spirochetes of the medium and large types, with few other organisms ZONE IV – SPIROCHETAL INFILTRATION ZONE- Consists of well preserved tissue infiltrated with medium and large spirochetes without other organisms. Spirochetes have been found as deep as 300 microns from the surface
- 46. ETIOLOGY Role of bacteria o Plaut and Vincent in 1894 and 1896, respectively introduced the concept NUG is caused by specific bacteria – namely a fusiform bacillus and a spirochetal organism. o Fusiform bacilli and a spirochetal organism are always found in the disease.
- 47. Rosebury and coworkers described a fusospirochetal complex consisting of T. marcodentium, intermediate spirochetes, vibrios, fusiform bacilli and filamentous organisms in addition to several Borrelia species
- 48. More recently Loesche and colleagues described a constant flora and a variable flora Constant flora :- Fusospirochetal organisms, P. intermedia, A. odontolyticus and various spirilla like Selenomonas species. Variable flora :- Heterogenous array of bacterial types
- 49. Bacteriologic findings have been supported by immunological data presented by Chung et al who reported increased IgG and IgM antibodies to intermediate spirochetes, P. intermedia in NUG patients as compared to those with chronic gingivitis and healthy controls Metronidazole effective
- 50. Role of host response Presence of organisms insufficient to cause disease NUG is not produced experimentally in humans and animals by inoculation of bacterial exudates from the lesion Characteristic lesions occurs in animals when they are under immunosupression Not found in well nourished individuals with fully functional immune system
- 51. Immunosupression essential- NUG patients displayed depression in leukocyte chemotaxis and phagocytosis (Cogen et al, 1983) Nutritional deficiency, fatigue caused by chronic sleep deprivation, alcohol/drug abuse, psychological factors, systemic disease It is hence concluded that - The specific cause of NUG has not been established & it is produced by a complex of bacterial organisms but requires underlying tissue changes to facilitate the pathogenic activity of the bacteria. HIV
- 52. LOCAL PREDISPOSING FACTORS Pre-existing gingivitis Injury to the gingiva (eg: malocclusion) Smoking 98% pts with NUG were smokers & frequency of the disease increases with increasing exposure to tobacco smoke (Pindborg et al, 1951) Preexisting chronic periodontitis, pericoronal flaps (favourable environment for anaerobic fusiform bacilli and spirochetes)
- 53. SYSTEMIC PREDISPOSING FACTORS Nutritional deficiency Produced in animals by giving them nutritionally deficient diet Nutritional deficiencies diminishes immune responses and alteres the periodontal structures, making them more susceptible
- 54. Debilitating disease Chronic diseases( syphilis, cancer) Severe gastrointestinal disorders (ulcerative colitis) Blood dyscrasias( anemia, leukemia) AIDS
- 55. Psychosomatic factors Disease often occurs in association with stressful situations (induction into the armed forces, school examinations) Hypothalamic-pituitary-adrenal axis activation resulting in cortisol secretion and decrease in immune response
- 56. Increase in the levels of cortisol and catecholamines leads to reduced gingival microcirculation and salivary flow which enhances nutrition to P.intermedia Depression in neutrophil and lymphocyte function leads to bacterial invasion and tissue damage. (Johnson and Engel 1986)
- 57. DIAGNOSIS Clinical findings (gingival pain,ulceration and bleeding) Bacterial smear not definitive Microscopic examination of biopsy specimen (TB, neoplastic disease)
- 58. DIAGNOSTIC CRITERIA By Genco, Goldman and Cohen: Interproximal necrosis and ulceration (punched-out papillae) Painful gingiva Bleeding (spontaneous or on slight provocation) Pseudomembrane (fibrin, debris) Fever, malaise, lymphadenopathy “Fetor Oris”
- 59. Herpetic Gingivostomatitis Chronic Periodontitis Desquamative Gingivitis Streptococcal Gingivostomatitis Apthous Stomatitis Diptheric And Syphilitic Lesions Tuberculous Gingival Lesion Candidiasis Agranulocytosis Dermatoses (Pemphigus, Erythema Multiforme ,Lichen Planus)
- 60. Treatment differs Herpes/NUG
- 63. STREPTOCOCCAL GINGIVOSTOMATITIS Characterized by diffuse erythema of the gingiva and other areas of the oral mucosa Necrosis of the gingival margin – not a feature of this disease. No fetid odor Bacterial smears– streptococcal forms Streptococcus viridans , groupA ß-hemolytic streptococcus
- 64. GONOCOCCAL STOMATITIS Caused by Neisseria gonorrhoeae Mucosa is covered with a grayish membrane that sloughs off in areas to expose an underlying raw bleeding surface Most common in new born due to transmission through maternal passages
- 65. AGRANULOCYTOSIS Characterized by marked decrease in number of circulating PMN’s Lesions similar to NUG No marked inflammation due to diminished defense mechanism Blood studies can be used to differentiate between NUG and agranulocytosis
- 66. VINCENT’S ANGINA Fusospirochetal infection of oropharynx and throat, distinguished from NUG, which affects marginal gingiva. May extend to the larynx and the middle ear
- 67. NUG in Leukemia Not produced by leukemia per se , but due to reduced host defense mechanism NUG may superimpose on gingival tissue alteration caused by leukemia
- 68. NUG IN HIV PATIENTS Same clinical features Extremely destructive course leading to NUP Presenting symptom for HIV
- 69. COMMUNICABILITY Not contageous Study by King Kitchen facilities (controlled conditions, anaerobic environment, do not survive on utensils) Occurrence in epidemic like outbreaks– due to common predisposing factors Immunosupression+bacteria
- 70. NUP Extension of NUG or different disease entity No evidence Clinical similarities Until distinction can be proved/disproved, classified together Classification first adopted in world workshop in clinical periodontics in 1989
- 71. Deep interdental osseous craters Recession HIV positive patients Strongly associated Marker of immune supression and diagnosis of AIDS HIV-P Aggressive form of chronic periodontitis
- 72. TREATMENT Alleviation of the acute symptoms by reducing microbial load and removal of necrotic tissue Treatment of chronic disease either underlying the acute involvement or elsewhere in the oral cavity
- 73. Alleviation of the generalized symptoms such as fever and malaise Correction of the systemic conditions that contribute to the initiation or progression of gingival changes.
- 74. SEQUENCE OF TREATMENT FIRST VISIT Complete evaluation Comprehensive medical history with special attention to recent illness, living conditions, dietary backgrounds, type of employment, hours of rest, cigarette smoking, stress levels, HIV Examination should include general appearance, presence of halitosis, skin lesions, vital signs, lymph nodes
- 75. o Characteristic lesions o Oral hygiene (Pericoronal flap Pockets Local irritants) o Only acutely involved areas o Isolated with cotton rolls and dried o Topical anesthetic
- 76. Area swabbed to remove pseudo membrane with moistened cotton pellet after 2-3 min Cleanse area with warm water Superficial calculus removed (ultrasonic scalers) Subgingival scaling and curettage – contraindicated (bacteremia, extend infection to deeper tissues)
- 77. Surgical procedures other than emergencies postponed until pt is symptom free for 4 weeks Antibiotic regimen (amoxicillin 500 mg orally every 6 hrs for 10 days) in moderate to severe cases Metronidazole (500mg BID 7 days) Emergency procedures along with systemic antibiotics
- 78. PATIENT INSTRUCTIONS Patient told to rinse every two hours – glass full of equal mixture of warm water and 3 % Hydrogen peroxide and / or twice daily with 0.12%chlorhexidine Adequate rest Confine toothbrushing to removal of surface debris, ultrasoft brush, bland dentrifice
- 79. Analgesics Avoid tobacco, alcohol, condiments Report back in 1-2 days Motivation
- 80. SECOND VISIT Patient condition – usually improved. Pain is diminished or no longer present. Areas still erythematous but without pseudomembrane Shrinkage of gingiva – expose calculus which is then gently removed. Instruction same as previous visit
- 81. THIRD VISIT 5 days after 2nd visit Patient should be symptom free Repeat scaling and root planing Discontinue hydrogen peroxide mouthwash but continue CHX mouthwash Patient instructed in plaque control procedures Councelling on nutrition, habits
- 82. SUBSEQUENT VISITS Tooth surfaces in the involved areas are scaled. Plaque control is checked and corrected if required. Patient should now be scheduled for treatment of chronic disease.
- 83. GINGIVAL CHANGES WITH HEALING Removal of pseudo membrane – exposes red crater like hemorrhagic depression.(loss of normal barrier function of epithelium) Next day: Bulk and redness of crater margins reduced – but surface shiny.(reduction in inflammation and reepithelization)
- 84. Early signs of restoration of normal gingival contour and color. (further reduction in inflammation, reestablishment of normal barrier function including keratinization) Final stage- Normal gingival contour, colour, consistency are restored. Portions of roots exposed are covered by healthy gingiva
- 85. ADDITIONAL TREATMENT CONSIDERATIONS Countouring of gingiva as adjunctive procedure Shelf like margin Unesthetic, favours plaque retention Systemic antibiotics/topical antimicrobials Only in pts with systemic complications and local adenopathy Drug therapy—adjunctive to local debridement
- 86. Supportive systemic treatment Copious fluid consumption Administration of analgesics Bed rest
- 87. Nutritional supplements RATIONALE Lesions similar to NUG have been produced in animals – with certain nutritional deficiencies Difficulty in chewing raw fruits and vegetables may lead to selection of diet deficient in Vit B and C. Fewer recurrences – local treatment of NUG is supplemented by Vit B or C. Supplements may be discontinued after two months
- 88. PERSISTANT OR RECURRENT CASES Reassessment of differential diagnosis to rule out diseases that resemble NUG Underlying systemic disease causing immunosupression (HIV) Inadequate local therapy (mandibular anterior area due to pericoronal infection) Inadequate compliance
- 89. Pericoronitis Abscesses of the periodontium
- 93. CONTENTS Introduction Primary herpetic gingivostomatitis Necrotizing ulcerative gingivitis/ periodontitis (NUG) Pericoronitis Abscesses of periodontium Conclusion References
- 94. Pericoronitis
- 95. Inflammation of the gingiva in relation to the crown of an incompletely erupted tooth Mandibular third molar area
- 97. PATHOGENESIS Space- ideal area for accumulation of food debris and bacterial growth
- 98. Inflammatory fluid and cellular exudate Increase in bulk of the flap Interferes with complete closure of jaws or can be traumatized by contact with opposing jaw Aggrevation of the inflammatory involvement
- 99. CLINICAL FEATURES Chronic – no clinical signs or symptoms (chronic inflammation and ulceration on inner surface) Acute (trauma, occlusion, foreign body impaction) Inflammatory involvement +systemic complications
- 100. Red swollen suppurating lesion Tender Radiating pain to ear, throat, floor of mouth Foul taste Inability to close jaws Swelling of cheek, lymphadenitis, trismus Fever, leukocytosis, malaise
- 101. COMPLICATIONS Localized- pericoronal abscess Spread- submaxillary, posterior cervical, deep cervical and retropharyngeal lymph nodes Peritonsillar abscess, cellulitis, Ludwig’s angina Pericoronal abscess Peri-tonsillar abscess Ludwig’s angina
- 103. Chronic pericoronitis Removal as a preventive measure Acute pericoronitis Flushing area with warm water to remove debris and exudate Swabbing with antiseptic after elevating the flap gently Occlusal adjustment
- 104. Abscess drainage Antibiotics Decision to retain or extract the tooth after acute symptoms subside
- 105. Decision governed by likelihood of further eruption into good functional position, bone loss distal to second molars Extraction- Early extraction before root formation is completed
- 106. Retaining tooth- removal of pericoronal flap using periodontal knives or electrosurgery
- 107. incorrect correct healed site Surgical procedure to remove operculum
- 109. DEFINITION Periodontal abscess is defined as a lesion with expressed periodontal breakdown occuring during a limited period of time and with easily detectable clinical symptoms, and localized accumulation of pus within the gingival wall of the periodontal pocket (Hafstrom et al, 1994)
- 110. Independent disease entity (AAP world workshop, 1999) Represents period of active tissue breakdown due to extension of infection into intact periodontal tissues
- 111. CLASSIFICATION According to location (Meng et al, 1999) Gingival abscess Periodontal abscess Pericoronal abscess According to clinical signs and symptoms Acute abscess Chronic abscess
- 112. According to number Single Multiple (diabetes, immunosupression) Localized periodontal abscess in pt with poorly controlled type 2 diabetes mellitus
- 113. According to aetiology A) Periodontitis related abscess 1) Exacerbation of chronic lesion 2) Post therapy periodontal abscess a) Post scaling periodontal abscess (Dello Russo, 1985)— calculus impaction or obstruction b) Post surgery periodontal abscess (Garrett et al, 1997)– foreign body reaction, incomplete removal of calculus c) Post antibiotic periodontal abscess (no mechanical therapy, superinfection) Post scaling abscess
- 114. B) Non periodontitis related abscess 1) Impaction of foreign body in gingival sulcus 2) Root morphology alterations– invaginated root, fissured root, external root resorption, root tears, iatrogenic endodontic perforations
- 115. GINGIVAL ABSCESS Localized acute inflammatory lesion that may arise from a variety of sources such as microbial plaque infection, trauma and foreign body impaction Red, smooth, fluctuant, painful Marginal gingiva/interdental papilla
- 116. PERICORONAL ABSCESS o Associated with operculum of partially erupted tooth o Mandibular 3rd molars most frequently affected
- 117. PERIODONTAL ABSCESS A localized purulent infection within the tissues adjacent to the periodontal pocket that may lead to the destruction of periodontal ligament and alveolar bone In patients with untreated periodontitis Moderate to deep pockets
- 118. Acute exacerbation of chronic condition Incomplete calculus removal, antibiotic therapy, periodontal surgery Occlusion due to deep tortuous pocket, tooth morphology, debris, closely adapted pocket epithelium
- 119. ACUTE ABSCESS Exacerbation of chronic condition due to increase in number or virulence of bacteria combined with lowered tissue resistance and lack of spontaneous drainage Exudation Sensitivity to percussion Pain, Mobility Tooth elevation in socket Systemic involvement
- 120. CHRONIC ABSCESS Forms when spreading infection has been controlled by spontaneous drainage, host response or therapy No/dull pain Fewer/no symptoms Fistulous tract No systemic involvement
- 121. Periodontal Vs. Periapical Abscess Periapical Abscess •Non-vital tooth • Caries, restoration • No pocket • Apical radiolucency • No or minimal mobility • Percussion sensitivity • Sinus tract opens via alveolar mucosa •Severe, diffuse pain Periodontal Abscess •Vital tooth • No caries • Pocket, bone loss • Lateral radiolucency • Mobility • Percussion sensitivity variable • Sinus tract opens via keratinized gingiva •Dull localized pain
- 122. PREVALENCE 8-14% among all dental conditions needing emergency treatment (Ahl et al, 1986) Positively correlated with pocket depth High prevalence in molars- 50% (Smith and Davies, 1986) 3rd most frequent dental emergency
- 123. PATHOGENESIS AND HISTOPATHOLOGY Contains bacteria, bacterial products, inflammatory cells, tissue breakdown products and serum Occlusion of pocket lumen, extension of infection into soft tissues Entry of bacteria into soft tissue pocket wall
- 124. Accumulation of leukocytes, connective tissue destruction, bacterial encapsulation, formation of pus Central area Rate of tissue destruction depends on– growth and virulence of bacteria, Ph
- 125. MICROBIOLOGY Polymicrobial, mainly caused by endogenous bacteria (Tabaqhali, 1988) Similar to flora of chronic periodontitis Domination by gram negative, non-motile, strict anaerobic, rod-shaped species Pg
- 126. Pi, Tf, Fn, spirochetes (anaerobic species) Bifidobacterium spp, Actinomyces spp (gram positive, strict anaerobic) Aa, Capnocytophaga spp, Campylobacter spp (gram negative, facultative anaerobic)
- 127. DIAGNOSIS Clinical signs and radiological signs Ovoid elevation on lateral side of root Fistula, suppuration Pain, tenderness, swelling Sensitivitry to percussion
- 128. Mobility, tooth elevation, pocket Bone loss Systemic effects Use of dark field microscopy ( Trope et al, 1988) PET (Liu, 1996)
- 129. DIFFERENTIAL DIAGNOSIS Periapical abscess Lateral periapical cyst Vertical root fractures Endo-perio abscesses Parrish et al (1989)- 3 cases of osteomyelitis
- 130. TREATMENT 1) Resolving acute lesion 2) Management of the resulting chronic condition
- 131. ACUTE ABSCESS Drainage through pocket retraction or incision Scaling/ root planing Periodontal surgery Short term high dose adjunctive systemic antibiotics Tooth removal Avoid aggressive mechanical instrumentation in initial stage
- 132. Reduce exertion Fluid intake Chlorhexidine mouthwash Warm saline gargles Analgesics/antibiotics
- 133. Chronic abscess SPT, surgery/ antibiotics Gingival abscess Scaling/ root planing Drainage Removal of cause Warm saline gargles
- 134. Pericoronal abscess Drainage Irrigation to remove debris Warm saline gargles, antibiotics Analgesics Operculectomy/ extraction
- 136. COMPLICATIONS A) Tooth loss B) Dissemination of infection 1) Dissemination of bacteria inside the tissues during therapy 2) Bacterial dissemination through blood stream due to bacteriema from an untreated abscess
- 137. Pulmonary actinomycosis Brain abscess Cellulitis Cervical necrotizing fasciitis Necrotizing cavernositis
- 138. CONCLUSION Acute gingival infections lead to severe discomfort and may lead to life-threatening complications, and therefore they need to be treated promptly Adequate patient education and motivation is necessary as patients do not complete the treatment once the acute phase has subsided
- 139. REFERENCES o Newman, Takei, Klokkevold, Carranza: Carrazanza’s Clinical Periodontology, Saunders, 10th edition. o Acute necrotizing ulcerative gingivitis: risk factors involving host defense mechanisms.-- Yoji, Hidemi, Atsushi: Periodontology 2000, Vol. 6, 1994, 116-124. o Burkitt – Textbook of oral medicine o Shafer –Textbook of oral pathology
- 140. o Lindhe, Lang, Karring: Clinical Periodontology and Implant Dentistry. Blackwell Munksgaard, 5th edition. o The Periodontal abscess– A Review: Herrera et al, JCP 2000; 27: 377-386
Notes de l'éditeur
- primary