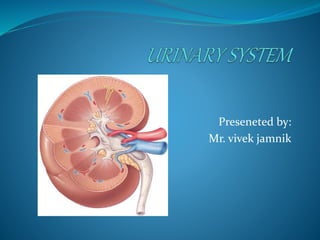
Uninary System
- 1. Preseneted by: Mr. vivek jamnik
- 2. URINARY STSTEM (Excretory system) The urinary system comprises the kidneys, ureters, bladder, and urethra. KIDNEY – regulate blood volume and composition, regulate pH, produce hormones and excrete waste URETERS- transport urine from kidney to urinary bladder URINARY BLADDER- store urine and expels through urethra URETHRA- discharge urine from the body
- 3. KIDNEY….. The kidneys are a pair of brownish-red structures bean-shaped appearance, located retroperitoneally (behind and outside the peritoneal cavity) on the posterior wall of the abdomen from the 12th thoracic vertebra to the 3rd lumbar vertebra in the adult An adult kidney weighs 120 to 150 gm and is 12cm long, 6 cm wide, and 2.5 cm thick. • The kidneys are well protected by the ribs, muscles, perirenal fat, and the renal capsule, which surround each kidney.
- 4. Position and relations Left Right Posterior Diaphragm (postero-superiorly) Quadratus lumborum (postero-laterally) Psoas major postero-medially Transversus abdominis postero-laterally Subcostal nerve and vessels Iliohypogastric and ilioinguinal nerves descend diagonally across posterior surface Anterior Lies with pancreas and spleen in the stomach bed Adrenal gland Stomach Spleen Pancreas (tail) Jejunum Descending colon Posterior wall of omental bursa Peritoneum Superiorly related to inferior surface of liver Descending part of duodenum Right colic (hepatic) flexure lies anterior to lateral border and inferior pole Small intestine (inferiorly) Peritoneum Medial L adrenal gland Right adrenal gland – wedged between superior pole and IVC IVC
- 5. STRUCTURE…. Each kidney is enclosed in a renal capsule, which is surrounded by adipose tissue. Internally, the kidneys consist of a renal cortex, renal medulla, renal pyramids, renal columns, major and minor calyces, and a renal pelvis. Blood enters the kidney through the renal artery and leaves through the renal vein.
- 6. The kidney consists of two distinct regions: Renal Parenchyma The renal parenchyma is divided into the cortex and the medulla. Renal Pelvis Renal Parenchyma The cortex contains the glomeruli, proximal and distal tubules, and cortical collecting ducts and their adjacent peritubular capillaries. The medulla resembles conical pyramids. The pyramids are situated with the base facing the concave surface of the kidney and the apex facing the hilum, or pelvis
- 7. CONTI….. The inner layer or Medulla is comprised of Renal Pyramids. The pyramids contain: • Medullary portions of Loops of Henle • Medullary Portions of Collecting Ducts Multiple pyramids taper and join forming a minor calyx. Several combined make a major calyx. The major calyces join and enter a funnel shaped renal pelvis that directs urine into the ureter.
- 8. Renal Pelvis pelvis, is the concave portion of the kidney through which the renal artery enters and the renal vein exits. The renal artery (arising from the abdominal aorta) divides into smaller and smaller vessels, eventually forming the afferent arteriole. The afferent arteriole branches to form the glomerulus, which is the capillary bed responsible for glomerular filtration. Blood leaves the glomerulus through the efferent arteriole and flows back to the inferior vena cava through a network of capillaries and veins.
- 9. Hilum At the concave part of each kidney Renal vein exits (anteriorly) Renal artery enters (posterior to renal vein) Renal pelvis exits (posterior to artery) Renal pelvis Funnel-shaped Lined with transitional epithelium with a smooth muscle and connective tissue wall Continuous inferiorly with ureter Divides into major and minor calyces Urine collecting tubule minor calyx major calyx renal pelvis ureters bladder
- 10. Cortex Beneath capsule, extends towards the pelvis as renal columns lying between pyramids of medulla Apices of several pyramids open together into a renal papilla, each of which projects into a renal calyx
- 11. ` Arterial supply Renal arteries branches of aorta at L1/L2 lie behind pancreas and renal veins Enter at hilum, giving rise to Anteriorly – apical, upper, middle and lower segments Posteriorly – posterior segment Venous drainage Renal veins Communicate widely Drain into IVC Lymphatic drainage • Para-aortic nodes at L1/L2
- 12. URETERS Urine, which is formed within the nephrons, flows into the ureter, a long fibromuscular tube that connects each kidney to the bladder. The ureters transport urine from the renal pelves of the right and left kidneys to the urinary bladder The ureters are narrow, muscular tubes, each 24 to 30 cm long, that originate at the lower portion of the renal pelvis and terminate in the bladder wall. pass beneath the urinary bladder, which results in the bladder compressing the ureters and hence preventing back-flow of urine when pressure in the bladder is high during urination.
- 13. The lining of the ureters is made up of transitional cell epithelium called urothelium. As in the bladder, the urothelium prevents reabsorption of urine. The movement of urine from the renal pelves through the ureters into the bladder is facilitated by peristaltic waves (occurring about one to five times per minute) from contraction of the smooth muscle in the ureter wall. “The left ureter is slightly shorter than the right”
- 14. Ureters There are three narrowed areas of each ureter: ureteropelvic junction ureteral segment ureterovesical junction
- 15. The angling of the ureterovesical junction is the primary means of providing antegrade, or downward, movement of urine, also referred to as efflux of urine. This angling prevents vesicoureteral reflux, which is the retrograde, or backward, movement of urine from the bladder, up the ureter, toward the kidney. ureterovesical junction
- 16. Bladder The urinary bladder is a muscular, hollow sac located just behind the pubic bone. The urinary bladder is posterior to the pubic symphysis The urinary bladder functions as a muscular sac that expands as urine is produced by the kidneys to allow storage of urine until voiding is convenient.
- 18. Toward the base of urinary bladder, the ureter drains into the urinary bladder via the ureteral opening. The bladder is characterized by its central, hollow area called the vesicle, which has two inlets (the ureters) and one outlet (the urethrovesical junction), which is surrounded by the bladder neck. The shape of urinary bladder depends on how much urine is contain. when empty, it look like a deflated balloon.
- 19. Capacity ~700-800 ml Smaller in female because, uterus occupies the space superior to the urinary bladder Bladder The wall of the bladder comprises four layers: adventitia detrusor lamina propria urothelium
- 20. The urothelium layer is specialized, transitional cell epithelium, containing a membrane that is impermeable to water. The urothelium prevents the reabsorption of urine stored in the bladder The bladder neck contains bundles of involuntary smooth muscle that form a portion of the urethral sphincter known as the internal sphincter. The portion of the sphincteric mechanism that is under voluntary control is the external urinary sphincter at the anterior urethra. urothelium
- 21. The urethra is a muscular tube that drains urine from the body; it is 3–4 cm long in females, but closer to 20 cm in males. The urethra arises from the base of the bladder: In the male, it passes through the penis; in the female, it opens just anterior to the vagina. In both male and female, the urethra is the passageway for discharging urine from the body. In the male, the prostate gland, which lies just below the bladder neck, surrounds the urethra posteriorly and laterally. Urethra
- 22. The male urethra also serves as the duct through which semen is ejaculated. Maindifference between the urinary systemof male and female is the “lengthof urethra.”
- 23. • Urine formation • Excretion of waste products • Regulation of electrolytes • Regulation of acid–base balance • Control of water balance • Control of blood pressure • Renal clearance • Regulation of red blood cell production • Synthesis of vitamin D to active form
- 24. NEPHRONS The functional unit of the kidney is called the nephron Each kidney contains about 1 million nephrons, the functional units of the kidney. Each kidney is capable of providing adequate renal function if the opposite kidney is damaged or becomes nonfunctional. Consist of 2 part: renal corpuscle, and renal tubule Renal corpuscle = glomerular (bowman’s capsule) glomerulus Renal tube Proximal convoluted tubules Nephron loop (descending & ascending) Distal convoluted tubules Collecting ducts converge into papillae, which empty into the minor calices, which drain into major calices that open directly into the renal pelvis.
- 25. Nephrons are struturally divided into two types: cortical and juxtamedullary.
- 26. FUNCTION OF NEPHRON Nephrons perform three basic tasks: glomerular filtration, tubular reabsorption, and tubular secretion. Together, the glomerular endothelium form a leaky filtration membrane that permits the passage of water and solutes from the blood into the capsular space. Blood cells and most plasma proteins remain in the blood because they are too large to pass through the filtration membrane. The pressure that causes filtration is the blood pressure in the glomerular capillaries.
- 28. Filtration Takes place through the semipermeable walls of the glomerular capillaries almost impermeable to proteins and large molecule Glomerular filtrate is formed by squeezing fluid through glomerular capillary bed Hydrostatic pressure (head of pressure) is controlled by afferent and efferent arterioles, and provided by arterial pressure About 20% of renal plasma flow is filtered each minute (125 ml/min). This is the glomerular filtration rate (GFR). Autoregulation
- 29. Tubular reabsorption 60% of solute is reabsorbed in proximal tubule Different parts of tubule system optimised to absorb different components of urine Distal tubule and collecting duct determines final urine concentration Regulated by ADH production by posterior pituitary
- 30. Hormones Renin Increases production of angiotensin II Aldosterone Stimulates water and sodium ion resorption in distal tubule Atrial natriuretic hormone (ANP) Produced when atrial pressure increases (eg heart failure) Promote Na+, Cl- and water loss Antidiuretic hormone Increases permability of distal tubule to water, to cinrease water resorption (therfore increases concentration of urine) 1,25 dihydroxy vitamin D3 Promotes calcium absorption from gut Erythropoietin (EPO) Stimulates marrow to produce red blood cells