Rebuilding anterior dental aesthetics
•
5 j'aime•792 vues
Marginal tissue recession
Signaler
Partager
Signaler
Partager
Recommandé
The Indian Dental Academy is the Leader in continuing dental education , training dentists in all aspects of dentistry and
offering a wide range of dental certified courses in different formats.for more details please visit
www.indiandentalacademy.comclinical, radiological , histopathological features, differential diagnosis a...

clinical, radiological , histopathological features, differential diagnosis a...Indian dental academy
Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADESH, INDIA.ORTHOGNATHIC CASE PRESENTATIONorthognathic Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR,...

orthognathic Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR,...CLOVE Dental OMNI Hospitals Andhra Hospital
Contenu connexe
Tendances
Tendances (20)
Fixed prosthodontics problems and solutions in dentistry

Fixed prosthodontics problems and solutions in dentistry
Diagnosis and treatment planning in removable partial denture

Diagnosis and treatment planning in removable partial denture
En vedette
The Indian Dental Academy is the Leader in continuing dental education , training dentists in all aspects of dentistry and
offering a wide range of dental certified courses in different formats.for more details please visit
www.indiandentalacademy.comclinical, radiological , histopathological features, differential diagnosis a...

clinical, radiological , histopathological features, differential diagnosis a...Indian dental academy
Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADESH, INDIA.ORTHOGNATHIC CASE PRESENTATIONorthognathic Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR,...

orthognathic Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR,...CLOVE Dental OMNI Hospitals Andhra Hospital
Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADESH, INDIA. TMJ TRAUMA CASE PRESENTATIONDr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADE...

Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADE...CLOVE Dental OMNI Hospitals Andhra Hospital
Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADESH, INDIA. TMJ ORTHOGNATHIC CASE PRESENTATIONDr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADE...

Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADE...CLOVE Dental OMNI Hospitals Andhra Hospital
Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADESH, INDIA. ORTHOGNATHIC CASE PRESENTATION13. orthognathicDr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNT...

13. orthognathicDr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNT...CLOVE Dental OMNI Hospitals Andhra Hospital
Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADESH, INDIA.ONCOLOGY CASE PRESENTATIONDr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADE...

Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADE...CLOVE Dental OMNI Hospitals Andhra Hospital
30. BILATERAL ANGLE #. N TEJA 15/M/ Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADESH, INDIA.TRAUMA CASE PRESENTATION 30. BILATERAL ANGLE #. N TEJA 15/M/ Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF ...

30. BILATERAL ANGLE #. N TEJA 15/M/ Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF ...CLOVE Dental OMNI Hospitals Andhra Hospital
En vedette (18)
clinical, radiological , histopathological features, differential diagnosis a...

clinical, radiological , histopathological features, differential diagnosis a...
orthognathic Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR,...

orthognathic Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR,...
Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADE...

Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADE...
Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADE...

Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADE...
13. orthognathicDr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNT...

13. orthognathicDr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNT...
Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADE...

Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADE...
30. BILATERAL ANGLE #. N TEJA 15/M/ Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF ...

30. BILATERAL ANGLE #. N TEJA 15/M/ Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF ...
Similaire à Rebuilding anterior dental aesthetics
3RD PUBLICATION - JCDR - Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIENCES, GUNTUR, ANDHRA PRADESH, INDIA. PUBLISHED LITERATURE3RD PUBLICATION - JCDR - Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIE...

3RD PUBLICATION - JCDR - Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIE...CLOVE Dental OMNI Hospitals Andhra Hospital
Similaire à Rebuilding anterior dental aesthetics (20)
SOCKET PRESERVATION TECHNIQUE- A Case Presentation.pptx

SOCKET PRESERVATION TECHNIQUE- A Case Presentation.pptx
Treatment of gingival recession using coronally advanced flap

Treatment of gingival recession using coronally advanced flap
Peri implantitis treatment with regenerative approach

Peri implantitis treatment with regenerative approach
full mouth rehabilitation of partially and fully edentulous patient with crow...

full mouth rehabilitation of partially and fully edentulous patient with crow...
Simultaneous vertical guided bone regeneration and guided tissue regeneration...

Simultaneous vertical guided bone regeneration and guided tissue regeneration...
connectivetissuegraftswithnonincisedpapillaesurgicalapproachforperiodontalrec...

connectivetissuegraftswithnonincisedpapillaesurgicalapproachforperiodontalrec...
Amato2019immediate loading of implant insertred through

Amato2019immediate loading of implant insertred through
3RD PUBLICATION - JCDR - Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIE...

3RD PUBLICATION - JCDR - Dr. RAHUL VC TIWARI, SIBAR INSTITUTE OF DENTAL SCIE...
Plus de Dr Gauri Kapila
Plus de Dr Gauri Kapila (13)
Association between alcohol consumption and periodontal disease

Association between alcohol consumption and periodontal disease
Correlation of the interdental and the interradicular bone loss

Correlation of the interdental and the interradicular bone loss
Desensitizing effect of a stabilized stannous fluoride and sodium hexametapho...

Desensitizing effect of a stabilized stannous fluoride and sodium hexametapho...
Dernier
Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent High Profile Call Girl 24×7
Booking Contact Details
WhatsApp Chat: +91-9930245274
Mumbai Escort Service includes providing maximum physical satisfaction to their clients as well as engaging conversation that keeps your time enjoyable and entertaining. Plus they look fabulously elegant; making an impressionable.
Independent Escorts Mumbai understands the value of confidentiality and discretion - they will go the extra mile to meet your needs. Simply contact them via text messaging or through their online profiles; they'd be more than delighted to accommodate any request or arrange a romantic date or fun-filled night together.
We provide -
Flexibility
Choices and options
Lists of many beauty fantasies
Turn your dream into reality
Perfect companionship
Cheap and convenient
In-call and Out-call services
And many more.
29-04-24 (Smt)Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent H...

Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent H...Call Girls in Nagpur High Profile
Dernier (20)
Call Girls Tirupati Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Tirupati Just Call 8250077686 Top Class Call Girl Service Available
Call Girls Faridabad Just Call 9907093804 Top Class Call Girl Service Available

Call Girls Faridabad Just Call 9907093804 Top Class Call Girl Service Available
College Call Girls in Haridwar 9667172968 Short 4000 Night 10000 Best call gi...

College Call Girls in Haridwar 9667172968 Short 4000 Night 10000 Best call gi...
Call Girls Gwalior Just Call 8617370543 Top Class Call Girl Service Available

Call Girls Gwalior Just Call 8617370543 Top Class Call Girl Service Available
Best Rate (Hyderabad) Call Girls Jahanuma ⟟ 8250192130 ⟟ High Class Call Girl...

Best Rate (Hyderabad) Call Girls Jahanuma ⟟ 8250192130 ⟟ High Class Call Girl...
The Most Attractive Hyderabad Call Girls Kothapet 𖠋 6297143586 𖠋 Will You Mis...

The Most Attractive Hyderabad Call Girls Kothapet 𖠋 6297143586 𖠋 Will You Mis...
Lucknow Call girls - 8800925952 - 24x7 service with hotel room

Lucknow Call girls - 8800925952 - 24x7 service with hotel room
Night 7k to 12k Chennai City Center Call Girls 👉👉 7427069034⭐⭐ 100% Genuine E...

Night 7k to 12k Chennai City Center Call Girls 👉👉 7427069034⭐⭐ 100% Genuine E...
(👑VVIP ISHAAN ) Russian Call Girls Service Navi Mumbai🖕9920874524🖕Independent...

(👑VVIP ISHAAN ) Russian Call Girls Service Navi Mumbai🖕9920874524🖕Independent...
Call Girls Nagpur Just Call 9907093804 Top Class Call Girl Service Available

Call Girls Nagpur Just Call 9907093804 Top Class Call Girl Service Available
Russian Escorts Girls Nehru Place ZINATHI 🔝9711199012 ☪ 24/7 Call Girls Delhi

Russian Escorts Girls Nehru Place ZINATHI 🔝9711199012 ☪ 24/7 Call Girls Delhi
Best Rate (Patna ) Call Girls Patna ⟟ 8617370543 ⟟ High Class Call Girl In 5 ...

Best Rate (Patna ) Call Girls Patna ⟟ 8617370543 ⟟ High Class Call Girl In 5 ...
Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent H...

Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent H...
Night 7k to 12k Navi Mumbai Call Girl Photo 👉 BOOK NOW 9833363713 👈 ♀️ night ...

Night 7k to 12k Navi Mumbai Call Girl Photo 👉 BOOK NOW 9833363713 👈 ♀️ night ...
Call Girls Gwalior Just Call 9907093804 Top Class Call Girl Service Available

Call Girls Gwalior Just Call 9907093804 Top Class Call Girl Service Available
Call Girls Jabalpur Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Jabalpur Just Call 8250077686 Top Class Call Girl Service Available
All Time Service Available Call Girls Marine Drive 📳 9820252231 For 18+ VIP C...

All Time Service Available Call Girls Marine Drive 📳 9820252231 For 18+ VIP C...
VIP Service Call Girls Sindhi Colony 📳 7877925207 For 18+ VIP Call Girl At Th...

VIP Service Call Girls Sindhi Colony 📳 7877925207 For 18+ VIP Call Girl At Th...
Call Girls Visakhapatnam Just Call 9907093804 Top Class Call Girl Service Ava...

Call Girls Visakhapatnam Just Call 9907093804 Top Class Call Girl Service Ava...
Best Rate (Guwahati ) Call Girls Guwahati ⟟ 8617370543 ⟟ High Class Call Girl...

Best Rate (Guwahati ) Call Girls Guwahati ⟟ 8617370543 ⟟ High Class Call Girl...
Rebuilding anterior dental aesthetics
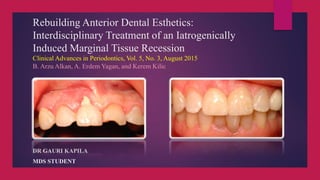
- 1. Rebuilding Anterior Dental Esthetics: Interdisciplinary Treatment of an Iatrogenically Induced Marginal Tissue Recession Clinical Advances in Periodontics, Vol. 5, No. 3, August 2015 B. Arzu Alkan, A. Erdem Yagan, and Kerem Kilic DR GAURI KAPILA MDS STUDENT
- 2. Clinical Presentation In July 2010, a 45-year-old female was referred to the Department of Endodontics, Faculty of Dentistry, Erciyes University, Kayseri, Turkey, with the complaint of severe pain in the maxillary right central incisor and poor esthetic appearance attributable to a fractured incisal edge of the neighboring left central incisor.
- 3. Clinical Presentation On clinical and radiographic examination, the tooth was diagnosed as having irreversible pulpitis, and endodontic therapy was initiated by an undergraduate student. During the preparation of the access cavity searching for the pulp chamber, the coronal root third was accidentally perforated at the labial surface of the tooth, resulting in an acute marginal tissue recession.
- 4. Clinical Presentation Root canal treatment was completed over 1 week in two sessions, and the perforation site was sealed with a temporary filling material (Fig. 1). The patient was referred to the the Periodontology Department for consultation 7 days after root perforation and completion of root canal therapy. Clinical periodontal examination revealed a 5-mm-deep and 3-mm-wide marginal tissue recession measured at the level of the cemento-enamel junction (CEJ) and 1 mm of enamel loss at the maxillary right central incisor.
- 5. Clinical Presentation Measurements of mid-labial probing depth (PD) = 1mm amount of keratinized gingiva = 5mm attached gingiva = 4 mm, respectively, at the maxillary right central incisor. There was no radiographic or clinical evidence of bone loss and soft tissue existed in the adjacent interproximal regions.
- 6. Case Management Oral informed consent was obtained from the patient prior to treatment. The Miller Class I marginal tissue recession (Fig. 2) was treated with subepithelial CT graft (SCTG) preceded by the simultaneous root surface restoration using a glass ionomer cement on the day of consultation. After local anesthesia, a split-thickness flap was reflected by using a no. 15C blade to create a pouch-like recipient bed to expose the root surface and the bony margins (Fig. 3).
- 7. Case Management No vertical incisions were made. A rubber dam was placed for isolation of the operative field. Minimal root preparation was performed to flatten the margins of the perforation. A resin ionomer restoration was placed following the manufacturer’s instructions to cover the entire defect.
- 8. Case Management The SCTG was harvested from the inner surface of a mucoperiosteal flap raised at the palatal premolar-molar region. Mattress and sling sutures crossing over the SCTG were used for the immobilization and tight adaptation of the soft-tissue graft to the root surface (Fig. 4).
- 9. Case Management A 5-0 polyglactin suture was used for this purpose, and the donor area was closed with 4-0 silk suture material. The patient was advised not to brush the treated site for 21 days. The patient was placed on 15 ml 0.12% clorhexidine gluconate twice daily for 3 weeks, and an analgesic (275 mg naproxen sodium, one tablet three times daily) and an antibiotic (625 mg amoxicillin, one tablet twice daily) were prescribed for 2 and 7 days, respectively.
- 10. Clinical Outcomes The sutures at the recipient and donor sites were removed 10 days after surgery. Follow-up visits were performed at 2, 4, 6, 8, and 12weeks and at 5 months after surgery. Total root coverage was obtained, but 1 mm of glass ionomer cement at the mid-labial enamel surface was evident.
- 11. Clinical Outcomes The mid-labial PD was the same as that of the baseline at final examination, and the width of keratinized tissue (KT) reached 10 mm (Table 1).
- 12. Clinical Outcomes Five months after surgery, the patient was referred to the Prosthodontics Department for the restoration of the maxillary central incisors using porcelain veneers (Figs. 6 and 7).
- 13. Discussion Endodontic claims are the most frequently filed malpractice claims in dentistry, and it is reported that errors frequently occur during instrumentation and root canal filling. Root perforation mostly occurs during access opening, as seen in this case report. The location of the perforation is the overriding factor in the decision-making process. Although perforations coronal to the crestal bone can frequently be managed non-surgically, apical third and critical crestal zone perforations may necessitate a surgical intervention. The root perforation in the present patient starts on the enamel 1mmcoronal to the CEJ and extended 5mmalong the root surface, resulting in an acute marginal tissue recession.
- 14. Discussion Regardless of the surgical technique performed to cover the exposed root surface, the restoration material of choice is important and should meet some criteria. In this context, GIC is insoluble in oral fluids and biocompatible with soft and hard tissues. Additionally, it releases fluoride, which may positively affect bacterial plaque chemistry. Successful treatment outcomes in terms of root coverage were reported in some cases. Although a histologic examination could not be performed for ethical reasons in the present case, it was reported that epithelium and connective tissue adhere to the resin ionomer when placed in a subgingival environment.
- 15. Discussion To the best of the authors’ knowledge, no study exists on the long-term stability of either the veneer adaptation over the glass ionomer or the glass ionomer subgingivally over time. The use of glass ionomer cement in combination with root coverage procedures appear in the literature in some case reports. For the management of soft tissue esthetics before any restorative treatment, an SCTG procedure was considered as a treatment option. A width of 5 mm of KT was present mid-labially apical to the gingival margin.
- 16. Discussion Indeed, this amount of KT was quite enough to cover the SCTG completely by a double papilla pedicle or coronally positioned flap. However, a high frenum attachment extending corono-apically just in the proximity of recession borders could have jeopardized the immobilization of any pedicle flap used to cover the graft. Therefore, the SCTG was placed into the pouch-like recipient bed prepared by split-thickness flap. No problem occurred with the survival of the CT graft. Total root coverage was maintained at 5 months after surgery. Excellent color match of the veneers with the neighboring teeth satisfied both the patient and the clinicians and restored anterior esthetics.
- 17. Conclusion In conclusion, dental practitioners will continue to be faced with endodontic perforations as a result of anatomic variations, technical deficiency, or simply a clinician’s insufficient knowledge, skill, and experience performing the procedure. Whatever the cause is, saving the tooth is the first mission of the clinician. In the case of the deterioration of anterior dental esthetics, an interdisciplinary approach can successfully restore both esthetics and function, as described this case report.
- 18. Strengths of the article Excellent esthetic clinical outcomes achieved following a multidisciplinary treatment approach. Clearly mentions the treatment steps involved in a complex malpractice case. Encourages communication among dental professionals from different specialties.
- 19. Limitations of the article Technique of harvesting the SCTG was not mentioned clearly. Not all sizes and different locations of the root perforation can be treated with this approach. A great quality of clinician’s skill is required.
- 20. THANK YOU
