Lower limb peripheral vascular disease
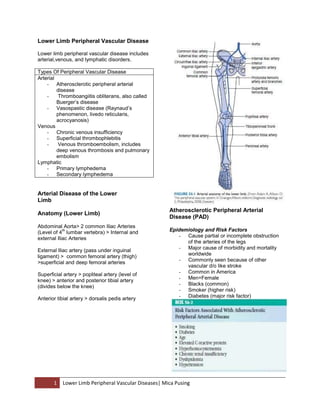
- 1. Lower Limb Peripheral Vascular Disease Lower limb peripheral vascular disease includes arterial,venous, and lymphatic disorders. Types Of Peripheral Vascular Disease Arterial - Atherosclerotic peripheral arterial disease Thromboangiitis obliterans, also called Buerger’s disease - Vasospastic disease (Raynaud’s phenomenon, livedo reticularis, acrocyanosis) Venous - Chronic venous insufficiency - Superficial thrombophlebitis Venous thromboembolism, includes deep venous thrombosis and pulmonary embolism Lymphatic - Primary lymphedema - Secondary lymphedema Arterial Disease of the Lower Limb Anatomy (Lower Limb) Abdominal Aorta> 2 common Iliac Arteries th (Level of 4 lumbar vertebra) > Internal and external Iliac Arteries External Iliac artery (pass under inguinal ligament) > common femoral artery (thigh) >superficial and deep femoral arteries Superficial artery > popliteal artery (level of knee) > anterior and posterior tibial artery (divides below the knee) Anterior tibial artery > dorsalis pedis artery 1 ARTERIAL DISEASES Atherosclerotic Peripheral Arterial Disease (PAD) Epidemiology and Risk Factors - Cause partial or incomplete obstruction of the arteries of the legs - Major cause of morbidity and mortality worldwide - Commonly seen because of other vascular d/o like stroke - Common in America - Men=Female - Blacks (common) - Smoker (higher risk) - Diabetes (major risk factor) Lower Limb Peripheral Vascular Diseases| Mica Pusing
- 2. (paleness of the skin), paresthesia, paralysis present for less than 2 weeks requires emergent vascular surgery> must be done to prevent irreversible tissue loss - embolectomy, thrombolysis, st amputation(30% in the 1 month of presentation) Critical Limb Ischemia - ischemia> more than 2 weeks - causes rest pain, ischemic ulcer and gangrene - begins once toe pressure falls to less that 30 to 50 mm Hg - rest pain : toe pressure falls 30mmHg - higher pressure is needed to heal wound than needed to maintain intact skin - 40mmHg: asymptomatic, intact skin, develop nonhealing ischemic ulcer after minor trauma Evaluation - Clinical Presentation - asymptomatic, intermittent claudication (IC), critical limb ischemia (CLI), and acute limb ischemia, with the most common being asymptomatic Clinical Presentation of PAD -Asymptomatic (most common) -Intermittent claudication: Reproducible paon in the lower limb with exertion that resolves quickly with rest -Acute limb ischemia: a sudden decrease in limb perfusion that threatens loss of the limb -Critical limb ischemia: chronic ischemia that causes either rest pain or wounds. Asymptomatic - complete occlusion was found in 1/3 of pt. - lack of symptoms is due to low physical ax - functional impairment is present - functional decline is related to anklebrachial index (ABI) Intermittent Claudation(IC) - leg pain with exertion that is relieves with rest - claudation produces ischemia in the affected muscle > pain - pain can be felt in : buttock, hip, thigh, calf, or foot - limits the pt. ability to walk - decreased walking speed and distance - decreased leg function Acute Limb Ischemia - can be caused by embolism, thrombosis or dissection - limb threatening medical emergency - pt. present with pain, poikilothermia(disruption of normal hypothalamic thermoregulatory function), pulselessness, pallor 2 - functional history should be taken to include mobility, activities of daily living, and independent activities of daily living. - The presence of risk factors for PAD must be noted - physical examination: lower limb pulses (evaluated) including the dorsalis pedis, posterior tibial, popliteal, and femoral. - legs and feet: changesof skin temperature, color, and evidence of poor vascular flow. - Dreased blood flow> atrophy thin shinny skin, decreased hair growth, nails are thickand brittle; foot >red or purple; pallor when elevated Vascular Testing for Peripheral Arterial Disease Ankle–Brachial Index. - compares the brachial systolic pressure with the ankle systolic pressure - 95% sensitive in detecting PAD - Obtained in pt. 70, patients aged 50 to 69 who have cardiovascular risk factors Toe Pressures - obtained by placing asmall cuff on the first or second toe. - For pt, with elevated ABI - .7 : abnormal Segmental Limb Systolic Pressure Measurement - taken in the thigh, calf, and ankle - Occlusive disease is noted by a significant decrease in systolic pressure Lower Limb Peripheral Vascular Diseases| Mica Pusing
- 3. Segmental Plethysmography (Pulse Volume Recordings) - recordings are obtained at the thigh, calf, and ankle. Occlusive lesions are detected by a change in waveform from one level to the next. Doppler Velocity Waveform Analysis - performed to localize the lesion Transcutaneous Partial Pressure of Oxygen - test to predict wound healing - usedto select amputation level - TcPo2 less than 30 mm Hg : poor wound healing - TcPo2 above 40mm Hg : adequate skin perfusion for healing Angiography - gold standard imaging test for PAD - used to visualize the arterial anatomy and the extent of PAD before revascularization procedures. Magnetic Resonance Angiography - safer - sensitivity and specificity are greater than 90% for evaluating PAD Multidetector Computed Tomography Angiography. - Faster and safer as compared to MRA Management Patients with PAD are more likely to have coronary artery disease and cerebral artery disease than patients without PAD. goals of tx: - reduce ischemic symptoms, - increase walking ability improve function, prevent and heal wounds - prevent limb loss - reduce morbidity and mortality management - education - risk factor modification - pharmacotherapy, - exercise - vascular interventions Risk Factor Modification Includes: smoking cessation, - - weight reduction control of hyperlipidemia, hypertension, and diabetes smoking cessation: 3 - can reduce their risk of amputation and cardiovascular events even if it does not improve claudication symptoms Pain Management - diabetic neuropathy: impair sensation enough that the pt cannot feel ischemic pain - ischemic pain relieved by reperfusion - opiates for pain control - pt that develop rest pain at night when they lie down and find that keeping the foot in a dependent position provides relief Wounds - ischemic wounds are best treated with reperfusion of the limb - tissue might not have sufficient blood supply to repair itself after the trauma of debridement. - Dry gangrene can be allowed to autoamputate as long as there is no evidence of infection and there is adequate perfusion to support healing of the underlying tissue - Dependent rubor : fade with elevation and is not associated with induration or increased warmth. erythema of cellulitis is often associated with induration, increased warmth, swelling, and does not fully resolve with elevation of the limb. Exercise - improve walking time and walking distance in PAD patients Foot Protection - Footwear should have enough length, breadth, and depth to prevent pressure on any bony prominences, deformities, or calluses Surgical Intervention - Open surgical bypass is used in more diffuse lesions. - surgical interventions include limb salvage and amputation Arteriosclerosis Obliterans - - disease commonly present because of symptoms of intermittent claudication or critical leg ischemia intermittent claudication: active Pts describe claudication as numbness, weakness, giving way, aching, cramping, or pain Lower Limb Peripheral Vascular Diseases| Mica Pusing
- 4. - - inactive: rest pain, ulceration, dependent rubor, or gangrene may be the presenting findings symptoms occur distal to the level of stenosis - Angioplasty - indicated for focal stenosis or short Tx Risk factor modification major risk factors for peripheral arterial occlusive disease: - age - diabetes mellitus current smoking status(2x risk) alterations in lipid metabolism Hypertension elevated plasma homocysteine levels - elevated fibrinogen levels Antiplatelet Therapy - decrease the rate of atherosclerotic disease progression, decrease the incidence of thrombotic events in the limbs, and decrease the rate of adverse coronary and cerebral vascular ischemic events Rehabilitation General Self-Care Measures - instructed to monitor their extremities carefully for redness or skin breakdown - Extremes of temperature should be avoided - Wash feet with mild soap and warm water - Rubbing when drying the foot is avoided since it can injure the skin - Skin bet toes should be dried to avoid maceration - Prevent the cracking of skin - Proper foot wear - Decrease activity Exercise - Elicit maximum walking time - Should receive structured claudication ex rehab program for at least 3 sessions weekly over a period of 12 weeks 4 instruct to walk until claudication occurs, rest until it subsides, and continue repeating the cycle for 1 hour each day. - - segmental occlusions in which the adjacent vessels are relatively free of disease localized stenosis of the common iliac artery (less than 5 cm in length) is the most favorable situation for angioplasty decrease effectiveness in distal vessel surgical revascularization - - considered in patients with rest pain, impending tissue loss, or significant limitation of lifestyle Pedal bypass grafting for critical limb ischemia is a durable procedure with acceptable graft patency and a very good limb salvage rate Intermittent Pneumatic Compression - Skin blood flow, as reflected by TcPO - External compression briefly raises tissue pressure, emptying the underlying veins and transiently reducing venous pressure without occluding arterial blood flow Epidural Spinal Cord Stimulation (SCS) - may decrease ischemic limb pain and enhance perfusion - result from vasodilation, possibly through an effect on resting sympathetic tone Acute Arterial Occlusion - - - three causes: o thrombosis o aortic dissection o emboli thrombosis o insitu occurs at the site of the vascular abnormality, Dissection o Aotic dissection associated to hypertention arthrosclerosis, Lower Limb Peripheral Vascular Diseases| Mica Pusing
- 5. connective tissue disorders, trauma - Emboli o Large enough to occlude large arteries typically cardiac source o Arterial embolus unusual cause paradoxic embolus(DVT>pass foramen ovale) o Multiple ad recurrent Other Arterial Diseases UPPER EXTREMITY ISCHEMIA - Coldness and color changes: presenting sx Thromboangiitis Obliterans (Buerger’s Disease) - nonatherosclerotic PAD affecting young male smokers - inflammatory disease that affects smalland medium-sized arteries of the upper and lower distal extremities - considered to be a form of vasculitis - M>F - Higher risk for smokers - high risk for amputation as compared to PAD Clinical Presentation, Evaluation, and Diagnosis of Thromboangiitis Obliterans - legs are more involved than the arms, however, three or four limbs involved when assessed with angiography - Allen test to assess for asymptomatic involvement of the upper extremities; (+) indicates small artery disease in the upper limbs but is not specific to TAO Management of Thromboangiitis Obliterans - Smoking cessation is key to disease management Vasospastic Disease (Raynaud’s Phenomenon, Livedo Reticularis,Acrocyanosis) Raynaud’s Phenomenon - pain, and numbness in the fingers and sometimes the toes - triggered by cold temperatures, emotional stress, vibration, or anything that activates the sympathetic nervous system - Secondary Raynaud’s phenomenon is associated with other disorders, such as connective tissue diseases such as scleroderma and lupus - Patients should be instructed to keep the whole body warm, avoid sudden decreases in temperature, stop smoking, avoid caffeine, avoid sympathomimetic drugs, and reduce stress Livedo Reticularis - seen on the arms and legs and occasionally the trunk - common in young women - trigeer: cold Acrocyanosis - causes the hands and feet to be bluish and cold but is not painful common in young women aggravated by cold exposure episodic Venous Disorders of the Lower Limb Peripheral venous disorders include the following conditions: 1. Chronic venous insufficiency (CVI) and venous leg ulcers 2. Superficial thrombophlebitis 3. Deep venous thrombosis (DVT) 4. VTE, which is a collective term for DVT with pulmonary embolism (PE) Chronic Venous Insufficiency Epidemiology of Chronic Venous Insufficiency - 2x common in women but severity is higher in men - Predisposing factor: o o o more common in young women and those with a family history of the disorder affect both hand and feet but affect hand more often occurs when the normal vascular response becomes exaggerated causes color changes, o o Pathogenesis 5 Lower Limb Peripheral Vascular Diseases| Mica Pusing prolonged standing, obesity, positive family history, multiparity, advanced age, historyof leg injury, surgery, heart failure, paralysis, and DVT
- 6. o - - - persistent ambulatory venous hypertension in the superficial and deep venous systems in the lower limbs Normal functioning of the venous blood flow system depends on competent valves, calf muscle pump mechanism, and normal venous anatomy Incompetence in any valves disrupts the unidirectional flow of blood from the superficial to the deep systems and toward the heart, resulting in ambulatory venous hypertension Clinical Features - - - - Initial complaints can be purely cosmetic Chief clinical manifestation: dilated leg veins, edema, leg pain, skin pigmentation, subcutaneous fibrosis, dermatitis, and ulceration Patients can describe heaviness and aching in the legs with prolonged standing. The pain is usually localized to the calf or along the varicose veins and is relieved by walking or lying down with the leg elevated. deep venous system obstruction can experience venous claudication, a mild aching sensation at rest that becomes an intense cramping-type sensation in the calf with ambulation cutaneous manifestation: o brownish pigmentation (perimalleolar area) o reddish purple hue (from venous engorgement and obstruction) Diagnostic Evaluation - Duplex ultrasound scanning has become the test of choice for evaluation (allows identification of any underlying unrecognized acute or subacute DVT, as well as the site and type of pathology causing the CVI Management - - - limb elevation is used for edema control, patients should be instructed to elevate the limb above heart level. Periodic elevation of the leg 20 cm above heart level during the day has been shown to relieve edema by effectively lowering the hydrostatic pressure to nearly zero Compression stockings 6 reduce superficial venous volume and venous hypertension, assist calf muscle pump, and help prevent transcapillary leakage of fluid into the interstitial tissue - Contraindications for compression therapy include arterial insufficiency with ABI of less than 0.6, ankle pressure less than 60 mm Hg, active skin disease, or allergy to any of the stocking components - Physiologically, intravenous pressure in the leg vein reflects the weight of the blood column between the site of measurement and the right atrium - In the supine position: leg vein pressure: bet. 10-20 mmHg > total occlude at pressure of :20-25mmHg - Thromboembolic stockings exert a pressure between 14 and 20 mm Hg. - During standing, intravenous pressure in the lower leg veins: around 60 mm Hg, depending on the height of the individual. - An external pressure of 35 to 40 mm Hg has been shown to narrow the veins in the standing position, and 60 mm Hg will totally occlude the veins in the standing position. - For mild disease and those with underlying arterial disease, compression stockings with 20 to 30 mm Venous Ulceration - disabling complication of CVI most often large, irregular in shape, and have a flat wound edge with a shallow moist ruddy or beefy granulation base - risk is highest when the ambulatory venous pressure is 80mm Hg or greater - Compression therapy is the mainstay of treatment and is aimed at lessening the impact of the underlying venous insufficiency Superficial Thrombophlebitis - - treated with elevation, superficial heat, and ambulation with 30 to 40 mm Hg compression stockings. Nonsteroidal anti-inflammatory drugs are useful in reducing pain and limiting local inflammation Venous Thromboembolism Epidemiology - primarily a disease of old age incidence increases with age Lower Limb Peripheral Vascular Diseases| Mica Pusing
- 7. - Male to female ratio = 1.2:1 Higher in women in childbearing yrs Higher incidence in African American and whites - - Pathogenesis - Primary or idiopathic DVT occurs in the absence of recognized thrombotic risk factors - secondary DVT occurs in the presence of known risk factors - Virchow’s Triad o venous stasis o vessel wall injury o variation in coagulability of the blood (important contributor in pathogenesis of DVT) - Thrombi usually begin to form at low flow sites (deep veins of the calf, soleus sinuses, behind the cusps of venous valves, and at the entrance of tributary veins) Risk factos associated with virchows triad stasis Hypercoagulable Endothelial state injury Age(>60) Estrogenic PostOp state medication Immobility Pregnancy Cenous acess Paralysis Cancer Trauma, burns HR/ Family HX Spinal cord Myocardial injury infarction Anesthesia Sepsis Sepsis in past surgery Obesity Inherited vasculitis hypercoagulable state Long Factor v leiden Prior DVT distance mutation travel - - Surgery of hip and knee, venous catheterization, and burns can cause vessel wall damage that initiates thrombus formation Venous thrombi consist of deposit of fibrin, red cells, platelets and leukocytes Most clinically significant PE originates from DVT of the proximal lower limb (popliteal, femoral, or iliac veins) Clinical Features of Venous Thromboembolism 7 - - Classic signs of edema, erythema, warmth, tenderness, and positive Homan’s sign are nonspecific and might not be always present Patients can present with unilateral edema and tenderness confined to the calf muscle or along the distribution of the deep veins of medial thigh without any other signs. A 3-cm or greater difference in calf circumference 10 cm below the tibial tuberosity is associated with a high likelihood of having DVT Patients with obstructive iliofemoral thrombosis can present with a markedly swollen, cyanosed leg or with a white, cold leg if there is associated arterial spasm Diagnostic Evaluation of Venous Thromboembolism Duplex Ultrasound for Deep Venous Thrombosis - choice for detection of DVT Magnetic Resonance Venography 100% sensitivity in diagnosis - of DVT proximal to the inguinal ligament - safe to use in pregnant women - concern: in pt with renal insufficiency D-Dimer Assay - Elevated levels of d-dimer occur with acute thrombosis, but this does not discriminate between physiologic (e.g., postoperative or posttrauma) or pathologic (e.g., deep vein) thrombi Diagnostic Testing for Pulmonary Embolism Ventilation Perfusion Scintigraphy A normal study can effectively rule out clinically important PE. Spiral Computed Tomography. - It is minimally invasive compared with pulmonary angiography but allows visualization of pulmonary vessels, parenchyma, pleura, and mediastinum. Pulmonary Angiography - costly, invasive, technically demanding, and has significant radiation exposure. Treatment of Acute Venous Thromboembolism - goals of treatment: o prevent PE o recurrent VTE, o postphlebitis syndrome Lower Limb Peripheral Vascular Diseases| Mica Pusing
- 8. - Anticoagulation is the mainstay of treatment, and the treatment regimen is similar to that for DVT and PE Ambulation After DVT - Adjunctive therapy with graduated belowknee stockings with 30 to 40 mm Hg pressure at the ankle is indicated after proximal DVT. Lymphatic Disease in the Lower Limbs - - - - - - - lymphatic vasculature is divided into superficial and deep systems located in the popliteal fossa and the inguinal region superficial system : from the skin and subcutaneous tissues deep system: muscles and joints lymph has no valve lymph capillaries flows into the lymph precollector then collectors lymph angion o a segment of a lymph collector located between two valves o Contain smooth muscle o Contract around 10-12 time/min at rest Lymphangiomotoricity o frequency and amplitude of these contractions o affected by : internal stretch, temperature, hormones, external stretch from manual lymph drainage or muscle or joint pump during exercise Lymphedema o caused by a defect in the lymphatic system that leads to protein-rich interstitial fluid overload. primary lymphedema o Hereditary and congenital types o Less common o Divided into three major types: congenital, lymphedema praecox, lymphedema tarda Congenital lymphedema o Onset in the first 1-2 years of life o Bilateral o Aplastic lymphatics o Due to gene defect hat involves lymphathogenesis Lymphadema praecox o Onset between 1-35 y/o o Hypoplastic lymphatics o Unilateral 8 - - Lymphadema tard o Onset is after age of 35 o Week lymphatics unable to compensate when stresses with overload injury Secondary lympedema o Most common type o Usually caused by canser o Unilateral pain swelling o Precaution Meticulous skin care Meticulous nail care Avoid anything that cause swelling (needle sticks, blood pressure cuff, tight clothing, leaving the leg in dependent position for long period) o Clinical presentation Pitting edema but becomes nonpitting(tissue become fibrotic) Pt. complains limb feels heavy and stiff o Complication Cellulitis Lymphangitis Lymphangiosarcoma o Treatment goals Improve function of limb Prevent complication Improve quality of life o The treatment phase involves sessions 5 days/wk and includes manual lymph drainage (MLD), exercise, skin and nail care, and compression. MLD consists of light strokes to help stimulate lymph production and transport o The bandages should not be removed and should be worn until the next treatment session. Exercise is performed twice a day for 15 minutes while wearing compression bandages o Once the patient has reached maximum limb reduction, therapy moves from the initial treatment phase to the maintenance phase o The maintenance phase is a lifelong process of preventing reaccumulation of lymphedema and protecting the skin Reference Lower Limb Peripheral Vascular Diseases| Mica Pusing
- 9. Physical medicine and rehabilitation 4th edition by Braddom 9 Lower Limb Peripheral Vascular Diseases| Mica Pusing
