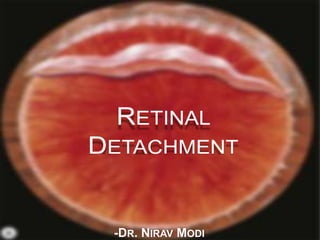
Retinal detachment presentation
- 2. DEFINITION A Retinal Detachment (RD) describes the separation of the neurosensory retina (NSR) from the retinal pigment epithelium (RPE). This results in the accumulation of sub-retinal fluid (SRF) in the potential space between the NSR and RPE.
- 3. TYPES There are three types of retinal detachment: 1) Rhegmatogenous 2) Tractional 3) Exudative
- 5. Rhegmatogenous retinal detachment occurs due to a break in the retina (called a retinal tear) Retinal breaks are the predisposing lesions than can go into RRD. These retinal breaks can be of 3 types Retinal Tear. Retinal Hole, Retinal Dialyses,
- 6. PATHOGENESIS Presence of retinal break in concert with Vitreo-retinal traction allows accumulation of liquefied vitreous under the Neuro-Sensory retina, separating it from RPE. Even though Retinal break is present, at least partially liquefied vitreous and/or traction must be there. Vitreous degeneration, PVD, Lattice degeneration, Snail-track degeneration, WWP, high myopic eyes & vitreous loss during cataract or YAG capsulotomy are predisposing.
- 7. Symptoms 1) Photopsia is the subjective sensation of a flash of light. In eyes with acute PVD it is probably caused by traction at sites of vitreoretinal adhesion. The cessation of photopsia is the result of either separation of the adhesion or complete tearing away of a piece of retina (operculum). Patient will often describe it as an arc of golden or white light induced by eye movements and is more noticeable in dim illumination.
- 8. 2) Floaters are moving vitreous opacities which are perceived when they cast shadows on the retina. Vitreous opacities in eyes with acute PVD are of the following three types: Weiss ring is a solitary floater consisting of the detached annular attachment of vitreous to the margin of the optic disc. Vitreous Hemorrhage secondary to tearing of a peripheral retinal blood vessel is indicated by sudden shower of minute red-coloured or dark spots. Usually Vitreous haemorrhage here is usually sparse due to the small calibre of peripheral retinal vessels.
- 9. 3) Visual field defect is perceived as a ‘black curtain’. In some patients it may not be present on waking in the morning, due to spontaneous absorption of SRF while lying inactive overnight, only to reappear later in the day. A lower field defect is usually appreciated more quickly by the patient than an upper field defect. The quadrant of the visual field in which the field defect first appears is useful in predicting the location of the primary retinal break, which will be in the opposite quadrant.
- 10. LINCOFF’S RULES A shallow inferior RD in which the SRF is slightly higher on the temporal side points to a primary break located inferiorly on that side A primary break located at 6 o’clock will cause an inferior RD with equal fluid levels In a bullous inferior RD the primary break usually lies above the horizontal meridian If the primary break is located in the upper nasal quadrant the SRF will revolve around the optic disc and then rise on the temporal side until it is level with the primary break A subtotal RD with a superior wedge of attached retina points to a primary break located in the periphery nearest its highest border When the SRF crosses the vertical midline above, the primary break is near to 12 o’clock, the lower edge of the RD corresponding to the side of the break
- 12. SIGNS 1) Marcus Gunn pupil (relative afferent pupillary defect) is present in an eye with an extensive RD irrespective of the type. 2) Intraocular pressure is usually lower by about 5 mmHg compared with the normal eye. If the intraocular pressure is extremely low, an associated choroidal detachment may be present. 3) Iritis is very common but usually mild. 4) Tobacco dust consisting of pigment cells is seen in the anterior vitreous.
- 13. 5) Retinal breaks are usually red because of the colour contrast between the sensory retina and underlying choroid. However, in eyes with hypo-pigmented choroid (as in high myopia), the colour contrast is decreased and small breaks may be missed.
- 14. FRESH RETINAL DETACHMENT 1) The RD has a convex configuration and a slightly opaque and corrugated appearance as a result of retinal oedema. There is loss of the underlying choroidal pattern and retinal blood vessels appear darker than in flat retina. 2) SRF extends up to the ora serrata, except in the rare cases caused by a macular hole in which the SRF is initially confined to the posterior pole. Because of the thinness of the retina at the fovea, a pseudohole is frequently seen if the posterior pole is detached. This should not be mistaken for a true macular hole, which may give rise to RD in highly myopic eyes or following blunt ocular trauma. 3 B-scan ultrasonography shows good mobility of the retina and vitreous.
- 15. (A)U-tear (B) Superior bullous RD (C) Shallow temporal RD (D) B-scan- totally detached retina with open funnel
- 16. LONG-STANDING RETINAL DETACHMENT 1) Retinal thinning secondary to atrophy is a characteristic finding which must not be mistaken for retinoschisis. 2) Secondary intra-retinal cysts may develop if the RD has been present for about 1 year; these tend to disappear after retinal reattachment. 3) Subretinal demarcation lines ‘‘high water marks’’ caused by proliferation of RPE cells at the junction of flat and detached retina are common and take about 3 months to develop. They are initially pigmented but tend to lose this with time. Demarcation lines are convex with respect to the ora serrata and, although they represent sites of increased adhesion, they do not invariably limit spread of SRF.
- 17. Long-standing RD (A) Secondary retinal cyst. (B) B-scan shows a retinal cyst (C) ‘high water mark’ in an eye with an inferior RD
- 18. PROLIFERATIVE VITREO-RETINOPATHY Proliferative vitreoretinopathy (PVR) is caused by epiretinal and subretinal membrane formation. Cell-mediated contraction of these membranes causes tangential retinal traction and fixed retinal folds. Usually, PVR occurs following surgery for rhegmatogenous RD or penetrating injury. However, it may also occur in eyes with rhegmatogenous RD that have not had previous vitreoretinal surgery. The main features are retinal folds and rigidity so that retinal mobility induced by eye movements or scleral indentation is decreased.
- 19. ADVANCED PVR WITH FUNNEL LIKE RD
- 21. Exudative, Serous or Secondary Occurs due to inflammation, injury or vascular abnormalities. Fluid accumulating underneath the retina without the presence of a hole, tear, or break. Rare
- 22. PATHOGENESIS Exudative RD occurs in a variety of vascular, inflammatory and neoplastic diseases involving the NSR, RPE and choroid in which fluid leaks outside the vessels and accumulates under the retina. As long as the RPE is able to compensate by pumping the leaking fluid into the choroidal circulation, no fluid accumulates in the sub-retinal space and RD does not occur. But if the normal RPE pump is overwhelmed or if the RPE activity is decreased, then fluid starts to accumulate in the sub-retinal space
- 23. The main causes are the following: 1) Choroidal tumours such as melanomas, haemangiomas and metastases; it is therefore very important to consider that exudative RD is caused by an intraocular tumour until proved otherwise. 2) Inflammation such as Harada disease (Part of VKH syndrome) and posterior scleritis. 3) Bullous central serous chorioretinopathy is a rare cause. 4) Iatrogenic causes include retinal detachment surgery and panretinal photocoagulation. 5) Subretinal neovascularization which may leak and give rise to extensive subretinal accumulation of fluid at the posterior pole. 6) Hypertensive choroidopathy, as may occur in toxaemia of pregnancy, is a very rare cause. 7) Idiopathic such as the uveal effusion syndrome.
- 24. Symptoms: Photopsia is absent because there is no vitreoretinal traction, although floaters may be present if there is associated vitritis. The visual field defect may develop suddenly and progress rapidly. Depending on the cause both eyes may be involved simultaneously (e.g. Harada disease).
- 25. Signs : The RD has a convex configuration, just like a rhegmatogenous RD, but its surface is smooth and not corrugated. The detached retina is very mobile and exhibits the phenomenon of ‘shifting fluid’ in which SRF responds to the force of gravity and detaches the area of retina under which it accumulates. For example, in the upright position the SRF collects under the inferior retina, but on assuming the supine position for several minutes, the inferior retina flattens and the SRF shifts posteriorly detaching the superior retina.
- 26. The cause of the RD, such as a choroidal tumour, may be apparent when the fundus is examined, or the patient may have an associated systemic disease responsible for the RD (e.g. Harada disease, toxaemia of pregnancy). ‘Leopard spots’ consisting of scattered areas of sub-retinal pigment clumping may be seen after the detachment has flattened.
- 27. Exudative RD showing shifting fluid. (A)Inferior collection of sub-retinal fluid with the patient sitting; (B) the subretinal fluid shifts upwards when the patient assumes the supine.
- 28. Exudative RD caused by Choroidal melanoma
- 30. Tractional retinal detachment occurs when fibrous or fibro-vascular tissue, pulls the sensory retina from the retinal pigment epithelium.
- 31. Main causes of tractional RD are (a) proliferative retinopathy such as diabetic and retinopathy of prematurity, (b) penetrating posterior segment trauma
- 32. PATHOGENESIS 1) Tractional RD is caused by progressive contraction of fibrovascular membranes over large areas of vitreoretinal adhesion. It is thought to be caused by leakage of plasma constituents into the vitreous gel from a fibrovascular network adherent to the posterior vitreous surface. Owing to the strong adhesions of the cortical vitreous to areas of fibrovascular proliferation, PVD is usually incomplete. In the very rare event of a subsequent complete PVD,the new blood vessels are avulsed and RD does not develop
- 33. 2) Static vitreo-retinal traction of the following three types is recognized. A) Tangential traction is caused by the contraction of epiretinal fibrovascular membranes with puckering of the retina and distortion of retinal blood vessels. B) Anteroposterior traction is caused by the contraction of fibrovascular membranes extending from the retina posteriorly, usually in association with the major arcades, to the vitreous base anteriorly. C) Bridging (trampoline) traction is the result of contraction of fibrovascular membranes which stretch from one part of the posterior retina to another or between the vascular arcades, tending to pull the two involved points together.
- 34. Tractional RD associated with Antero-posterior and bridging traction
- 35. Symptoms: Photopsia and floaters are usually absent because vitreoretinal traction develops insidiously and is not associated with acute PVD. The visual field defect usually progresses slowly and may become stationary for months or even years.
- 36. Signs : o The RD has a concave configuration and breaks are absent. o Retinal mobility is severely reduced and shifting fluid is absent. o The SRF is shallower than in a rhegmatogenous RD and seldom extends to the ora serrata. o The highest elevation of the retina occurs at sites of vitreoretinal traction. o If a tractional RD develops a break it assumes the characteristics of a rhegmatogenous RD and progresses more quickly (combined tractional-rhegmatogenous RD).
- 37. (A) Tractional RD in severe proliferative diabetic retinopathy (B) B-scan- Incomplete posterior vitreous detachment and a shallow tractional RD
- 38. B-scan ultrasonography shows incomplete posterior vitreous detachment and a relatively immobile retina.
Notes de l'éditeur
- Dialyses- circumferential tear along ora serrata
- PVD- seperation of cortical vit, along wid delineating post hyaloid memb,from NSR towards vit base. Latt- discontinuity of ILM wid atrophy of underlying NSR and liq.vitreous Snail- precursor to lattice WWP- strong adhesion of vit gel to retina Myop- holes+