The detection of hrHPV-infection of the cervix using first-void urine in women with an abnormal pap-smear
•
1 j'aime•797 vues
This study aimed to determine the sensitivity and specificity of morning first-void urine (U1) compared to afternoon first-void urine (U2) for HPV detection, and to compare HPV detection in self-collected urine samples to physician-taken cervical smears (PTS). 84 women collected U1 and U2 samples and underwent PTS and cervical biopsies. HPV detection results were identical for 75.6% of U1 and U2 samples, and compatible for 20.7%. Sensitivity for detecting CIN2+ lesions was 100% for U1, U2, and PTS, while specificity was 39-42%. No advantage was found for U1 over U2, and HPV detection in urine seemed
Signaler
Partager
Signaler
Partager
Recommandé
Recommandé
WHAT MICROBIOLOGISTS AND CLINICIANS SHOULD KNOW ABOUT CULTURING WOUND SWABS
Dr.T.V.Rao MD What microbiologists and clinicians should know about culturing wound swabs

What microbiologists and clinicians should know about culturing wound swabsSociety for Microbiology and Infection care
Made by: María Angélica Arango Posada
Molecular Biology
UPBDevelopment of novel visual detection methodology for Salmonella in meat usin...

Development of novel visual detection methodology for Salmonella in meat usin...MariaAngelicaArangoP
Contenu connexe
Tendances
WHAT MICROBIOLOGISTS AND CLINICIANS SHOULD KNOW ABOUT CULTURING WOUND SWABS
Dr.T.V.Rao MD What microbiologists and clinicians should know about culturing wound swabs

What microbiologists and clinicians should know about culturing wound swabsSociety for Microbiology and Infection care
Made by: María Angélica Arango Posada
Molecular Biology
UPBDevelopment of novel visual detection methodology for Salmonella in meat usin...

Development of novel visual detection methodology for Salmonella in meat usin...MariaAngelicaArangoP
Tendances (19)
Whole Genome Sequencing (WGS) for surveillance of foodborne infections in Den...

Whole Genome Sequencing (WGS) for surveillance of foodborne infections in Den...
What microbiologists and clinicians should know about culturing wound swabs

What microbiologists and clinicians should know about culturing wound swabs
Development of novel visual detection methodology for Salmonella in meat usin...

Development of novel visual detection methodology for Salmonella in meat usin...
Journal of Laboratory Automation-2016-Cain-Hom-37-48

Journal of Laboratory Automation-2016-Cain-Hom-37-48
Avian influenza virus surveillance in live bird markets, northern Vietnam

Avian influenza virus surveillance in live bird markets, northern Vietnam
Comparison of tzanck smear with viral serology in varicella

Comparison of tzanck smear with viral serology in varicella
Whole Genome Sequencing (WGS) for surveillance of foodborne infections in Den...

Whole Genome Sequencing (WGS) for surveillance of foodborne infections in Den...
Similaire à The detection of hrHPV-infection of the cervix using first-void urine in women with an abnormal pap-smear
ANALYTICAL AND QUANTITATIVE CYTOPATHOLOGY AND HISTOPATHOLOGYIs the Paris System Sufficient for Reporting Urinary Cytology?

Is the Paris System Sufficient for Reporting Urinary Cytology?ANALYTICAL AND QUANTITATIVE CYTOPATHOLOGY AND HISTOPATHOLOGY
Similaire à The detection of hrHPV-infection of the cervix using first-void urine in women with an abnormal pap-smear (20)
20160918 - F. Prefumo - Ecografia, screening biochimico, NIPT e diagnosi pren...

20160918 - F. Prefumo - Ecografia, screening biochimico, NIPT e diagnosi pren...
Comparative Study of Visual, Clinical and Microbiological Diagnosis of White ...

Comparative Study of Visual, Clinical and Microbiological Diagnosis of White ...
“Integrated Approach: Utilizing Biomarkers, Non-Invasive Prenatal Screening (...

“Integrated Approach: Utilizing Biomarkers, Non-Invasive Prenatal Screening (...
Molecular Detection of Chlamydia Trachomatis and Neisseria Gonorrhea Prevalen...

Molecular Detection of Chlamydia Trachomatis and Neisseria Gonorrhea Prevalen...
Reliability, accuracy and cost effectiveness of prenatal screening

Reliability, accuracy and cost effectiveness of prenatal screening
Interim Guidelines in the Management and Prevention of Ebola Virus Disease as...

Interim Guidelines in the Management and Prevention of Ebola Virus Disease as...
Primary High Risk HPV Testing with Cyctology Triage

Primary High Risk HPV Testing with Cyctology Triage
Role of Diagnostic Laparoscopy in Chronic Abdominal Conditions with Uncertain...

Role of Diagnostic Laparoscopy in Chronic Abdominal Conditions with Uncertain...
Is the Paris System Sufficient for Reporting Urinary Cytology?

Is the Paris System Sufficient for Reporting Urinary Cytology?
Plus de Novosanis
Plus de Novosanis (12)
Immunogenicity and Safety of HepatitisB Injection in the Dermis Using VAX-ID

Immunogenicity and Safety of HepatitisB Injection in the Dermis Using VAX-ID
Assessment of acceptability and usability of new delivery prototype device fo...

Assessment of acceptability and usability of new delivery prototype device fo...
HF-Ultrasound to assess skin thickness and accuracy of penetration depth of V...

HF-Ultrasound to assess skin thickness and accuracy of penetration depth of V...
Intradermal drug delivery: human, medical and design factors

Intradermal drug delivery: human, medical and design factors
Shear Stress Test for the Determination of the Optimal Needle Diameter for In...

Shear Stress Test for the Determination of the Optimal Needle Diameter for In...
Evaluation of injection forces of VAX-ID to maximize usability, minimize pain...

Evaluation of injection forces of VAX-ID to maximize usability, minimize pain...
Colli-Pee: a new device to collect first-void urina at home for molecular de...

Colli-Pee: a new device to collect first-void urina at home for molecular de...
Computational Modeling for the Design Optimization of a Positive Air Pressure...

Computational Modeling for the Design Optimization of a Positive Air Pressure...
Microbiological evaluation of Medical grade PP in the development of a midstr...

Microbiological evaluation of Medical grade PP in the development of a midstr...
High Frequency ultrasound to assess skin thickness in healthy adults to deter...

High Frequency ultrasound to assess skin thickness in healthy adults to deter...
Dernier
❤️Chandigarh Escort Service☎️9815457724☎️ Call Girl service in Chandigarh☎️ Chandigarh Call Girls Service ☎️ Call Girls In Chandigarh BEST Call Girls in CHANDIGARH Escort Service provide Cute Nice sweet and Sexy Models in beautiful CHANDIGARH city cash in hand to hand call girl in CHANDIGARH and CHANDIGARH escorts. HOT & SEXY MODELS // COLLEGE GIRLS IN CHANDIGARH AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME ★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE ★ 100% SATISFACTION,UNLIMITED ENJOYMENT. ★ All Meetings are confidential and no information is provided to any one at any cost.
★ EXCLUSIVE Profiles Are Safe and Consensual with Most Limits Respected
★ Service Available In: - HOME & 24x7 :: 3 * 5 *7 *Star Hotel Service .In Call & Out call
Services :
★ A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without a Condom)Chandigarh Call Girls❤️Chandigarh Escort Service☎️9815457724☎️ Call Girl service in Chandigarh☎️ C...

❤️Chandigarh Escort Service☎️9815457724☎️ Call Girl service in Chandigarh☎️ C...Rashmi Entertainment
❤️Amritsar Escort Service☎️98151-129OO☎️ Call Girl service in Amritsar☎️ Amritsar Call Girls Service ☎️ Call Girls In Amritsar BEST Call Girls in Amritsar Escort Service provide Cute Nice sweet and Sexy Models in beautiful Amritsar city cash in hand to hand call girl in Amritsar and Amritsar escorts. HOT & SEXY MODELS // COLLEGE GIRLS IN Amritsar AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME ★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE ★ 100% SATISFACTION,UNLIMITED ENJOYMENT. ★ All Meetings are confidential and no information is provided to any one at any cost.
★ EXCLUSIVE Profiles Are Safe and Consensual with Most Limits Respected
★ Service Available In: - HOME & 24x7 :: 3 * 5 *7 *Star Hotel Service .In Call & Out call
Services :
★ A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without a Condom)Amritsar Call Girls❤️Amritsar Escort Service☎️98151-129OO☎️ Call Girl service in Amritsar☎️ Amri...

❤️Amritsar Escort Service☎️98151-129OO☎️ Call Girl service in Amritsar☎️ Amri...shallyentertainment1
🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludhiana Call Girls Service 🍑👄 Call Girls In Ludhiana Book Now :- 98157-77685
Our agency presents a selection of young, charming call girls available for bookings at Oyo Hotels. Experience high-class escort services at pocket-friendly rates, with our female escorts exuding both beauty and a delightful personality, ready to meet your desires. Whether it's Housewives, College girls, Russian girls, Muslim girls, or any other preference, we offer a diverse range of options to cater to your tastes.
We provide both in-call and out-call services for your convenience. Our in-call location in Delhi ensures cleanliness, hygiene, and 100% safety, while our out-call services offer doorstep delivery for added ease.
We value your time and money, hence we kindly request pic collectors, time-passers, and bargain hunters to refrain from contacting us. l Ludhiana, Majestic Grand Hotel, Ramada by Wyndham Ludhiana City Centre, Park Plaza Ludhiana, Windsor Fountain, G.T Road Ludhiana escort all Ludhiana service Russian available model female girls in Ludhiana VIP Lo price personal Ludhiana off class call girls payment high profile model and female escort 70% Off On Your First Booking Ludhiana Call Girls Service Cash Payment
Welcome to DILPREET Ludhiana Call Girl Service, the Trusted call girl agency around. We Offer 70% Discount On Your First Booking For Ludhiana Call Girls Service Cash Payment is available.🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludh...

🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludh...dilpreetentertainmen
❤️ Call Girls service In Panchkula☎️9815457724☎️ Call Girl service in Panchkula☎️ Panchkula Call Girls Service ☎️ Call Girls In Panchkula BEST CALL GIRL ESCORTS SERVICE IN PANCHKULA CALL WATTSAPP 9815457724 THE MOST BEAUTIFUL INDEPENDENT ESCORT CALL GIRL SERVICE In Panchkula WE ARE PROVIDING GENUINE CALL GIRL SERVICE
I AM A a NATURAL BRUNETTES, SLIM BODY, NATURAL LONG HAIR AND ALL TYPE OF HAIR IS A NATURAL BRUNETTE IN THE MOST BEAUTIFUL MODELS INDEPENDENT ESCORT GIRL I AM A NATURAL BRUNETTE WITH ROOM AND HOTEL AND A NATURAL BRUNETTE WITH A BODY MADE FOR SIN AND ALL TYPE OF ME ALL THE TIME
I SEND YOU A HAIR, VERY SOCIABLE AND FUNNY, READY TO ENTERTAIN TO ENTERTAIN U AND MAKE FORGET ABOUT TO AGET ENTERTAINMENT YOU AND MAKE FORGET ABOUT ALL THE PROBLEMS. LET'S HAVE A WONDERFUL TIME TOGETHER AND FORGET ABOUT EVERYTHING ALL TYPE SERVICE ENJOYMENT SAFE AND SECURE IN CALL OUT CALL HOME AND HOTEL ANYTIME AVAILABLE
AND ALL TYPE SERVICE ENJOYMENTPANCHKULA INDEPENDENT BEST CALL GIRL ESCORTS SERVICE IN PANCHKULA INDEPENDENT CALL GIRLS❤️ Call Girls service In Panchkula☎️9815457724☎️ Call Girl service in Panchku...

❤️ Call Girls service In Panchkula☎️9815457724☎️ Call Girl service in Panchku...Rashmi Entertainment
Dernier (18)
❤️Chandigarh Escort Service☎️9815457724☎️ Call Girl service in Chandigarh☎️ C...

❤️Chandigarh Escort Service☎️9815457724☎️ Call Girl service in Chandigarh☎️ C...
💸Cash Payment No Advance Call Girls Pune 🧿 9332606886 🧿 High Class Call Girl ...

💸Cash Payment No Advance Call Girls Pune 🧿 9332606886 🧿 High Class Call Girl ...
💞 Safe And Secure Call Girls gaya 🧿 9332606886 🧿 High Class Call Girl Service...

💞 Safe And Secure Call Girls gaya 🧿 9332606886 🧿 High Class Call Girl Service...
💞 Safe And Secure Call Girls Mysore 🧿 9332606886 🧿 High Class Call Girl Servi...

💞 Safe And Secure Call Girls Mysore 🧿 9332606886 🧿 High Class Call Girl Servi...
💸Cash Payment No Advance Call Girls Kanpur 🧿 9332606886 🧿 High Class Call Gir...

💸Cash Payment No Advance Call Girls Kanpur 🧿 9332606886 🧿 High Class Call Gir...
💸Cash Payment No Advance Call Girls Hyderabad 🧿 9332606886 🧿 High Class Call ...

💸Cash Payment No Advance Call Girls Hyderabad 🧿 9332606886 🧿 High Class Call ...
💸Cash Payment No Advance Call Girls Surat 🧿 9332606886 🧿 High Class Call Girl...

💸Cash Payment No Advance Call Girls Surat 🧿 9332606886 🧿 High Class Call Girl...
👉Bangalore Call Girl Service👉📞 6378878445 👉📞 Just📲 Call Manisha Call Girls Se...

👉Bangalore Call Girl Service👉📞 6378878445 👉📞 Just📲 Call Manisha Call Girls Se...
💸Cash Payment No Advance Call Girls Nagpur 🧿 9332606886 🧿 High Class Call Gir...

💸Cash Payment No Advance Call Girls Nagpur 🧿 9332606886 🧿 High Class Call Gir...
❤️Amritsar Escort Service☎️98151-129OO☎️ Call Girl service in Amritsar☎️ Amri...

❤️Amritsar Escort Service☎️98151-129OO☎️ Call Girl service in Amritsar☎️ Amri...
🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludh...

🍑👄Ludhiana Escorts Service☎️98157-77685🍑👄 Call Girl service in Ludhiana☎️Ludh...
❤️ Chandigarh Call Girls Service☎️9878799926☎️ Call Girl service in Chandigar...

❤️ Chandigarh Call Girls Service☎️9878799926☎️ Call Girl service in Chandigar...
❤️ Call Girls service In Panchkula☎️9815457724☎️ Call Girl service in Panchku...

❤️ Call Girls service In Panchkula☎️9815457724☎️ Call Girl service in Panchku...
💸Cash Payment No Advance Call Girls Kolkata 🧿 9332606886 🧿 High Class Call Gi...

💸Cash Payment No Advance Call Girls Kolkata 🧿 9332606886 🧿 High Class Call Gi...
💞 Safe And Secure Call Girls Coimbatore 🧿 9332606886 🧿 High Class Call Girl S...

💞 Safe And Secure Call Girls Coimbatore 🧿 9332606886 🧿 High Class Call Girl S...
❤️ Zirakpur Call Girl Service ☎️9878799926☎️ Call Girl service in Zirakpur ☎...

❤️ Zirakpur Call Girl Service ☎️9878799926☎️ Call Girl service in Zirakpur ☎...
The detection of hrHPV-infection of the cervix using first-void urine in women with an abnormal pap-smear
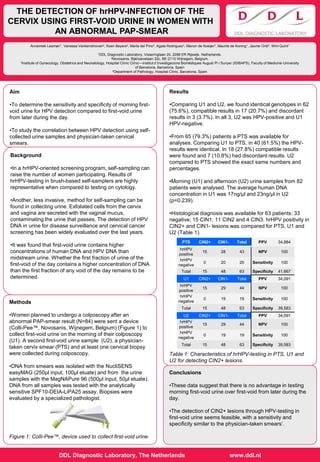
- 1. Background •In a hrHPV-oriented screening program, self-sampling can raise the number of women participating. Results of hrHPV-testing in brush-based self-samplers are highly representative when compared to testing on cytology. •Another, less invasive, method for self-sampling can be found in collecting urine. Exfoliated cells from the cervix and vagina are secreted with the vaginal mucus, contaminating the urine that passes. The detection of HPV DNA in urine for disease surveillance and cervical cancer screening has been widely evaluated over the last years. •It was found that first-void urine contains higher concentrations of human DNA and HPV DNA than midstream urine. Whether the first fraction of urine of the first-void of the day contains a higher concentration of DNA than the first fraction of any void of the day remains to be determined. Aim •To determine the sensitivity and specificity of morning first- void urine for HPV detection compared to first-void urine from later during the day. •To study the correlation between HPV detection using self- collected urine samples and physician-taken cervical smears. Results •Comparing U1 and U2, we found identical genotypes in 62 (75.6%), compatible results in 17 (20.7%) and discordant results in 3 (3.7%). In all 3, U2 was HPV-positive and U1 HPV-negative. •From 65 (79.3%) patients a PTS was available for analyses. Comparing U1 to PTS, in 40 (61.5%) the HPV- results were identical. In 18 (27.8%) compatible results were found and 7 (10.8%) had discordant results. U2 compared to PTS showed the exact same numbers and percentages. •Morning (U1) and afternoon (U2) urine samples from 82 patients were analysed. The average human DNA concentration in U1 was 17ng/µl and 23ng/µl in U2 (p=0.239). •Histological diagnosis was available for 63 patients: 33 negative; 15 CIN1; 11 CIN2 and 4 CIN3. hrHPV positivity in CIN2+ and CIN1- lesions was compared for PTS, U1 and U2 (Table 1). Table 1: Characteristics of hrHPV-testing in PTS, U1 and U2 for detecting CIN2+ lesions. Methods •Women planned to undergo a colposcopy after an abnormal PAP-smear result (N=84) were sent a device (Colli-Pee™, Novosanis, Wijnegem, Belgium) (Figure 1) to collect first-void urine on the morning of their colposcopy (U1). A second first-void urine sample (U2), a physician- taken cervix smear (PTS) and at least one cervical biopsy were collected during colposcopy. •DNA from smears was isolated with the NucliSENS easyMAG (250µl input, 100µl eluate) and from the urine samples with the MagNAPure 96 (500µl input, 50µl eluate). DNA from all samples was tested with the analytically sensitive SPF10-DEIA-LiPA25 assay. Biopsies were evaluated by a specialized pathologist. Figure 1: Colli-Pee™, device used to collect first-void urine. THE DETECTION OF hrHPV-INFECTION OF THE CERVIX USING FIRST-VOID URINE IN WOMEN WITH AN ABNORMAL PAP-SMEAR Annemiek Leeman1, Vanessa Vankerckhoven2, Koen Beyers2, Marta del Pino3, Agata Rodriguez3, Manon de Koeijer2, Maurits de Koning1, Jaume Ordi4, Wim Quint1 1DDL Diagnostic Laboratory, Visseringlaan 25, 2288 ER Rijswijk, Netherlands. 2Novosanis, Bijkhoevelaan 32c, BE-2110 Wijnegem, Belgium. 3Institute of Gynecology, Obstetrics and Neonatology, Hospital Clínic Clínic—Institut d´Investigacions Biomèdiques August Pi I Sunyer (IDIBAPS), Faculty of Medicine-University of Barcelona, Barcelona, Spain 4Department of Pathology, Hospital Clínic, Barcelona, Spain DDL Diagnostic Laboratory, The Netherlands www.ddl.nl Conclusions •These data suggest that there is no advantage in testing morning first-void urine over first-void from later during the day. •The detection of CIN2+ lesions through HPV-testing in first-void urine seems feasible, with a sensitivity and specificity similar to the physician-taken smears’. PTS CIN2+ CIN1- Total PPV 34,884 hrHPV positive 15 28 43 NPV 100 hrHPV negative 0 20 20 Sensitivity 100 Total 15 48 63 Specificity 41,667 U1 CIN2+ CIN1- Total PPV 34,091 hrHPV positive 15 29 44 NPV 100 hrHPV negative 0 19 19 Sensitivity 100 Total 15 48 63 Specificity 39,583 U2 CIN2+ CIN1- Total PPV 34,091 hrHPV positive 15 29 44 NPV 100 hrHPV negative 0 19 19 Sensitivity 100 Total 15 48 63 Specificity 39,583
