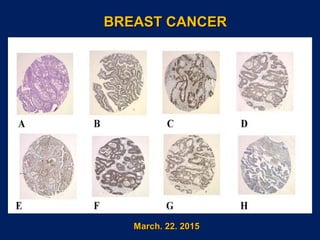
Breast carcinoma march 22. 2015
- 1. BREAST CANCERBREAST CANCER March. 22. 2015March. 22. 2015
- 3. Breast Carcinoma Statistics • One in eight women will get breast cancer, • one third of women with breast cancer will die of the disease.
- 4. Risk Factors for Breast Cancer Estrogen, Long & Strong exposure. (F/M ratio = 100/1) • Geography • Family historty; (1st degree, early age, bilat)/ 2 folds • Age (Peak; 60 – 70y) • Menstrual history & Reproductive history. - (Early menarch & late Menopause) - Pregnancy - (Nilliparous, Late 1st pregnancy) - (1st delivery at 18 y, / 1st delivery at 30 y) - Lactation, decrease risk - Oophorectomy (decrease the risk to 1/3) • Benign breast disease (Hx of previous breast pathology) - Fibrocystic disease +/- epith hyperplasia +/- atypia. - CIS - 0X, 2X, 5X, 10X
- 5. Risk Factors for Breast Cancer • Estrogen (exogenous), increase risk to 2.5 folds In 2002 Estrogen declared as carcinogen by National Toxicology Program. • Oral contraceptive • Radiation Exposure • Carcinoma of the contralateral breast or endometrium • Obesity • High fat diet • Alcohol • Smoking • Environmental Toxins • Breast augmentation. • ABORTIONS?
- 6. Causes of Breast Cancer • Genetic • Environmental • Hormonal
- 7. Breast Cancer Pathology Ductal Ca. (85 – 93%) Lobular Ca. (7 – 15%) In Situ Carcinomas (CIS) (15 ) Invasive Carcinomas (85%) Special Subtypes (> 5%)
- 8. Ductal Carcinoma in Situ • Clinical: – DCIS usually does not present as a palpable mass, if it does it is usually high grade and a large lesion • Mammogram: – The most common method of detection is by identifying calcifications • MRI • FNA • Biopsy
- 9. Mammography showing a normal breast (left) and a cancerous breast (right).
- 10. Stellate lesion Calcifications Mammogrm: -Calcification - fibrous parenchyma Mammogrm: -1% false positive -20% false negative -Calcification, positive -50 - 60% in ca. -20% in benign
- 11. DCIS is confined to within the ductal system
- 14. Architectural Patterns of DCIS • Comedo (high grade) – Grade 3 nuclei and necrosis – Often has associated microcalcifications • Solid (Low grade) – Carcinoma fills and distends the ducts • Micropapillary (Low grade) – Papillary structures that extend into the lumen of the duct • Cribriform (Low grade) – Forms a rigid “cartwheel” pattern
- 15. The adult, resting Breast connective tissue adipose well developed ducts connective tissue scanty secretory units
- 20. Pathobiologic Events Associated with DCIS
- 21. DCIS: actin Stain of Myoepithelium
- 22. Natural History • 5 Year survival = 100% < 50 or > 50 year • If untreated ; – 28% developed invasive cancer – 10 fold increase in RR to controls
- 23. Axillary lymph nodes • Axillary LN involvement is <1% • Axillary LN dissection is not recommended • Sentinel lymph node biopsy? – Not recommended. – Consider: extensive high grade DCIS or palpable mass (increased chance of invasive disease being found)
- 24. • Mammography is the standard for detection of DCIS. • MRI could help especially in high-grade DCIS
- 25. Burstein H et al. N Engl J Med 2004;350:1430-1441 The Risk of Ipsilateral or Contralateral Breast Tumor for Patients with DCIS Treated with Excision Alone; Excision and Radiotherapy; Excision, Radiotherapy, and Tamoxifen; or Excision, Radiotherapy, and Placebo
- 26. Lobular Carcinoma in Situ (LCIS) • Multicentric , Bilateral • Proliferation of neoplastic population of cells within the TDLU • may extend into adjacent ducts.
- 28. Invasive (Infiltrating) Breast Carcinoma Main histological types; • Invasive ductal ca.(85%) • Invasive lobular ca. (7 – 15%) • Medullary ca. (2%) • Mucoid ca. (2%) • Tubular ca. (2%)
- 29. Invasive (Infiltrating) ductal carcinoma • The most common (> 85%). – Mass – +/- skin dimpling, nipple retraction • Mammogram; • MRI • FNA. • Biopsy Correlate with breast parenchyma at each quadrant
- 31. Stellate lesion Calcifications Mammogrm: -Calcification - fibrous parenchyma Mammogrm: -1% false positive -20% false negative -Calcification, positive -50 - 60% in ca. -20% in benign
- 32. Infiltrating Ductal Ca. • Gross: – Firm, gritty, stellate • Micro: – Grading depends on: 1) degree of tubule formation 2) nuclear grade 3) mitotic rate – Fibrosis (desmoplasia) – +/- calcifications
- 33. Infiltrating Lobular Carcinoma • 2nd most common invasive breast cancer. • +/- mass • L/M; - linear profiles of malignant cells “INDIAN” FILE - low nuclear grade, - minimal mitosis. - Dense fibrosis • multifocal & bilateral • Same prognosis as IDC, if matched for stage • ER+/ PR + • HER2 Neg.
- 35. Uncommon types of Invasive Carcinoma of the Breast • Mucinous (Colloid) Ca. – Older women – Malignant cells floating in pools of mucin – Better prognosis than invasive ductal or lobular • Tubular Carcinoma – Younger women – Excellent prognosis • Medullary carcinoma. – lots of lymphocytes) – Is better in behavior
- 36. Inflammatory Carcinoma • Invasive carcinoma involving superficial dermal lymphatic spaces • Poor prognosis • so called “inflammatory changes” - Erythema and induration of the skin, – Peau d’orange- of involved skin caused by lymphatic involvement and obstruction
- 37. Inflammatory carcinoma: dermal lymphatic spaces containing tumor cells
- 38. Paget’s Disease • Invasion of the SKIN of the nipple or areola by malignant cells. • Associated with an underlying cancer: either IN SITU OR INVASIVE carcinoma • Clinically-erythema, scaling, ulceration
- 39. Paget’s Disease of the Nipple Intra-epidermal adenocarcinoma cells
- 41. Tumor grade HISTOLOGY • WHO grading Well diff. Mod. diff. Poor diff. • B-R grading Glands Nuclei Mitosis CYTOLOGY – Nuclei • Size • Chromatin • Nucleoli Nuclear grade 1-3 Good correlation with histologic grade
- 42. BREAST CANCER TNM stage groupingTNM stage grouping Stage 0Stage 0 Tis N0 M0 Stage IStage I T1* N0 M0 Stage IIAStage IIA T0 N1 M0 T1* N1** M0 T2 N0 M0 Stage IIBStage IIB T2 N1 M0 T3 N0 M0 Stage IIIAStage IIIA T0, T1,* T2 N2 M0 T3 N1, N2 M0 Stage IIIBStage IIIB T4 Any N M0 Any T N3 M0 Stage IVStage IV Any T Any N M1 * Note: T1 includes T1 mic. ** Note: The prognosis of patients with N1a is similar to that of patients with pN0. AJCC® Cancer Staging Manual, 5th edition (1997) published by Lippincott-Raven Publishers, Philadelphia, Pennsylvania.
- 43. BREAST CANCER Tumor definitionsTumor definitions • TX Primary tumor cannot be assessed • T0 No evidence of primary tumor • Tis Carcinoma in situ: Intraductal carcinoma, lobular carcinoma in situ, or Paget’s disease of the nipple with no tumor • T1 Tumor 2 cm or less in its greatest diameter T1mic Microinvasion more than 0.1 cm or less in its greatest diameter T1a Tumor more than 0.1 cm but not more than 0.5 cm in its greatest diameter T1b Tumor more than 0.5 cm but not more than 1 cm in its greatest diameter T1c Tumor more than 1 cm but not more than 2 cm in its greatest diameter • T2 Tumor more than 2 cm but not more than 5 cm in its greatest diameter • T3 Tumor more than 5 cm in its greatest diameter • T4 Tumor of any size with direct extension to (a) chest wall or (b) skin, only as described below T4a Extension to chest wall T4b Edema (including peau d’orange) or ulceration of the skin of the breast or satellite skin nodules confined to the same breast T4c Both (T4a and T4b) T4d Inflammatory carcinoma AJCC® Cancer Staging Manual, 5th edition (1997) published by Lippincott-Raven Publishers, Philadelphia, Pennsylvania.
- 44. BREAST CANCER Commonly assessed prognosticCommonly assessed prognostic factorsfactors Slamon DJ. Chemotherapy Foundation. 1999;46. Winer E, et al. Cancer: Principles & Practice of Oncology. 6th ed. 2001;1651-1717. Nuclear grade Estrogen/progesterone receptors HER2/neu overexpression Number of positive axillary nodes Tumor size Lymphatic and vascular invasion Histologic tumor type Histologic grade
- 45. BREAST CANCER 5-year survival as function of the number5-year survival as function of the number of positive axillary lymph nodesof positive axillary lymph nodes 0% 20% 40% 60% 80% 5-YearSurvival5-YearSurvival 0 1 2 3 4 5 6-10 11-15 16-20 >20 Number of Positive NodesNumber of Positive Nodes Harris J, et al. Cancer: Principles & Practice of Oncology. 5th ed. 1997;1557-1616.
- 46. Histopathologic Grade If B-R score is 3, 4, 5 = low grade If B-R score is 6, 7 = Intermediate grade If B-R score is 8, 9 = High grade
- 47. Total Cancers Per Cent In Situ Carcinoma 15–30 Ductal carcinoma in situ, DCIS 80 Lobular carcinoma in situ, LCIS 20 Invasive Carcinoma 70–85 No special type ductal carcinoma (“NOS") 79 Lobular carcinoma 10 Tubular/cribriform carcinoma (Better prognosis than average) < 5 Mucinous (colloid) carcinoma (Better prognosis than average) 2 Medullary carcinoma (Better prognosis than average) 2 Papillary carcinoma (Better prognosis than average) 1 Metaplastic carcinoma, (Squamous)
- 48. The “Triple Test”: (Screening) – Clinical picture – Mammographic findings – Cytologic findings Biopsy. (diagnosis)
- 49. MALE BREAST • GYNECOMASTIA (related to hyperestrogenism) • CARCINOMA (1% of ♀ )
- 50. Gynecomastia • Reversible enlargement of the male breast • Unilateral or bilateral subareolar mass +/-pain • Ductal and stromal proliferation • Etiology- Systemic disease-hyperthyroidism, cirrhosis, chronic renal failure – Drugs-cimetidine, digitalis, tricyclic antidepressants, marijuana – Neoplasms-pulmonary, testicular germ cell tumors – Hypogonadism: testicular atrophy, exogenous estrogen, Klinefelter’s syndrome
- 54. Adenocarcinoma
- 55. Carcinoma of the Male Breast • < 1% of breast cancer • Very rare occurrence; F/M = 100:1 • Infiltrating ductal carcinoma. • Tends to present at a more advanced stage – Less fat and breast tissue, therefore involvement of chest wall occurs earlier • Similar prognosis when matched, stage for stage, with female breast cancer • Associated with inherited BRCA2 mutation
- 57. Multistage Model of Carcinogenesis Normal Atypical Hyperplasia Carcinoma In Situ Invasive Carcinoma Metastasis
- 58. QUIZ 1. List the benign breast diseases that increase a patient’s risk of developing breast cancer and classify these conditions by the degree of risk.
Notes de l'éditeur
- Microcalcifications, seen on mammograms, are often the result of necrotic intraductal crud which has calcified. Lets make this quite simple: NECROSIS in a hyperplastic duct is usually DCIS
- Figure 1. Pathobiologic Events Associated with Ductal Carcinoma in Situ. The molecular, cellular, and pathological processes that occur in the transformation from healthy tissue to preinvasive lesions, such as ductal carcinoma in situ, to breast cancer are shown. The majority of the changes that give rise to cancer, including the accumulation of genetic changes, oncogene expression, and the loss of normal cell-cycle regulation, appear to have occurred by the time ductal carcinoma in situ is present. Most of the clinical features of a subsequent invasive breast cancer are already determined at this stage, although additional events, including tissue invasion and changes in the surrounding stroma, characterize the invasive tumor.
- Figure 3. The Risk of Ipsilateral or Contralateral Breast Tumor after Surgical Excision among Patients with Ductal Carcinoma in Situ Who Were Treated with Excision Alone; Excision and Radiotherapy; Excision, Radiotherapy, and Tamoxifen; or Excision, Radiotherapy, and Placebo. The overall risk, the risk of invasive cancer, and the risk of noninvasive cancer are shown. Data are from combined analyses of the National Surgical Adjuvant Breast and Bowel Project B-17 and B-24 trials.
- A whole lobule filled with monotono0us cells of the same type can be called LCIS, or lobular carcinoma in situ. Note the COMPLETE LACK of atypia and necrosis, but it’s still CA-in-situ because this is a LOBULE!
- The tumor cells are INSIDE the skin dermal lymphatic spaces.
- Breast Cancer: TNM Stage Grouping The current breast cancer staging system is the 5th edition of the American Joint Committee on Cancer (AJCC) system, sponsored jointly by the American Cancer Society, the National Cancer Institute, the College of American Pathologists, and the American Colleges of Physicians, Radiology, and Surgeons. The AJCC system is a clinical and pathologic staging system based on the TNM system. T refers to tumor, N to nodes, and M to metastasis.
- Tumor definitions This slide further delineates the breakdown in staging of the primary tumor.
- Breast Cancer: Commonly Assessed Prognostic Factors A prognostic factor is defined as a biologic or clinical measurement associated with disease-free or overall survival in the absence of adjuvant systemic therapy. The most useful prognostic factor is the number of positive axillary lymph nodes based on a level I/II (or higher) axillary dissection and detailed histologic evaluation. Tumor size correlates with the number of involved nodes, but has independent prognostic significance.
- Breast Cancer: 5-year Survival as Function of the Number of Positive Axillary Lymph Nodes As the number of involved lymph nodes increases, 5-year survival rates decrease.
- Note that no matter how big a male’s breasts may get, they should never for m lobules, but just end as blunt ducts.
