AORTIC ANEURYSM.pptx
- 1. AORTIC ANEURYSM DR MOHAMMED SHANIL.P JUNIOR RESIDENT, GENERAL MEDICINE
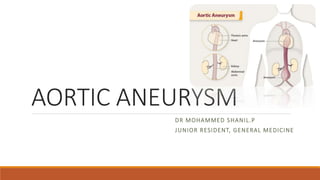
- 2. What is the anatomy of the aorta? The aorta has many sections, including the: •Aortic root: Section that attaches to the heart. This is the widest part of the aorta. •Aortic valve: Three flaps of tissue (leaflets) that snap open and shut to release oxygen-rich blood from the heart. •Ascending aorta: Upward curve that occurs shortly after the aorta leaves the heart. •Aortic arch: Curved segment that gives the aorta its cane-like shape. It bridges the ascending and descending aorta. •Descending aorta: Long, straight segment that runs from your chest (thoracic aorta) to your abdominal area (abdominal aorta).
- 3. AORTIC ANEURYSM •It is a localized dilatation of the aorta having a diameter at least 1.5 times that of the expected normal diameter of that given aortic segment •True aneurysm involves all the three layers of the aortic wall. It is produced by the progressive distension of the aortic wall that is weakened by the degeneration of the tunica media
- 4. •Morphologically two types: • Fusiform aneurysm (more common)- symmetrical dilatation of the full circumference of the aortic wall • Saccular aneurysm- involves localized dilation appearing as an out-pouching of only a portion of the aortic wall •False or pseudoaneurysm- well defined collection of blood and connective tissue outside the vessel wall due to contained rupture of the aortic wall
- 6. DISEASES ASSOCIATED WITH AA
- 7. ABDOMINAL AORTIC ANEURYSM •More common than thoracic aneurysm •Male > Female ETIOPATHOGENESIS •Usually atherosclerotic •Rarely traumatic, congenital or myxomatous •Most are infrarenal and fusiform •Absence of vasa vasorum in the infrarenal aorta coupled with atherosclerotic thickening of intima may jeopardise nutrient and oxygen supply to the media of this segment •In genetically predisposed subjects due to increased elastolytic activity and lead to aneurysm formartion •DM patients are not prone to development of abdominal aortic aneurysm
- 8. CRAWFORD CLASSIFICATION OF TAAA ReplyForward Type I arises from above the sixth intercostal space, usually near the left subclavian artery, and extends to include the origins of the celiac axis and superior mesenteric arteries. Although the renal arteries can also be involved, the aneurysm does not extend into the infrarenal aortic segment. Type II aneurysm also arises above the sixth intercostal space and may include the ascending aorta, but extends distal to include the infrarenal aortic segment, often to the level of the aortic bifurcation.
- 9. Type III aneurysm arises in the distal half of the descending thoracic aorta, below the sixth intercostal space, and extends into the abdominal aorta. Type IV aneurysm generally involves the entire abdominal aorta from the level of the diaphragm to the aortic bifurcation. Type V aneurysm arises in the distal half of the descending thoracic aorta, below the sixth intercostal space, and extends into the abdominal aorta, but is limited to the visceral segment
- 10. CLINICAL FEATURES Symptoms: •Backache •Abdominal pain •Limb edema •Venous congestion •Most common complaint is a steady, gnawing pain in the hypogastrium or lower back for hours/ days and not affected by movement
- 11. CLINICAL FEATURES (cont..) Signs: •Palpable pulsatile mass in the abdomen (from xiphoid process to the umbilicus) • Tender on palpation •Presence of peripheral vascular disease •Signs of distal embolism •Hemodynamic collapse •Absence of femoral and lower limb pulses and bruits over affected arteries •Rarely, lower limb edema, venous congestion •Haematomas in the flanks and groin • Rupture into the left retroperitoneum, peritoneal cavity, duodenum producing hemorrhage and abdominal distension • Rarely rupture into the IVC, iliac or renal vein producing collapse and cardiac failure
- 12. DIAGNOSIS AND SIZE ESTIMATION •Physical examination •Routine roentgenography •Abdominal cross sectional ultrasonography •Digital subtraction angiography •Abdominal aortic angiography •CT scan- extremely accurate for diagnosis and size estimation •MRI •Xray- paravertebral soft tissue mass. With rupture, there is distortion of the psoas muscle shadow and absence of gas in the bowel over the aneurysm
- 13. DIAGNOSIS AND SIZE ESTIMATION (cont..) As per ESC guidelnes on diagnosis and treatment of aortic disease, following are the recommendations for abdominal aortic aneurysm (AAA) screening: •All males > 65years of age •Maybe considered in females> 65 years of age with history of current/ past smoking
- 14. TREATMENT •Beta blockers •Aneurysmectomy & replacement by a synthetic prosthesis usually Dacron •Complications of AAA repair • Death • Ischaemia (mainly cardiac, lower limb, colonic & spinal cord) • Pneumonia • Renal insufficiency • Stroke • Wound infection • Graft infection • Thrombosis •Endovascular AAA repair
- 15. TREATMENT (cont..) As per ESC guidelnes on diagnosis and treatment of aortic diseases, recommendations for management of asymptomatic patients with enlarged aorta or AAA are: •AAA with diameter 25 - 29mm, ultrasound imaging should be considered 4 years later •AAA with diameter 30 – 39mm, ultrasound imaging every 3 years, 40 – 44mm every 2 years and >45mm, every year is recommended •AAA repair is indicated if : • AAA diameter> 55mm (IB) • Aneurysm growth> 10mm/year (IB) •Large aneurysm- aortic repair is recommended •In symptomatic & suspended rupture- urgent repair is indicated
- 16. THORACIC AORTIC ANEURYSM •Divided anatomically: • Ascending arch aneurysm • Descending aortic aneurysm •Ascending aorta aneurysms results from: • cystic medial necrosis • Marfan’s syndrome • Syphilis • Atherosclerosis
- 17. CLINICAL MANIFESTATIONS •Vascular consequences: • Aortic regurgitation • Secondary congestive heart failure due to aortic root dilatation • Myocardial ischaemia due to coronary artery compression by enlarged sinuses of Valsalva • Rupture of sinus of Valsalva into the right heart producing continuous murmur with CCF • Thromboembolism causing stroke • Lower extremity ischaemia • Renal infarction • Mesenteric ischaemia • Superior vena cava syndrome: trachea, main stem bronchus compression, oesophageal compression causing dysphagia, hoarseness
- 18. DIAGNOSIS •Transthoracic Echocardiography •Transoesophageal Echocardiography •Contrast CT scan •MR Angiography
- 19. TREATMENT •Beta blockers to reduce size in smaller aneurysms •Aneurysmectomy and replacement by a prosthetic sleeve or composite graft valve in aneurysms 6cm or larger •Early surgery indicated in Marfan’s syndrome, bicuspid aortic valve or rapidly growing aneurysms •Transluminally placed endovascular stent grafts
- 20. TREATMENT (cont..) As per 2014 ESC guidelnes on diagnosis and treatment of aortic disease, following are the recommendations for interventions on thoracic aortic aneurysm •For ascending aorta aneurysms, surgery should be considered for: • AAA >/=50mm for patients with Marfan’s syndrome with risk factors 50mm for patients with bicuspid valve with risk factors • 55mm for other patients with no elastopathy •Interventions on Aortic arch aneurysm: • Surgery should be considered in patients who have isolated AAA with maximal diameter >/= 55mm
- 21. •Interventions on Descending arch aneurysm: • TEVAR in patients with maximal diameter>/= 55mm • In case of Marfan’s syndrome and other elastopathies, surgeries should be indicated rather than TEVAR
