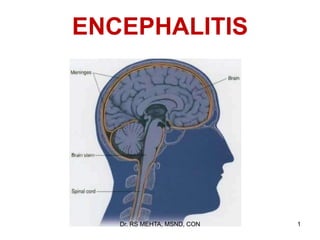
Understanding Encephalitis
- 1. ENCEPHALITIS Dr. RS MEHTA, MSND, CON 1
- 2. Encephalitis: Infectious process & inflammatory response limited to brain parenchyma. Meningoencephalitis: Meninges + brain Encephalomyelitis: Brain + spinal cord Encephalomyeloradicilitis: brain + spinal cord + nerve root Dr. RS MEHTA, MSND, CON 2
- 3. J. ENCEPHALITIS Flavivirus Dr. RS MEHTA, MSND, CON 3
- 4. Year JE Cases Death 1993 446 108 1994 1836 283 1995 1246 255 1996 1450 260 1997 2953 407 Dr. RS MEHTA, MSND, CON 4
- 5. No.of cases Average month wise distribution of subjects(1993-20000 700 600 500 400 300 200 100 0 650 25 May 100 75 July 25 Sept. Oct. Nov Months Dr. RS MEHTA, MSND, CON 5
- 6. ENCEPHALITIS • Encephalitis is the inflammation of the brain parenchyma, presents as diffuse and/ or focal neuropsychological dysfunction. • From an epidemiologic and pathophysiologic perspective, encephalitis is distinct from menningitis though on clinical evaluation the two often coexist with the sign and symptoms of meningeal inflammation such as photophobia, headache or a stiff neck. Dr. RS MEHTA, MSND, CON 6
- 7. • Viral infection is the most common and important cause, with over 100 viruses implicated worldwide Dr. RS MEHTA, MSND, CON 7
- 8. PATHOPHYSIOLOGY Portal of Entry Mosquito Transmit virus to the body Hematogeneous Spread or neural and olfactory pathways. Crosses BBB Enters neural cells Disruption in cell functioning Perivascular congestion Haemorrhage Inflammatory response Dr. RS MEHTA, MSND, CON 8
- 9. • In acute encephalitis, cerebral edema and petechial hemorrhages occur throughout the hemispheres, brain stem, cerebellum, and, occasionally, spinal cord. • Direct viral invasion of the brain usually damages neurons, sometimes producing visible inclusion bodies. • Severe infection, particularly untreated encephalitis, can cause brain hemorrhagic necrosis. Dr. RS MEHTA, MSND, CON 9
- 10. Sign and Symptoms Initial Signs • • • • • Headache Malaise Anorexia Nausea and Vomiting Abdominal pain Dr. RS MEHTA, MSND, CON 10
- 11. • Symptoms – Fever – Headache – Behavioral changes – Altered level of consciousness – Focal neurologic deficits – Seizures Dr. RS MEHTA, MSND, CON 11
- 12. Developing Signs • Altered LOC – mild lethargy to deep coma. • Altered Mental State – confused, delirious, disoriented. • Mental Disorders: – – – – – hallucinations agitation personality change behavioral disorders occasionally frank psychosis • Focal or general seizures in >50% severe cases. • Severe focused neurologic deficits. Dr. RS MEHTA, MSND, CON 12
- 13. • The classic presentation is encephalopathy with diffuse or focal neurologic symptoms, including the following: –Behavioral and personality changes, decreased level of consciousness –Stiff neck, photophobia, and lethargy –Generalized or localized seizures –Acute confusion or amnestic states –Flaccid paralysis (10%) Dr. RS MEHTA, MSND, CON 13
- 14. Dr. RS MEHTA, MSND, CON 14
- 15. Dr. RS MEHTA, MSND, CON 15
- 16. Neurologic Signs • Virtually every possible focal neurological disturbance has been reported. • Most Common – Aphasia – Ataxia – Hemiparesis with hyperactive tendon reflexes – Involuntary movements – Cranial nerve deficits (ocular palsies, facial weakness) Dr. RS MEHTA, MSND, CON 16
- 17. Summary C/F • • • • • • • • • • Acute febrile illness : Meningitis + Encephalitis Confusion, behavioural changes Altered LOC: lethargy & coma Focal / Diffuse neurological S/S Frank psychotic status Focal/Generalized seizures Focal findings: aphasia, ataxia, hemiparesis Increase DTR, Increase planter Involumentry movement, tremor, myoclonic jerk Ocular palsy/facial weaknes Dr. RS MEHTA, MSND, CON 17
- 18. Differential diagnosis • • • • • • • • Brain absess Subarachnoid hemorrhage SLE Toxoplasmosis Hypoglycemia Meningitis Status epilepticus Tuberculosis Dr. RS MEHTA, MSND, CON 18
- 19. Lab findings: Summary • • • • • • CSF: LP all suspected cases DLC: Lymphocyte Protein: Mildly elevated Sugar: Normal (> 45 mg/dl) in viral RBC in CSF: 20%, RBC > 500 /L MRI/CT: Mass lesion / basal meningitis / hydrocephalus • Brain biopsy: previously gold standard – now CSF • CSF PCR has become the primary diagnostic test for CNS infections caused by CMV, EBV, VZV, Dr. RS MEHTA, MSND, 19 HHV-6, and enteroviruses. CON
- 20. CSF Parameters CONDITION CELL TYPE CELL COUNT NORMAL LYMPHOCYTES 0-4*108 /L VIRAL LYMPHOCYTES 10-2000 BACTERIAL POLYMORPHS TUBERCULO P+L MIXED US GLUCOSE PROTEIN GRAM STAIN >60% of Blood glucose Upto 0.45g/l (-) Normal Normal (-) 10005000 Low Normal/ elevated + 50-5000 Low Elevated Often (-) FUNGAL LYMPHOCYTES 50-500 Low Elevated (+/-) MALIGNANT LYMPHOCYTES 0-100 Low Normal/ elevated (-) Dr. RS MEHTA, MSND, CON 20
- 21. TREATMENT 1. EMERGENCY MANAGEMENT • Evaluate and treat for shock or hypotension. Administer a crystalloid infusion until the patient is euvolemic. • Consider airway protection in patients with an altered mental status. • Consider seizure precautions. Treat seizures according to usual protocol (ie, lorazepam 0.1 mg/kg given intravenously [IV]). • Stabilize alert patients with normal vital signs by administering oxygen, securing IV access, and providing rapid transport to the ED. Dr. RS MEHTA, MSND, CON 21
- 22. Medication Antivirals • The goal of the use of antivirals to shorten the clinical course, prevent complications, prevent the development of latency and/or subsequent recurrences, decrease transmission, and eliminate established latency 1. Acyclovir (Zovirax) Adult • 10 mg/kg (infuse over 1 h) IV q8h for 14-21 d Dr. RS MEHTA, MSND, CON 22
- 23. 2. Foscarnet (Foscavir) • Adult • 40 mg/kg IV q8h for 14-26 d 3. Dexamethasone • Adult • 10 mg IV q6h Dr. RS MEHTA, MSND, CON 23
- 24. Managing complications • Signs of hydrocephalus and increased ICP – General measures: Manage fever and pain, control straining and coughing, and avoid seizures and systemic hypotension. – In otherwise stable patients, elevating the head and monitoring neurologic status usually are sufficient. Dr. RS MEHTA, MSND, CON 24
- 25. - When more aggressive maneuvers are indicated, some authorities favor the early use of diuresis (eg, furosemide 20 mg IV, mannitol 1 g/kg IV) provided circulatory volume is protected. Dexamethasone 10 mg IV q6h helps in managing edema surrounding space-occupying lesions. - Hyperventilation (PaCO2 30 mm Hg) may cause a disproportional decrease in cerebral blood flow (CBF), but it is used to control increasing ICP on an emergency basis only. Dr. RS MEHTA, MSND, CON 25
- 26. –Intraventricular ICP monitoring is controversial because some authorities believe dangerous focal edema with a pressure gradient between the temporal lobe and the subtentorial space usually is not detected by the monitor, leading to a false sense of security. In fact, monitor placement may potentially aggravate a pressure gradient. Dr. RS MEHTA, MSND, CON 26
- 27. Follow up 1. Further inpatient care: • Admission of the patient to the hospital, as necessary. 2. Prevention • Immunization against JE is recommended for those traveling into endemic areas during high-risk times of year and this must be explained to the patient Dr. RS MEHTA, MSND, CON 27
- 28. Complications • Seizures • Syndrome of inappropriate secretion of antidiuretic hormone • Increased ICP • Coma Dr. RS MEHTA, MSND, CON 28
- 29. Prognosis • The prognosis depends on the virulence of the virus and on variables associated with the patient's health status, such as extremes of age, immune status, and preexisting neurologic conditions. – – – high rates of mortality and severe morbidity, including mental retardation, hemiplegia, and seizures. Increased mortality and morbidity rates are found in patients who are older than 60 years. Long-term sequelae include behavioral disorders, memory loss, and seizures. Dr. RS MEHTA, MSND, CON 29
- 30. CONTROL • Biological control of natural vertebrate : impractical • Arthropod control : effective method • Personal protection Dr. RS MEHTA, MSND, CON 30
- 31. NURSING ASSESSMENT • Poor personal hygiene • High fever and convulsions • Dehydration • Irritability and restlessness • Baby's parents, anxiety about prognosis, complications & life threatening sequences. Dr. RS MEHTA, MSND, CON 31
- 32. NURSING PRIORITIES The top most Nursing priorities are: 1. Vital status and neurological status 2. Hygienic needs - care of mouth hair and skin. 2. Physical comfort - support of mother(child), calm & clean environment, comfortable position and bed. 3. Nutritional needs - Nutritional balance during illness. 4. Elimination needs - change of soiled linen 5. Safety needs providing bed railings, pads, splinting etc. 6. Special care during fever, fits, lumbar puncture, etc. 7. Communication needs - reassurance and confidence. 8. Psychological and spiritual needs - mental and moral support Dr. RS MEHTA, MSND, CON 32
- 33. NURSING INTERVENTIONS 1. Monitor vital signs and neurological status and record a. Tepid sponging if febrile. b. Hot water bottle if chill c. Attach to nasal oxygen if needed 2.Provide a comfortable bed with pillows or soft pads supported by railings to prevent injuries due to fall. 3. Provide a mackintosh and draw sheet to reduce complications of bed-wetting. 4. Change soiled linens as frequently as needed to avoid bed sores. 5. Provide calm and dim - lighted environment to reduce irritability. Dr. RS MEHTA, MSND, CON 33
- 34. 6. Give morning, evening and bed time care or as required viz. oral hygiene, partial bath, combing and nail cutting to maintain good personal hygiene. 7. Give parentral nutrition as needed & maintain I.V. Infusion / naso gastric tube. 8. Encourage small frequent feeds. Dr. RS MEHTA, MSND, CON 34
- 35. 9. Admit timely attention and aseptic precautions. 10. Administer medicine after checking the orders, labels, etc. under direct supervision to avoid confusions or misuse of drugs. 11. Change the bed linen whenever necessary. Dr. RS MEHTA, MSND, CON 35
- 36. 12. During fever a. Give plenty of oral fluids. b. Maintain fluid balance c. Provide additional warmth by blanket if needed d. Provide proper ventilation. Dr. RS MEHTA, MSND, CON 36
- 37. 13. WHILE CONVULSIONS 1. Apply suction if needed to avoid secretions to block airway, 2. Provide an air way to prevent tongue bite and falling of tongue which blocks the air way. 3. Prefer lateral position for secretions to come out and prevent aspiration. 4. Splint IV line to avoid unnecessary variation in position of canula. 5. Protect the patient from injuries such as chocking, aspiration of vomitus, a fall of head, etc. Dr. RS MEHTA, MSND, CON 37
- 38. 14. During LUMBAR PUNCTURE 1.Follow aseptic precautions. 2.Assist the doctor to do the procedure. 3.Put the patient in lateral position. 4.Have the patient's back arched so that his head almost touch his knees. 5.Collect label and send the specimen promptly. 6.Don't disturb the patient from bed for 24 hours. 7.Elevate foot end of patient after lumbar puncture Dr. RS MEHTA, MSND, CON 38
- 39. 15. Frequently change the position to left lateral & right lateral and give back care. 16. Maintain records of intake, output, vital signs, convulsions (time, frequency, duration, parts included type, etc), drug administration, etc. 17. Explain the patient party about the procedure to relieve anxiety and fear. 18. Provide facilities for daily prayers if desired, allow visitors for particular time without disturbing the patient Dr. RS MEHTA, MSND, CON 39
- 40. ADVICE ON DISCHARGE: 1. Regular medication should be followed. 2. Regular health check-up should be done. Dr. RS MEHTA, MSND, CON 40
- 41. Some Common nursing Diagnosis of the client may be: 1. Altered thought process RT failure in memory and lack of self protective behaviour. 2. Risk for injury RT the unpredictable behaviour and inability to interpret environmental stimuli. 3. sleep pattern disturbance RT alteration in usual sleep habits 4. Altered cerebral tissue perfusion RT increased ICP 5. Impaired verbal communication RT neuronal degeneration. 6. Self care deficit RT loss of memory and motor impairment. 7. Incontinence RT neural degeneration and forgetfulness. Dr. RS MEHTA, MSND, CON 41
- 42. Dr. RS MEHTA, MSND, CON 42
