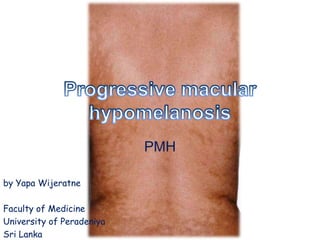
Progressive macular hypomelanosis PMH
•Télécharger en tant que PPTX, PDF•
3 j'aime•4,321 vues
Progressive macular hypomelanosis (PMH) is a common skin disorder that is often misdiagnosed.
Signaler
Partager
Signaler
Partager
Recommandé
Contenu connexe
Tendances
Tendances (20)
Seminar clinical approach to papulosqamous disorders.

Seminar clinical approach to papulosqamous disorders.
Similaire à Progressive macular hypomelanosis PMH
Similaire à Progressive macular hypomelanosis PMH (20)
Dermatology 5th year, 3rd lecture (Dr. Ali El-Ethawi)

Dermatology 5th year, 3rd lecture (Dr. Ali El-Ethawi)
лекция.pptx for std dermatovenerology, cause and symptoms

лекция.pptx for std dermatovenerology, cause and symptoms
Bullous pemphigoid , dermatitis herpitiformis and cbdc

Bullous pemphigoid , dermatitis herpitiformis and cbdc
Plus de Yapa
Plus de Yapa (20)
Assessment of hearing (with self assessment questions).

Assessment of hearing (with self assessment questions).
Foramina and other apertures of cranial fossae and contents

Foramina and other apertures of cranial fossae and contents
Examination of lower limb in neurology-Short case approach for Final MBBS

Examination of lower limb in neurology-Short case approach for Final MBBS
Dernier
Model Call Girl Services in Delhi reach out to us at 🔝 9953056974 🔝✔️✔️
Our agency presents a selection of young, charming call girls available for bookings at Oyo Hotels. Experience high-class escort services at pocket-friendly rates, with our female escorts exuding both beauty and a delightful personality, ready to meet your desires. Whether it's Housewives, College girls, Russian girls, Muslim girls, or any other preference, we offer a diverse range of options to cater to your tastes.
We provide both in-call and out-call services for your convenience. Our in-call location in Delhi ensures cleanliness, hygiene, and 100% safety, while our out-call services offer doorstep delivery for added ease.
We value your time and money, hence we kindly request pic collectors, time-passers, and bargain hunters to refrain from contacting us.
Our services feature various packages at competitive rates:
One shot: ₹2000/in-call, ₹5000/out-call
Two shots with one girl: ₹3500/in-call, ₹6000/out-call
Body to body massage with sex: ₹3000/in-call
Full night for one person: ₹7000/in-call, ₹10000/out-call
Full night for more than 1 person: Contact us at 🔝 9953056974 🔝. for details
Operating 24/7, we serve various locations in Delhi, including Green Park, Lajpat Nagar, Saket, and Hauz Khas near metro stations.
For premium call girl services in Delhi 🔝 9953056974 🔝. Thank you for considering us!Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7![Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
![Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X79953056974 Low Rate Call Girls In Saket, Delhi NCR
Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Escort ServiceModels Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...

Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...GENUINE ESCORT AGENCY
Dernier (20)
Russian Call Girls Service Jaipur {8445551418} ❤️PALLAVI VIP Jaipur Call Gir...

Russian Call Girls Service Jaipur {8445551418} ❤️PALLAVI VIP Jaipur Call Gir...
Top Rated Pune Call Girls (DIPAL) ⟟ 8250077686 ⟟ Call Me For Genuine Sex Serv...

Top Rated Pune Call Girls (DIPAL) ⟟ 8250077686 ⟟ Call Me For Genuine Sex Serv...
Coimbatore Call Girls in Coimbatore 7427069034 genuine Escort Service Girl 10...

Coimbatore Call Girls in Coimbatore 7427069034 genuine Escort Service Girl 10...
Coimbatore Call Girls in Thudiyalur : 7427069034 High Profile Model Escorts |...

Coimbatore Call Girls in Thudiyalur : 7427069034 High Profile Model Escorts |...
Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7![Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
![Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7
Top Rated Hyderabad Call Girls Erragadda ⟟ 9332606886 ⟟ Call Me For Genuine ...

Top Rated Hyderabad Call Girls Erragadda ⟟ 9332606886 ⟟ Call Me For Genuine ...
Call Girls in Lucknow Just Call 👉👉7877925207 Top Class Call Girl Service Avai...

Call Girls in Lucknow Just Call 👉👉7877925207 Top Class Call Girl Service Avai...
Low Rate Call Girls Bangalore {7304373326} ❤️VVIP NISHA Call Girls in Bangalo...

Low Rate Call Girls Bangalore {7304373326} ❤️VVIP NISHA Call Girls in Bangalo...
Call Girls Service Jaipur {8445551418} ❤️VVIP BHAWNA Call Girl in Jaipur Raja...

Call Girls Service Jaipur {8445551418} ❤️VVIP BHAWNA Call Girl in Jaipur Raja...
Independent Call Girls In Jaipur { 8445551418 } ✔ ANIKA MEHTA ✔ Get High Prof...

Independent Call Girls In Jaipur { 8445551418 } ✔ ANIKA MEHTA ✔ Get High Prof...
Call Girls Mysore Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Mysore Just Call 8250077686 Top Class Call Girl Service Available
Call Girl in Indore 8827247818 {LowPrice} ❤️ (ahana) Indore Call Girls * UPA...

Call Girl in Indore 8827247818 {LowPrice} ❤️ (ahana) Indore Call Girls * UPA...
Call Girls Coimbatore Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Coimbatore Just Call 8250077686 Top Class Call Girl Service Available
Premium Call Girls In Jaipur {8445551418} ❤️VVIP SEEMA Call Girl in Jaipur Ra...

Premium Call Girls In Jaipur {8445551418} ❤️VVIP SEEMA Call Girl in Jaipur Ra...
Call Girl In Pune 👉 Just CALL ME: 9352988975 💋 Call Out Call Both With High p...

Call Girl In Pune 👉 Just CALL ME: 9352988975 💋 Call Out Call Both With High p...
Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...

Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...
Russian Call Girls Lucknow Just Call 👉👉7877925207 Top Class Call Girl Service...

Russian Call Girls Lucknow Just Call 👉👉7877925207 Top Class Call Girl Service...
Independent Call Girls Service Mohali Sector 116 | 6367187148 | Call Girl Ser...

Independent Call Girls Service Mohali Sector 116 | 6367187148 | Call Girl Ser...
Call Girls in Delhi Triveni Complex Escort Service(🔝))/WhatsApp 97111⇛47426

Call Girls in Delhi Triveni Complex Escort Service(🔝))/WhatsApp 97111⇛47426
Progressive macular hypomelanosis PMH
- 1. PMH by Yapa Wijeratne Faculty of Medicine University of Peradeniya Sri Lanka
- 2. • Progressive macular hypomelanosis (PMH) is a common skin disorder that is often misdiagnosed. • characterized by ill defined, nummular, symmetrically localized, hypopigmented macules on sebum-rich areas of the skin. • Various authors have written about similar skin disorders, referring to them by different names, but we believe that all these similar disorders are part of the same entity.
- 4. PMH is characterized by 1. Ill-defined nummular, 2. Non-scaly hypopigmented spots on the trunk, 3. Often confluent in and around the midline, 4. Rarely extending to the proximal extremities and neck/head region. 5. There is no itch, pain, or preceding inflammation.
- 5. • PMH has a worldwide distribution; however, it is more often identified in Black people living in or originating from tropical countries. • It is also more often seen in young females. • The natural history of PMH is stable disease or perhaps slow progression over decades, with spontaneous disappearance after mid- life.
- 6. • Extensive pityriasis alba is probably identical with PMH and we suggest discontinuation of use of the former term on the grounds that extensive pityriasis alba is histologically and clinically different from classical pityriasis alba, which is basically an eczematous type of disorder.
- 7. • PMH is characterized histologically by diminished pigment in the epidermis and a normal-looking dermis. • Electron microscopy shows a shift from large melanosomes in normal-looking skin to small aggregated, membrane-bound melanosomes in hypopigmented skin. • PMH should be differentiated from other disorders with hypopigmentation on the trunk such as pityriasis versicolor.
- 8. • We propose that Propionibacterium acnes bacteria living in hair follicles are the cause of PMH as a result of production of a hypothetical depigmenting factor. • This hypothesis is based on: • (i) the presence of a red follicular fluorescence in the hypopigmented spots and the absence of this phenomenon in normal skin when examined under a Wood's light in a dark room;
- 9. • (ii) cultivation of P. acnes from the follicles in the hypopigmented spots but not from follicles in normal-looking skin; and • (iii) improvement of the disorder after elimination of these micro-organisms with topical antimicrobial treatment in combination with UVA light.
- 10. • Currently, the treatment of choice of PMH is application of 1. 1% clindamycin lotion during the daytime, 2. 5% benzoyl peroxide gel at night-time, and 3. UVA light irradiation 3/week for a period of 12 weeks. • There is insufficient information available as yet to comment on the recurrence rate after therapy.
