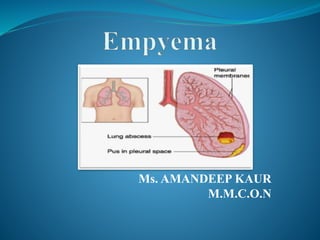
Empyema
- 3. Definition Also known as:- Pyothorax Or Purulent Pleuritis. The word Empyema comes from the greek word Empyein, which means :pus – producing (suppurates). Accumulation of Pus in the Pleural cavity.
- 4. ETIOLOGY EMPYEMA STABBING GUNSHOT WOUNDS ETC. NON TRAUMATIC EXTRATHORACIC SEPSIS THORACIC SEPSIS OSTEOMELITIS MEDIASTINITIS PULMONARY DISEASE PNEUMONIA, TB, BRONCHIECTASIS, LUNG ABCESS NON- IATROGENIC LUNG RESECTION, OESOPHAGEAL TEARS, PARACENTESIS, THORACIS, LIVER BIOPSY IATROGENIC TRAUMATIC SUBPHERANIC ABCESS, HEPATIC ABCESS STERNUM VERTEBRAE RIBS
- 5. ORGANISMS The most common: Staph. aureus .(90% of causes in infants & children) Strept. pneuomonie. H. influenzae
- 6. ETIOLOGY Lung diseases: Pneumonia (the most common cause) Lung abscess. Subphrenic abscess (accumulation of infected fluid between the diaphragm, liver, and spleen) Post traumatic. Post-operative. Blood spread. (post PE) Iatrogenic.
- 7. RISK FACTOR Alcoholism Drug use HIV infection Neoplasm Pre-existent pulmonary disease
- 8. Pathophysiology Presence of Parapneumonic Effusion Release of inflammatory mediators ↑permeability of the capilliaries Attracts WBCs to the site Escape of albumin & other protein from the capillaries ↑ Pleural fluid Presence of Free-flowing, Protein Rich Pleural Fluid (Stage I) Inflammation worsens
- 9. Cont… Attracts more WBCs to the site. Extensive purulent exudate production. Initiation of fibroblastic (collagen and other proteins) activity (Stage II) Adherence of the two pleural membranes (Stage III) Formation of a “Peel”
- 10. CLINICAL STAGES Acute stage : within the first 2 weeks of the onset. Chronic Stage : after 2 weeks or with the formation of the thick peel and loculations.
- 11. Causes of Chronicity: Inadequate Tube Drainage. Chronic pulmonary Disease( T.B. or Fungal Infection) Immuno-supressed patients. Presence of Foreign body within the pleural space.
- 12. SYMPTOMS & SIGNS Fever Cough & Expectoration. Pleuretic chest pain. Easy fatiguability. Loss of weight. Night sweating.
- 13. COMPLICATIONS Rupture into the lung; Broncho-Pleural fistula Spread to the subcutaneous tissue; Empyema Necessitasis) (extension of an empyema outward the pleural cavity.) Septicaemia & septic shock.
- 14. INVESTIGATIONS Chest X-ray. C-T scan. Ultrasonography Thoracentesis
- 15. Light’s criteria Pleural fluid protein: serum protein > O.5 (1-2 g/dL) Pleural fluid : serum LDH >0.6 (Lactate dehydrogenase less than 50% of plasma)
- 16. Other minor criteria Cholesterol > 45mg/dl (< 45 mg/dL). pH <7.2 (7.60-7.64) Glucose < 50% serum (similar to that of plasma)
- 17. Goals of the treatment Treat the infection Drain the purulent effusion adequately and completely Re-expand the lung to fill the pleural space Eliminate complications and avoid chronicity
- 18. Antibiotic treatment As soon as the bacteriologic sample are recovered Pneumonia Amoxicillin, Metronidazole Amox-clavulanic acid Nosocomial Tazobactam or Imipenem Aminoglycoside or Quinolone Adapted to the laboratory results
- 21. Primary treatment options Antibiotics alone; Récurrent thoracocentèsis Insertion of chest drain alone or in combination with fibrinolytics VATS(Video-Assisted Thoracic Surgery). Open decortication:- the operation of removing fibrous scar tissue that prevents expansion of the lung.
- 22. Thoracocentesis Big caliber needle Mostly diagnosis technique Therapeutically used if the liquid remains. Theoretically allows pleural lavage
- 23. Chest Tube As soon as the liquid is thick Localization free: axillary loculated: Chest imaging using ultrasonography and/or computed tomography Size: 20 à 24 Bedside
- 24. Pleural Lavage Isotonic saline Modalités 3 way stopcock Directly through the CT: 250 to 500 ml Cautiously if suspicion of broncho-pleural fistula Timing: Immediately after CT placement Once a day until the liquid is clear
- 25. NOXYFLEX (noxytioline) Local disinfectant (formaldéhyde) 2,5 g diluted in at least 100ml isotonic saline Maximum: 5g/day Incompatible with iodine polyvidone,chlorhexidin, chlorine solution, lactic acid
- 26. Fibrinolytics Urokinase: 100 000 or 300 000 IU conditioning Streptokinase: 250000 IU conditioning 250.000 IU in 10-20 ml isotonic saline Don’t evacuate before 24 to 48 heures Constantly associated with fever (38-39°C) Then evacuate Pleural lavage clamp 4h ( Chest 1996)
- 27. Video-assisted thoracic surgery Collection<10 cm: unusual Visual control of the CT position 5 mm introducer, 4 mm optical Collection>10 cm 10 mm introducer Two or three ports are made in the chest One port is utilised for the camera and the others for grasping instruments Free fluid is evacuated and loculations drained under thoracoscopic visualisation. Fibrinous adhesions are separated and the pleural debris removed from the pleural lining using endoscopic grasping forceps or by extensive irrigation and suction. Following the procedure, one or two chest drains are then placed in the portholes.
- 28. Local antibiotics Usually Rifampin or Colimycin Still debated Do not replace systemic treatment
- 29. Physiotherapy Key to a correct evolution After CT removal Often and for a long time….. Decrease surgery Decrease long term pain and functionnal limitations
- 30. Complications Pleural thickening Reduced lung function
- 31. Nursing Diagnosis Impaired Gas Exchange r/t compressed lung Acute Pain r/t infection of the pleura Risk for Activity Intolerance r/t hypoxia secondary to empyema