Contenu connexe
Similaire à Intra-cellular cocco-bacilli
Similaire à Intra-cellular cocco-bacilli (20)
Plus de Najla El Bizri (8)
Intra-cellular cocco-bacilli
- 1. RESEARCH POSTER PRESENTATION DESIGN © 2012
www.PosterPresentations.com
Our case was that of a CVC-related bacteremia, that persisted for 24
hours along, in a woman without predisposing factors, where intra-
and extra-cellular cocco-bacilli where discovered on the peripheral
blood smear, and where blood culture grew both Acincetobacter
Baumannii and Enterobacter Cloacae. To the best of our knowledge,
no previous data have yet reported the intracellular occurrence of
either cited organisms in a peripheral blood smear, even in patients
having a CVC. Interpretation of this finding should be careful as
bacteria should be distinguished from artifacts and intracytoplasmic
structures (Barr bodies, Howell-Jolly bodies and Döhle bodies) 2.
bpm: beats per minute; CVC: central venous catheter ;
EDTA: ethylenediaminetetraacetic acid ; ESR: erythrocyte sedimentation rate ;
HPF: high power field
1. Free and intracellular bacteria on peripheral blood smears: an uncommon situation related to an adverse prognosis.
J. Gérard1E. Lebas2A. Godon1O. Blanchet1F. Geneviève1A. Mercat2M. Zandecki1Ann Biol Clin 2007 ; 65 (1) : 87-91
2. Infectious diseases manifested in the peripheral blood smear Steven H. Kroft, MD CLINICS IN LABORATORY MEDICINE
VOLUME 22 • NUMBER 1 • MARCH 2002
3. Pneumococcal Bacteremia Diagnosed by Peripheral Blood Smear in Multiple Myeloma Marshall R. Posner, MD; Steven
L. Berk, MD; Peter A. Rice, MD (Arch Intern Med 138:1720-1721, 1978)
4. Overwhelming Neonatal Septicemia Diagnosed Upon Examination of Peripheral Blood Smears Dena M. Selby, MD*|,
Ghislaine Gautier, MTf, Naomi L.C. Luban, MD*'^t. Joseph M. Campos, PhD*t Vol.29 No. 12 CLINICAL PEDIATRICS
5. Gram negative septicaemia diagnosed on peripheral blood smear appearances A Fife, D Hill, C Barton, P Burden Jf
Clin Pathol 1994;47:82-84
6. Intracellular Bacteria in Blood Smears in Patients With Central Venous Catheters. Emina Torlakovic, MD; Jonathan R.
Hibbs, MD; Jeffrey S. Miller, MD; Craig E. Litz, MD Arch Intern Med. 1995;155:1547-1550
7. Candida albicans blastoconidia in peripheral blood smears from non-neutropenic surgical patients. Y Berrouane, H
Bisiau, F Le Baron, C Cattoen, P Duthilleul, E Dei Cas J Clin Pathol 1998;51:537-538
8. Bacteria in Blood Smears: Overwhelming Sepsis or Trivial ContaminationW. van der Meera J.M.M. Verwielb C.E.M.
Giddingc M. de Metzd M.H. de Keijzera. Departments of aClinical Chemistry, bPediatric Intensive Care, cPediatric
Oncology, University Medical Center St. Radboud Nijmegen, and dDepartment of Clinical Chemistry, Canisius
Wilhelmina Hospital Nijmegen, The Netherlands Acta Haematol 2002;107:220–223
9.Overwhelming Pneumococcal Bacteremia Revealed by a Peripheral Blood Smear In a 74-year-old Healthy Woman
Hideta Nakamura1,3, Manabu Saitou 2, Shunichi Kinjo 1, Hiroshi Kaneshima1, Futoshi Higa 3, Masao Tateyama3 and
Jiro Fujita DOI: 10.2169/internalmedicine.46.6032
10.Bacteremia Detected by a Peripheral Blood Smear in a Pediatric Surgical Patient with Thrombocytopenia Jeong Tae
Kim1, Jae Hyeon Lee1, Hye Soo Lee1,3,4, Yong Gon Cho1,3,4, Dal Sik Kim1,3,4,Sam Im Choi1,3,4, Soo Chul
Cho2,3,4Korean J Clin Microbiol Vol. 13, No. 4, December, 2010 DOI: 10.5145/KJCM.2010.13.4.182
11. Blood smear: fulminant pneumococcal bacteremia. Jonathan Lancashire and Mark Crowther Blood 2012 120: 4459
BLOOD, 29 NOVEMBER 2012 _ VOLUME 120, NUMBER 23
12. Rapid diagnosis of central-venous-catheter-related bloodstream infection without catheter removal. Kite P,
Dobbins BM, Wilcox MH, McMahon MJ: Lancet 1999;354:1504–1507.
LIST OF ABBREVIATIONS
The finding of bacteria in routinely prepared peripheral blood film is
an uncommon phenomenon in the hematology laboratory. Their
presence is associated either to infection, usually overwhelming sepsis
or artifact. In this report, we describe a case of a central venous-
related bacteremia in a previously healthy, immunocompetent,
asymptomatic young woman, where intra- and extra-cellular cocco-
bacilli where incidentally discovered on a peripheral blood smear, and
blood culture were positive for Acincetobacter Baumannii and
Enterobacter Cloacae. To the best of our knowledge, no previous data
have yet reported the intracellular occurrence of either cited
organisms in a peripheral blood smear, even in patients having a
central venous catheter. We recommend careful interpretation of
bacterial finding in a peripheral film. Their presence in a patient with
a central venous catheter usually points to an active infection. We
recommend that central venous catheters be removed in such
patients, even if the patient is asymptomatic.
ABSTRACT
CASE REPORT
We reviewed 10 articles published from 1978 to 2012 and enumerated
20 cases reporting the finding of infectious organisms in the peripheral
blood smear (Table 1).
The M: F ratio was 11:9. Ages ranged from neonatal age to 80 years
old. Among the 20 patients, 16 had an underlying condition, 9 were
immunocompromised (ANC <1.500) and 10 had a central-venous
catheter. In 11 cases, there was a clinical suspicion of sepsis. Prior
antibiotic treatment before the PBS finding was documented in 4
cases; no antiobiotherapy in 4, and in the other 8 cases, it was not
mentioned. 10 cases were diagnosed as septicemia, 9 as CVC-related
bacteremia and 1 as an in-vitro contamination. 10 patients recovered
and 10 had a fatal outcome.
A previously healthy, 27-year-old woman was admitted to Rafik Hariri
University Hospital in Beirut because of polytrauma. Upon admission,
the patient was conscious, poorly oriented, in pain. She was
hypotensive (blood pressure 110/70 mmHg), tachycardic (heart rate 77
bpm), and afebrile (oral temperature 36.5°C).
On physical exam, the lungs were clear to auscultation, the cardio-
vascular exam unrevealing, and there was no acute abdomen. The
neurological exam was intact with lack of cooperation due to pain. A
scalp laceration was noted, as well as multiple right upper and lower
limbs closed fractures with no vascular or neurological deficits.
A CVC in the left internal jugular vein was placed and a Foley catheter
inserted. Laboratory tests revealed anemia (hemoglobin 8.1 g/dl;
hematocrit 23.9%) with no other abnormalities. Imaging studies
revealed the presence of a massive scalp hematoma not associated
with skull fracture, a Montaggia fracture of the right forearm, right
tibial and fibular fractures. A mild left hemothorax and fractures of the
10th and 11th ribs were also present.
Tetanus immune globulin was administrated intramuscularly for
tetanus prophylaxis. Aggressive hydration and transfusion of two
packed red blood cells units and two fresh frozen plasma units were
administered in an attempt to avoid progression to hemorrhagic shock
(hemoglobin: 6.9 g/dl after 6 hours). No transfusion reaction was
observed neither during nor after the transfusion. The scalp
hematoma was evacuated, and the fractures were managed
conservatively awaiting definitive surgical treatment. According to the
emergency room protocol, she was started on amoxicillin clavulanate
as prophylaxis.
For 11 consecutive days, the patient was clinically stable, oriented,
afebrile, complaining only of pain over fracture sites. She was
bedridden on a water mattress with frequent positioning and having
insentive spirometry. Low molecular weight heparin was administered
for deep venous thrombosis prophylaxis. Foley catheter care with
povidone-iodine topical antiseptic was regularly performed. Her
laboratory tests were unremarkable during this period with no further
need for transfusion. Amoxicillin clavulanate was continued for seven
days then was switched to ceftizoxime.
On the 12th day of admission, while the patient was still afebrile, a
follow-up blood drawn at 7 am from the central venous catheter in an
EDTA tube revealed a total white blood cell count of 8.5 109/L with
58% neutrophils. ESR from the same sample was 91 mm/hour. Because
of the relatively high monocyte count on the automated counter, a
Giemsa/Wright-stained blood smear was performed for manual
differential count. No abnormal cell findings were observed, however,
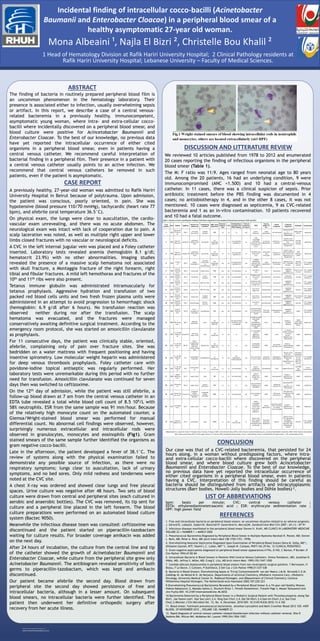
surprisingly numerous extracellular and intracellular rods were
observed in granulocytes, monocytes and eosinophils (Fig1). Gram
stained smears of the same sample further identified the organisms as
gram negative cocco-bacilli.
Late in the afternoon, the patient developed a fever of 38.1°C. The
review of systems along with the physical examination failed to
demonstrate any possible source of infection, as there were no
respiratory symptoms; lungs clear to auscultation, lack of urinary
symptoms, and no bed sores. Only mild redness and tenderness were
noted at the CVC site.
A chest X-ray was ordered and showed clear lungs and free pleural
spaces. Urine culture was negative after 48 hours. Two sets of blood
culture were drawn from central and peripheral sites (each cultured in
aerobic and anaerobic bottles). The CVC was removed, its tip sent for
culture and a peripheral line placed in the left forearm. The blood
culture preparations were performed on an automated blood culture
system (Bactec 9050).
Meanwhile the infectious disease team was consulted: ceftizoxime was
discontinued and the patient started on piperacillin-tazobactam
waiting for culture results. For broader coverage amikacin was added
on the next day.
After 24 hours of incubation, the culture from the central line and tip
of the catheter showed the growth of Acinetobacter Baumannii and
Enterobacter Cloacae, while culture from the peripheral site grew only
Acinetobacter Baumannii. The antibiogram revealed sensitivity of both
germs to piperacillin-tazobactam, which was kept and amikacin
discontinued.
Our patient became afebrile the second day. Blood drawn from
peripheral site the second day showed persistence of free and
intracellular bacteria, although in a lesser amount. On subsequent
blood smears, no intracellular bacteria were further identified. The
patient then underwent her definitive orthopedic surgery after
recovery from her acute illness.
1 Head of Hematology Division at Rafik Hariri University Hospital; 2 Clinical Pathology residents at
Rafik Hariri University Hospital; Lebanese University – Faculty of Medical Sciences.
Mona Albeaini ¹, Najla El Bizri ², Christelle Bou Khalil ²
Incidental finding of intracellular cocco-bacilli (Acinetobacter
Baumanii and Enterobacter Cloacae) in a peripheral blood smear of a
healthy asymptomatic 27-year old woman.
REFERENCES
CONCLUSION
DISCUSSION AND LITTERATURE REVIEW