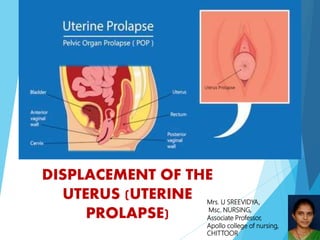
Displacement of uterus
- 1. DISPLACEMENT OF THE UTERUS (UTERINE PROLAPSE) Mrs. U SREEVIDYA, Msc. NURSING, Associate Professor, Apollo college of nursing, CHITTOOR
- 3. The uterus has central position in the pelvis The external Os is at the level of the ischial spine It is ante verted & ante flexed
- 4. Prolapse of the uterus refers to the downward displacement of the vagina and uterus.
- 5. It is one of the common clinical condition met in day to day gynecological practice It is most often seen in multiparous women. It is a form of herniation Uterine prolapse can happen to women of any age, but it affects post menopausal women who had one or more vaginal deliveries. The incidence of prolapse is about one in 250 pregnancies.
- 6. Uterine prolapse occurs when pelvic floor muscles and ligaments stretch and weaken, providing inadequate support for the uterus . The uterus then slips down into or protrudes out of the vagina. Weakening of the pelvic muscles that leads to uterine prolapse can be caused by: 1) Damage to supportive tissue during pregnancy and child birth 2) Effects of gravity 3) Loss of oestrogen
- 7. Round ligaments Broad ligaments Pubocervical ligaments Pelvic floor muscles Utero sacral ligaments
- 8. Uterine prolapse means the uterus has descended from its normal position in the pelvis farther down into the vagina. Uterine prolapse is a form of female genital prolapse. It is also called pelvic organ prolapse or prolapse of the uterus (womb).
- 11. 1. Congenital – At birth 2.Acquired – During Labour 1-Bearing down 2-Forceps delivery 3- Traction on cord 4- Breech extraction before fully dilatation
- 12. During puerperium Lack of exercises and bodily weakness Others: Repeated deliveries or child birth
- 13. 1. Increase in intra - abdominal pressure Abdominal mass Ascitis Chronic cough, constipation 2. Obesity 3. Uterine fibroid
- 14. 1. Uterovaginal prolapse: It is the prolapse of uterus, Cx & upper vagina. Commonest type It is accompanied by Cystocele. 2. Congenital prolapse: No cystocele Often seen in nulliparous, so called as nulliparous prolapse. Cause-congenital weakness of supports of Uterus.
- 22. 1.In first-degree prolapse- The uterus descends down from its anatomical position (external os at the level of ischial spines) but the external os still remains inside vagina. 2. In second-degree The external os protrudes outside the vaginal introits but the uterine body still remains inside the vagina. 1 2 3 4
- 24. 3. In third-degree prolapse or total prolapse or procidentia- The uterine cervix and body descends to lie outside the introitus. It is also known as Procidentia OR complete prolapse. 4. In fourth degree or complex prolapse- Prolapse of the uterus with eversion of entire vagina. It is inevitably associated with cystocele and an enterocele.
- 25. Feeling of something coming down per vaginum specially while she is moving Backache or Dragging pain in the pelvis Dysparenunia
- 26. Difficulty in passing urine, more lessthe sternous effort evacuation. Incomplete evacuation Urgency or frequency of micturation The woman difficulty in may experience passing stools and complete evacuation of bowels.
- 27. utero-vaginal prolapse may be visible during inspection of the vulva. In case of minor prolapse it may become visible on straining. Rectal examination also differentiate between rectocele and enterocele.
- 28. Pelvic examination Both dorsal & standing positions. The patient is asked to strain , this helps to demonstrate a prolapse which may not be seen at rest
- 29. Hematology Rectal exam Pelvic exam USG X-ray MRI
- 30. Cystic swelling in the vagina Chronic inversion of the uterus Hypertropy of the cervix
- 32. Adequate antenatal & intranatal care To avoid injury to the supporting structures during the time of vaginal delivery Adequate postnatal care To encourage early ambulance To encourage pelvic floor exercises General measures To avoid strenuous activities- heavy lifting To avoid pregnancies too soon
- 33. Oestogen replacement therapy Kegal exercise Pessary treatment A vaginal pessary is an object inserted into the vagina to hold the uterus in place.
- 34. Early cases of UV prolapse are helped by pelvic floor exercises Particularly during puerperium and while waiting to undergo surgical treatment. Kegel exercises are used to tone up pelvic musculature These exercises are done 3 times a day for 20 min each. Kegal exercises
- 37. A mechanical device for correcting and controlling UV prolapse A pessary does not cure UV prolapse It only holds the genital tract in position Advised for patients who cannot undergo surgery Types 1.Ring pessary 2.Hodge pessary
- 38. Indications During pregnancy (1st trimester) During puerperium Unfit for surgical treatment Patient’s choice
- 39. Management Choice of pessary ( ring pessaries commonly used) Select the Size (depends upon size of vagina) Sterilize the pessary Insertion- before insertion of the pessary, it is to be kept in hot water for few minutes so that pessary become soft and easy to insert Follow up pessary should be removed ,cleaned and reinserted at regular intervals of 6-12 months.
- 41. Surgery should wait until symptoms are worse than the risks of having surgery. The surgical approach depends on: Degree of prolapse Desire for future pregnancies Often, a vaginal hysterectomy is used to correct uterine prolapse.
- 42. Vaginal Hysterectomy – most common operation and its indications are: - Post-menopausal prolapse -Uterine pathology like small fibroids or adenomyosis -Menstrual disorders such as dysfunctional uterine bleeding -Prolapse during childbearing age , after completion of family Burch Operation – for relief of symptoms of cystocele.
- 43. Anterior Colporrhaphy – for anterior vaginal wall prolapse. Posterior Colporrhaphy – for repair of the posterior vaginal wall and perineum. Manchester Repair (Fothergill’s Operation) – for repair of uterovaginal prolapse. Carried out in women of child bearing age and haven’t completed their families and insist on preservation of uterus
- 45. a)To assess the level of pain, cause, location, intensity to get base line data b)To provide comfortable position to the patient to relieve discomfort i.e. lying down position c)To provide diversion therapy to the patient to divert the mind of the patient d)To provide analgesics to patient as prescribed by physician to relieve pain.
- 46. a) To assess the signs & symptoms of infection. b) To assess the vital signs of the patient c)To encourage the patient not to touch the prolapsed area with unclean hands. d) Provide prescribed antibiotics to patient
- 47. a) Explain all treatment and procedures b) Encourage verbalization of feelings by patient and family c) Provide information on treatment modalities.
- 48. 1)Dutta D.C 'Textbook of obstetrics' 6th edition published by new book agency (P) limited pp -312-313,421-422. 2)Jacob annamma ‘a comprehensive textbook of midwifery ‘1st edition published by jitender p vij pp 539- 55 3) www.Google.com